Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com
No texting or chat messages, please. Ordinary e-mails are welcome.

|

|
 |
 |
 |
 |
|
verify here. |
Cyberfriends: The help you're looking for is probably here.
This website collects no information. If you e-mail me, neither your e-mail address nor any other information will ever be passed on to any third party, unless required by law.
This page was last modified January 1, 2016.
I have no sponsors and do not host paid advertisements. All external links are provided freely to sites that I believe my visitors will find helpful.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected. No texting or chat messages, please. Ordinary e-mails are welcome.
 I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
 If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

|
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource.
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
pathology.org -- my cyberfriends, great for current news and browsing for the general public
EnjoyPath -- a great resource for everyone, from beginning medical students to pathologists with years of experience
Medmark Pathology -- massive listing of pathology sites
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm still handling dozens of requests for information weekly, all as a public service.
Pathology's modern founder, Rudolf Virchow M.D., left a legacy of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of all the make-believe and bunk that interfere with peoples' health, reasonable freedom, and happiness. I talk and write straight, and without apology.
Throughout these notes, I am speaking only for myself, and not for any employer, organization, or associate.
Special thanks to my friend and colleague, Charles Wheeler M.D., pathologist and former Kansas City mayor. Thanks also to the real Patch Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:

My home page
More of my notes
My medical students
Especially if you're looking for information on a disease with a name that you know, here are a couple of great places for you to go right now and use Medline, which will allow you to find every relevant current scientific publication. You owe it to yourself to learn to use this invaluable internet resource. Not only will you find some information immediately, but you'll have references to journal articles that you can obtain by interlibrary loan, plus the names of the world's foremost experts and their institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review. If you are interested in complementary medicine, then I would urge you to visit my new Alternative Medicine page. If you are looking for something on complementary medicine, please go first to the American Association of Naturopathic Physicians. And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I do not accept donations, though I appreciate those who have offered to help.
During the eighteen years my site has been online, it's proved to be one of the most popular of all internet sites for undergraduate physician and allied-health education. It is so well-known that I'm not worried about borrowers. I never refuse requests from colleagues for permission to adapt or duplicate it for their own courses... and many do. So, fellow-teachers, help yourselves. Don't sell it for a profit, don't use it for a bad purpose, and at some time in your course, mention me as author and William Carey as my institution. Drop me a note about your successes. And special thanks to everyone who's helped and encouraged me, and especially the people at William Carey for making it still possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
OBJECTIVES
The student will order, perform, and interpret chemical and microscopic urinalyses when appropriate, avoiding all the common pitfalls.
The student will correctly instruct patients and allied health personnel in the collecting of urine specimens.
QUIZBANK
Microscopy (all)
|
|
Nice review of the whole business: Am. Fam. Phys. 71: 1153, 2005.
SPOT URINE COLLECTION
You will frequently order tests on random, timed, and 24-hour urine specimens.
Since the chemical urinalysis is so easy, you'll perform it frequently in your practice. Counting the labor and reagents, it's $0.65 per test.
I'd recommend a chemical urinalysis on everybody who has any symptoms suggesting kidney ("Uh, I just don't feel well lately") or bladder disease, and anyone you don't know well or who's sick without an obvious cause (you don't want to miss glomerulonephritis, endocarditis, or pyelonephritis, Doc... Br. Med. J. 301: 329, 1990).
Screening aims to find treatable disease without excessive risk or cost of workups for false-positives.
When there are no symptoms, it seems reasonable to do a chemical urinalysis on a kid before he/she enters school (Pediatrics 100: 919, 1997); more frequent checking of children just generates costs by forcing you to do more tests that almost never turn up anything important.
The fad for screening kids for (and giving long-term antibiotics for) asymptomatic bacteriuria seems to be over (thankfully). Whether all pregnant women (even those with normal urinalysis) should have routine urine cultures for asymptomatic bacteriuria remains under discussion (Am. J. Ob. Gyn. 182: 1076, 2000).
You are already familiar with the emphasis on obtaining midstream urine, especially for culture. See Appendix I for instructions (you can copy it for patients).
Acrobatic skill is required, especially for women. There has always been skepticism, and most recently, just getting a midstream clean-catch seems to give as good results as anything more elaborate (Arch. Int. Med. 160: 2537, 2000).
To collect urine from incontinent adults, try sealing on an ileostomy bag (see Lancet 2: 394, 1982).
Squamous epithelial cells in the urinary sediment indicate contamination from the genital tract, making interpretation a problem. (Sometimes the vagina must be packed, or a tampon used.)
Opinions vary regarding the best urine to "spot-check".
First morning-voided specimens are best for checking ability to concentrate urine, and for nitrite and protein.
Formed elements in the sediment may be more numerous in the first morning-voided specimen, but will be better preserved in subsequent specimens. (This is especially important if you are sending some urine for cancer cytology.)
It is better if urine sent for bacterial counts, etc., has not "incubated" so long in the bladder.
* Diabetics still sometimes check their urine for glucose after meals, or to validate their blood results. This isn't a bad idea (J. Fam. Pract. 34: 495, 1992).
Regardless of what sample you send, it must reach the lab within an hour or two to yield useful results.
Bacteria multiply at an astonishing rate, and will convert glucose to acids rapidly. (Urea splitters will produce a strongly alkaline urine.)
Formed elements will lyse within a few hours whether or not there is infection, especially if the urine is hypotonic.
* Preservative tablets are available if the urine must stand around for a while (i.e., when a group of people are being screened as for insurance). These release mercury (which is bad for the environment) and formaldehyde. Refrigeration can also keep the specimens fresh for a few hours.
TWENTY-FOUR HOUR URINE COLLECTION
Obtaining a complete 24-hour urine collection requires cooperation from all concerned. Instructions like the set in Appendix I can make all the difference.
The lab can check the total urine creatinine to estimate whether the specimen is really complete. This works pretty well.
Choice of preservative for such a collection depends entirely on what you are planning to measure.
NO PRESERVATIVES OR REFRIGERATION is necessary if you are only planning to assay for heavy metals or * estriol. (Ask about a lead-free glass container if you are going to measure urinary lead excretion.)
REFRIGERATION ONLY is enough for amylase, hCG, total protein, Bence-Jones protein, electrolytes, most drugs of abuse.
SODIUM CARBONATE (5 gm) and PROTECTION FROM LIGHT are required for all porphyrin studies.
* HYDROCHLORIC ACID (15 mL) is recommended for delta-amino levulinic acid, calcium, and phosphorus.
GLACIAL ACETIC ACID (*15 mL) is recommended for most steroids and catecholamine metabolites.
* BORIC ACID (15 gm) is recommended for uric acid, creatinine, proteins (if mailed), amino acids, 5'-HIAA, and a few steroids (estradiol, cortisol).
* Defense attorneys will attribute alcohol in the urine to fermentation by yeast; you can rule this (silly) defense out by using fluoride for your collection kit (J. For. Sci. 38: 266, 1993).
CHEMICAL URINALYSIS
DIPSTICKS:
Today, the color and odor (if any) of the urine are noted, and the urine chemistries are performed using a reagent strip, with pads that change color ("Multistix" or "Chemstrip").
These are easy to use. Be sure to swirl the urine before dipping the stick, keep your fingers off the pads, and don't leave the strip in too long or allow the dyes to run.
Store the sticks at room temperature, in their light-proof bottle, with the lid on tight and the desiccant in place. The first pad to be damaged by improper storage is the important ketone pad.
* The 1980's brought us first an office dipstick-reading machine (such technology!), then machines to do the microscopic urinalysis as well (yesterday's Yellow IRIS, today's flow cytometers Sysmex UF-50 and UF-100, and now the Iris iQ200: Am. J. Clin. Path. 129: 445, 2008; Am. J. Clin. Path. 133: 577, 2010). The latter do a pretty good job and once the initial investment is made, they're faster than using your own eyeballs and microscope. However, if the sediment really matters (i.e., you are looking for red cell casts), there's still no substitute for a human examiner. See Am. J. Clin. Path. 112: 25, 1999; Am. J. Clin. Path. 115: 605, 2001; update Arch. Dis. Child. 95: 103, 2010).
APPEARANCE (colors South. Med. J. 105: 43, 2012)
The familiar yellow color of concentrated urine is due to "urochrome" porphyrins.
"Amber" urine: conjugated bilirubin
Red urine: hemoglobin (blood, free), myoglobin, porphyria, drugs (phenolphthalein, deferoxamine, some phenothiazines), beets / blackberries (some people's metabolism or if they've taken foods rich in oxalate), malingerer adding food coloring to fake a kidney stone
Smoky/brown urine: altered blood (* acid hematin), alkaptonuria (turns brown on standing), melanin (i.e., disseminated melanoma), * rhubarb (some people, alkaline urine), * cascara (some people)
Dark orange urine: drugs (pyridium, rifampin, really overdoing that riboflavin from the health food store, others). Bright blue urine: drugs (methylene blue, others). Fluorescent yellow: Overpriced vitamins. Don't dipstick these urines, as the colors won't turn out right.
Green urine is usually an idiopathic response to medication (Clin. Tox. 46: 485, 2008). Really overdoing the "Clorets" breath mints can turn urine green. Fluorescent green urine is a marker for having drunk antifreeze.
Purple urine is usually seen in the foley bag of someone in a nursing home who's also constipated. It's probably a bacterial product from the gut perhaps reacting with the plastic in the bag. Nobody's figured it out yet.
Foamy urine: proteinuria, conjugated bilirubin, pyridium
Turbid/cloudy urine: WBC's, urates, phosphates; very rarely a lymphatic fistula or very heavy proteinuria
Fat globules on the surface: fat embolization
ODOR: Limited usefulness.
Ammonia: Urea-splitting organisms.
* Asparagus: Autosomal dominant, methanethiol (Experientia 43: 382, 1987, such science!)
SPECIFIC GRAVITY
Healthy folks can concentrate their urine to SG 1.030 and dilute to SG 1.003.
This may be "determined" using a hygrometer, refractometer, osmometer (best, the lab might have one), or an electrolyte-sensitive pad on some "dipstick" reagent strips. (The strips really measures ionic strength, and is really a pretty good screen.) Generally, a low or high specific gravity proves good tubular function.
Specific gravity closely approximates osmolality, which is what you're really concerned about. This works except with x-ray contrast media or very high concentrations of glucose, or in babies (J. Ped. 108: 613, 1986; J. Ped. Surg. 21: 580, 1986).
HYPOSTHENURIA: specific gravity less than 1.007. Think of diabetes insipidus, fluid loading.
ISOSTHENURIA: specific gravity fixed at 1.010. Think of renal tubular dysfunction; if oliguria is also present, think of acute tubular necrosis.
Checking the specific gravity is a good way of proving to stone-formers that they aren't drinking enough water: J. Urol. 146: 1475, 1991.
pH / ACIDITY-ALKALINITY
This is determined by the color change of an indicator on the reagent strip. It is of limited usefulness.
* Urine pH reflects metabolic adjustments, and checking urine pH can detect renal tubular acidosis, currently a popular diagnosis among clinicians.
Normally, urinary pH rises after a meal (alkaline tide) because the parietal cells of the stomach pump alkali into the bloodstream. Surgeons can even use this to see if the vagotomy worked.
Strongly alkaline urine usually indicates urea-splitting by Proteus (* occasionally Pseudomonas, others).
* Grunge in acid urine is uric acid crystals; grunge in alkaline urine is calcium phosphate crystals. (No big deal!)
PROTEIN (Am. Fam. Phys. 82: 645, 2010)
This is measured using the protein error of indicators. Normal adults lose up to 150 mg/24 hr. Office workup of proteinuria: Am. J. Med. Sci. 320: 188, 2000.
Dipstick approximations:
negative... 0-50 mg/L
trace... 50-150 mg/L
1+... 150-300 mg/L
2+... 300-1000 mg/L
3+... 1-3 gm/L
4+... >3 gm/L
If you want to assume that your patient puts out 1 L of urine per day, these equate to the daily protein output. If you drink a lot of water, you may have nephrotic-range proteinuria but show only minimal proteinuria on dipstick. If it really matters (i.e., pre-eclampsia), do a 24-hour urine (if you can; Am. J. Ob. Gyn. 170: 137, 1994). Savvy pathologists and clinicians today prefer a protein/creatinine ratio, which make the 24-hour collection unnecessary (we suggest using the first-voided morning urine, please do this before calling the nephrologist: Mayo Clin. Proc. 84: 180, 2009).
False positives for protein are caused by highly alkaline or highly buffered urine. Remember hemoglobin and vaginal secretions as sources of protein.
Proteinuria is the single most sensitive indicator of most renal disease, though of course it is not specific.
Nephrotic syndrome (selective proteinuria is better than nonselective), nephritic syndrome, tubular disease ("tubular proteinuria", largely beta2m, will not exceed about 1.5 gm/day), urinary tract infections and tumors.
You can have proteinuria quantitated (ask for "24 hr. quantitative protein"), checked for "selectivity", etc.
Macroalbuminuria, not nephrotic range: 300-3500 mg/day or mg / gram of creatinine. Consider checking first for orthostatic proteinuria. Do a urine protein electrophoresis so as not to miss plasma cell myeloma. It may be due just to having a fever, or exercising, or maybe you'll never find a cause.
In the current era of intensive screening for diabetic proteinuria in order to institute therapy to prevent diabetic glomerulopathy (i.e., ACE-inhibitor; good stuff Ann. Int. Med. 118: 577, 1993), even the "trace" reading on the pad on the dipstick isn't sensitive enough. You'll want to quantify by other techniques (Hosp. Pract. 28(3): 129, March 15, 1993; Arch. Path. Lab. Med. 115: 34, 1991).
Of course, lots of things beside kidney disease can cause proteinuria.
Postural proteinuria (orthostatic, etc.): 3-5% of healthy children and young adults pass excess protein during the day, not at night.
Functional proteinuria (albuminuria): occurs with fever, cold exposure, stress, pregnancy, eclampsia, CHF, shock, severe exercise (persists up to 3 days following. See JAMA 253: 236, 1985.) Immediate investigation of "trace proteinuria", especially during acute illness, is not worthwhile; however, long-term it's a pretty good indicator that something's seriously wrong with the body (check the first AM sample: Br. Med. J. 304: 1196, 1992).
Bence Jones globulin: plasma cell myeloma, macroglobulinemia, lymphoma. Reagent strips for protein miss it. Ask for a urine protein electrophoresis.
If proteinuria persists, then check for azotemia and quantitate the protein. If there's azotemia and/or more than 2 gm is lost daily, it's time for a nephrology workup.
Of course, simply finding your protein in the end-of-the-day specimen and no protein in the just-got-out-of-bed sample clinches the diagnosis of orthostatic proteinuria.
GLUCOSE
The reagent strip method uses glucose oxidase and is very sensitive and specific.
False negatives can result from megadose vitamin C. (Lots of people are on megadose vitamin C. See Clin. Chem. 38: 426, 1992).
False positives (trace to +1) can result from the dipstick jar being left uncapped for a few days (Am. J. Clin. Path. 96: 398, 1992). Since the test is based on oxidation, strong false-positives will result in the presence of hypochlorite bleach ("I collected the urine in my empty 'Clorox' bottle", etc.) Tetracycline can also give a false negative.
KETONES (acetoacetic acid and acetone; strips do not detect beta-hydroxybutyrate)
* The reagent strip uses the nitroprusside reaction.
These reagents are especially vulnerable to improper storage (heat, uncapped bottle).
False positives result from L-DOPA metabolites (Rx for Parkinson's disease), * phthalein dyes (BSP, Ex-lax), and people with cystinuria (stones, remember?).
Miss a meal, and you are likely to show mild ketonuria. Large amounts indicate diabetic ketoacidosis or aspirin poisoning, and detecting these makes the test worthwhile.
BLOOD
The reagent strips detect peroxidase from blood, and are as sensitive as microscopy (Br. J. Urol. 58: 211, 1986). However, they are infamously nonspecific, and are often strongly positive apparently for no reason whatever.
Hematuria is "microscopic" if the urine isn't red but the urinary sediment contains more than about 5 red cells per high power field.
In younger people with microscopic hematuria who have otherwise-normal labs and no signs or symptoms, further workup is unlikely to yield any useful information. A lot of these people will turn out to have thin-GBM non-disease. Only a few will have troubles later (JAMA 306: 729, 2011).
In older folks, of course, microscopic hematuria is your warning about kidney / bladder cancer.
* Some microscopic hematuria is attributed to hypercalciuria, i.e., the oxalate crystals injury the bladder mucosa.
Positives also result from hemoglobinuria (intravascular hemolysis), and myoglobinuria (crush injury, electrocution, rhabdomyolysis). Hypochlorite bleaches (that "Clorox" bottle again) produce a false positive.
False negatives result from megadose vitamin C, leaving the lid off the dipstick jar for a few days (Am. J. Clin. Path. 96: 398, 1991) or formaldehyde. Intact RBC's supposedly will not react, but this seldom or never causes problems.
Hematuria is an important sign of glomerulonephritis, stones, tumors, TB![]() , SBE, coagulopathy,
infection, vasculitis,
schistosomiasis
, SBE, coagulopathy,
infection, vasculitis,
schistosomiasis![]() ,
leptospirosis, etc.
,
leptospirosis, etc.
Checking the urine for blood is THE way to screen older folks for bladder cancer, which is worthwhile.
In the "three-glass" method of checking a man's random urine, blood mostly in the first glass indicates penile urethral bleeding, while blood mostly in the third glass indicates prostatic bleeding. Why?
NITRITE
The presence of nitrite suggests bacterial action (nitrate reduction; notably E. coli and many others; it's worth remembering that the enterococcus does NOT reduce nitrate). The reagent strips detect nitrite by its reaction with an azo dye.
Just how to check people, especially children, for urinary tract infections is a subject of much discussion today.
Especially in kids, routine urinalysis (nitrite, protein, leukocyte esterase) often misses urinary tract infection (J. Fam. Pract. 40: 45, 1995; Arch. Ped. Ad. Med. 155: 60, 2001; Clin. Ped. 39: 461, 2000; Pediatrics 103: 843, 1999; Postgrad. Med. 109: 171, 2001, the last one from the DO's in Michigan). The current recommendation is to tap or catheterize a febrile child who you suspect has a urinary tract infection, even if "urinalysis is normal" (Am. Fam. Phys. 62: 1815, 2000.)
Using a bag to collect urine from a not-yet-toilet-trained kid is so likely to produce a false-positive result that the further interventions required actually place the kid at unjustifiable danger (J. Ped. 137: 221, 2000).
BILIRUBIN
The reagent strips detect conjugated bilirubin (which is the only kind that will show up in the urine) * by a diazo reaction.
* False negatives result from delay in testing the urine (the bilirubin-glucuronic acid bond breaks) or certain drugs. But in this era of cheap chemical profiles, who needs a urinalysis to detect conjugated hyperbilirubinemia?
UROBILINOGEN (remember this is colorless)
* The reagent strips detect urobilinogen by the Ehrlich aldehyde reaction.
Urobilinogen is very labile in acid pH and light, and the reaction is not analytically specific. Increased levels are quite a good way to screen for hemolysis (but other tests for hemolysis are much more sensitive and specific), or hepatocyte dysfunction (still a fairly good screen).
Contrary to widespread belief, this pad is worthless for detecting porphobilinogen (acute intermittent porphyria and others) or uroporphyrin (porphyria cutanea tarda).
LEUKOCYTE ALKALINE ESTERASE on some reagent strips detects polys. It's a pretty good way to pick up a urinary tract infection if you're disinclined to look for WBC's in the urinary sediment (shame on you).
The last decade, with its emphasis on pretending to do everything on the cheap, saw an effort to use dipstick results-only to diagnose and start treatment for urinary tract infections and even urethritis in men. Be VERY cautious, especially if the diagnosis is not obvious on history and physical exam.
Confirmatory tests (for semiquantitative results, or if your are dissatisfied with your reagent strips for some reason)
* Protein: sulfosalicylic acid test. (False-positives result from x-ray contrast media)
Glucose -- "Clinitest", a copper reduction test that detects all reducing sugars. (Good for screening for inborn errors of carbohydrate metabolism, and, since it's a fizzy test-tube test, it is preferred by old-timers who "don't believe in dipsticks").
* Bilirubin -- "Ictotest tablets" (slightly more sensitive, but who cares?)
Future surgeons! You can use dipsticks on peritoneal lavage fluid to decide whether to operate people who have been stabbed in the tummy. Check protein content and white count: Br. J. Surg. 78: 696, 1991.
MICROSCOPIC URINALYSIS (see Arch. Pathol. Lab. Med. 108: 399, 1984, still good)
Shake the urine, pour some into a test tube, spin it down (* 2000 rpm), and resuspend the sediment in 1 mL of urine.
Look at the sediment at high power using phase microscopy, polarized light, or the * Sternheimer stain. Use the supernatant for Bence-Jones protein determination, electrophoresis, sugar chromatography, etc.
Your lab may do a urinary sediment if there is any abnormality on the dipstick, or may require the physician to ask. The former is wasteful, the latter requires that physicians understand (Am. J. Clin. Path. 137: 486, 2012).
CELLS
Red blood cells
These appear as 7 micron pale discs. Hypertonic urine crenates them, and hypotonic urine makes them swell. Normally there may be 1-2/hpf. If there are 3 or more, work it up. Working up microscopic hematuria: Am. Fam. Phys. 73: 1748, 2006.
In glomerular hematuria only, red cells are likely to show certain dysmorphic features (acanthocytes, blebbed donuts). This is fascinating, but it is of limited clinical usefulness, because (1) you can't appreciate the changes except with a phase-contrast microscope, and (2) it does not yield information that cannot be obtained with a standard history, physical exam, and routine labs (J. Urol. 160: 1492, 1998).
Polymorphonuclear leukocytes
Granular spheres ("glitter cells" -- the Brownian movement makes the granules move around), 12 microns across. Think of infection, of course; there are many other causes though these are less common. In fact, if there are no glitter cells in the urine, there's no urinary tract infection (at least in kids, and physicians can learn to do it at point-of-care: J. Clin. Path. 63: 823, 2010).
Ten or more WBC/mm3 of urine says urinary tract infection, especially when the history and physical exam are right (Med. Clin. N.A. 75: 313, 1991). However, culture is more sensitive and of course more specific.
Renal tubular cells
Cuboidal cells. Think of renal tubular disease (pyelonephritis, ATN).
Lipid-laden cells
Tubular cells plus absorbed lipids (cholesterol esters polarize as Maltese crosses -- triglycerides require fat stain). Think nephrotic syndrome, diabetic nephropathy.
Other cells
Transitional cells (if you are concerned about tumor, send urine for cytology), squamous cells (vaginal), sperms, trichomonads, "miscellaneous" (see Am. J. Clin. Path. 77: 1126, 1984).
Eosinophils are easy to see if you use Wright's stain or Hansel's stain (NEJM 315: 1516, 1986). More than 5% eosinophils suggests allergic acute interstitial nephritis or (nobody knows why) atheroembolization, though if you want to be sure of the diagnosis of this untreatable problem, a renal biopsy is required.
BACTERIA
Yes, you can easily see them. This is probably unfortunate, because of the 1980's fad for trying to eradicate them in the absence of any sign they were doing harm. How the business ended: Am. J. Dis. Child. 146: 343, 1992.
CASTS
The basic material is precipitated protein and matrix secretion (Tamm-Horsfall mucoprotein) from ascending loop of Henle and distal convoluted tubules. Casts are likely to form when there is slow flow of concentrated, acidic urine in the nephron.
All cellular casts undergo degeneration to granular and waxy casts
Hyaline casts: normal finding. Excess number is "cylinduria", no real significance.
* "Hyaline" casts with adherent epithelial cells and/or giant cells are probably composed of myeloma protein.
* A PAS stain may be useful if you suspect a deep fungal infection of the kidney.
WBC casts: acute pyelonephritis (much less often, lupus or other interstitial nephritis)
RBC casts: nephritic syndrome or necrotizing glomerulopathy
Granular casts (coarse or fine): look for some other casts
Epithelial cell casts: think of tubulointerstitial disease. In acute tubular necrosis, the pathologist may be able to show you the typical muddy brown casts.
Fatty casts (i.e., fat within tubular epithelium): think of the nephrotic syndrome -- but the diagnosis should be obvious already
* Blue fluorescent casts are triamterene (Nephron 51: 454, 1989). You are perhaps going to get triamterene nephropathy.
Waxy and broad casts: this is bad renal disease
| CRYSTALS |
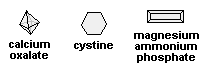 |
We think only calcium oxalate, cystine, and magnesium ammonium phosphate are worth knowing.
Acid urine:
calcium oxalate (octahedra, etc.): finding a few isn't abnormal, or think of vitamin C faddist, ileitis (especially Crohn's), ethylene glycol poisoning, or a spinach gourmet....
cystine (colorless hexagons): cystinuria (THIS one's important to know, because it indicates a treatable disease....)
* uric acid (brick dust, rhomboids, hexagons, squares): normal. If numerous, think of gout or leukemia (but you probably already know the patient was hyperuricemic....)
* leucine (bicycle wheels) and tyrosine (sheaves): severe liver disease (but you knew about that anyway....)
* sulfa drugs: a great variety of beautiful crystals may appear in the urine. Oooh! (The old sulfa preparations precipitated in the tubules and often caused severe damage.)
Alkaline urine:
magnesium ammonium phosphate ("triple phosphate", "struvite"; "coffin lids"): infection with urea splitting bacteria
* ammonium biurate ("thorn apples"): ditto
* calcium phosphate (amorphous dust): no real significance
* Indinavir produces crystals in patients being treated for HIV: Arch. Path. Lab. Med. 124: 246, 2000.
|
|
URINE SCREENING FOR DRUGS OF ABUSE (Mayo Clin. Prod. 83: 66, 2008)
The availability of accurate, reliable drug screens was probably the biggest victory in our "war on drugs". If a test is to have medicolegal consequences (i.e., someone will go back to prison for returning to heroin, some will lose their job for having smoked a joint of marijuana), the screening test (usually an immunoassay) must be confirmed by a test using a different chemical principle (gas chromatography / mass spectroscopy, or maybe high-performance liquid chromatography).
Your hospital will also test for alcohol, benzodiazepines, and antidepressants.
You can do a simple drug-screen in your office on urine. It's worthwhile -- just remember your bond of trust with the patient (i.e., if it pops up positive for cannabis, which stays around for a very long time, there will be a permanent record), and that the popular kit misses hydrocodone, oxycodone, methadone, fentanyl, tramadol, and some others (Am. Fam. Phys. 81: 635, 2010).
* It's a notorious fact that urine positivity for cannabinoids lasts much longer than cocaine, methamphetamine, or heroin -- stoners can stay positive for weeks. For this reason, Friday-night partygoers who may be random-urine-tested on Monday are more likely to use a more dangerous drug than smoke a joint. You'll need to decide whether firing employees who test positive for cannabis is really a wise social policy.
Labs that test for drugs routinely comment if the specimen is not urine (i.e., doesn't contain enough creatinine) or has had chemicals added to give false-negative tests.
* One of your lecturer's best cases was the successful courtesy defense of a truck driver who lost his job and whose insurance benefits were denied "because he was driving under the influence of marijuana." The other side's toxicologist failed to mention that the levels of cannabinoid in his blood were two orders of magnitude below "stoned", and were consistent with having been around another smoker, just as he'd said. Future doctors: Please be honest, and don't withhold key facts in a matter of law just to save money for a company.
MORE THINGS TO DO WITH URINE:
Tests for microbial antigens for rapid diagnosis of infection elsewhere in the body are also coming into use (for example, the screen for legionella is specific but not sensitive). Stay tuned.
TO THINK ABOUT:
1. Why is it often so difficult to obtain a complete 24-hour urine specimen? When do you really need one?
2. Millions of Americans take big doses of vitamin C daily. How does this complicate the chemical urinalysis? Is this important?
3. Why is there no widely-accepted standardized procedure for microscopic urinalysis?
4. Recreational drug users often try to obtain opiates by feigning renal colic. What might an enterprising junkie do to make his or her presentation more convincing? How might the suspicious clinician detect the deception? Why might a malingerer spit in his or her urine specimen?
5. Which of the following are "worthless"? This was a big question in the 1980's, when gouging third-party payers for "routine tests" supported other services that were not fairly reimbursed. Ask your clinical teachers. Ask the third-party payers. Ask a lawyer.
a."Routine urinalysis" on:
b. The "bilirubin" pad on the dipstick
c. The "urobilinogen" pad on the dipstick
d. Urine sediment examination following a normal chemical urinalysis
e. Following up a "trace positive" urine protein with more tests
f. Urine culture in immunocompetent patients in the absence of WBC's
g. Most of what you read about urine crystals
h. Urine porphobilinogen on an improperly collected sample
i. Screening the pediatric population for asymptomatic bacteriuria
j. Dipsticking urines at well-child visits
1. Retract foreskin (if not circumcised).
2. Using one of the towelettes provided, cleanse the urethral opening with a single stroke directed from the ring of the glans toward the tip. Discard towelette.
3. Repeat cleansing procedure using two more towelettes.
4. Void into the toilet and continue to void but interrupt the stream to collect urine into the supplied container.
5. Close the container, complete information on label, and attach it to the specimen container.
1. While seated on the toilet spread the outer folds (labia majora).
2. Using one of the towelettes provided (see step 2 above), wipe the inner side of one inner fold (labium minor) by using a single stroke from front to back; discard towelette.
3. Using a second towelette, repeat step 2 on the opposite side.
4. Using a third towelette, cleanse urethral (urinary) opening with a single front-to-back stroke.
5. Void into the toilet and continue to void, but interrupt stream to collect urine into the supplied container.
6. Close the container, complete information on the label, and attach it to the specimen container.
For proper evaluation of tests on a 24-hour urine sample it is important that a complete and accurate collection be made.
Drink less liquids during the collection period than you usually do, unless instructed otherwise by your physician. Do not drink any alcoholic beverages.
1. Empty your bladder when you get up in the morning and discard this urine.
(______________ A.M., __________________________)
(time)
(date)
2. From then on collect in a clean bottle all urine you pass during the day and night.
3. Make your final collection when you empty your bladder the next morning at the same hour.
(______________ A.M., __________________________)
(time)
(date)
4. Keep the collected urine refrigerated, if possible, and bring it to the office or laboratory as soon as possible after the 24-hour collection is complete.
BIBLIOGRAPHY / FURTHER READING
I urge anyone interested in learning more about urinalysis to consult these standard textbooks.
In my notes, the most helpful current journal references are embedded in the text. Students using these during lecture strongly prefer this. And because the site is constantly being updated, numbered endnotes would be unmanageable. What's available online, and for whom, is always changing. Most public libraries will be happy to help you get an article that you need. Good luck on your own searches, and again, if there is any way in which I can help you, please contact me at scalpel_blade@yahoo.com. No texting or chat messages, please. Ordinary e-mails are welcome. Health and friendship!
| New visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if people like me who call ourselves Christians didn't try to act as good as other good people ." Prayer Request

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |
Teaching Pathology
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |
 |
Click here to
see the author prove you can have fun skydiving without being world-class. Click here to see the author's friend, Dr. Ken Savage, do it right. |
