Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com
No texting or chat messages, please. Ordinary e-mails are welcome.

|

|
 |
 |
 |
 |
|
verify here. |
Cyberfriends: The help you're looking for is probably here.
This website collects no information. If you e-mail me, neither your e-mail address nor any other information will ever be passed on to any third party, unless required by law.
This page was last modified January 1, 2016.
I have no sponsors and do not host paid advertisements. All external links are provided freely to sites that I believe my visitors will find helpful.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected. No texting or chat messages, please. Ordinary e-mails are welcome.
 I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
 If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

|
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource.
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
pathology.org -- my cyberfriends, great for current news and browsing for the general public
EnjoyPath -- a great resource for everyone, from beginning medical students to pathologists with years of experience
Medmark Pathology -- massive listing of pathology sites
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm still handling dozens of requests for information weekly, all as a public service.
Pathology's modern founder, Rudolf Virchow M.D., left a legacy of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of all the make-believe and bunk that interfere with peoples' health, reasonable freedom, and happiness. I talk and write straight, and without apology.
Throughout these notes, I am speaking only for myself, and not for any employer, organization, or associate.
Special thanks to my friend and colleague, Charles Wheeler M.D., pathologist and former Kansas City mayor. Thanks also to the real Patch Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:

My home page
More of my notes
My medical students
Especially if you're looking for information on a disease with a name that you know, here are a couple of great places for you to go right now and use Medline, which will allow you to find every relevant current scientific publication. You owe it to yourself to learn to use this invaluable internet resource. Not only will you find some information immediately, but you'll have references to journal articles that you can obtain by interlibrary loan, plus the names of the world's foremost experts and their institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review. If you are interested in complementary medicine, then I would urge you to visit my new Alternative Medicine page. If you are looking for something on complementary medicine, please go first to the American Association of Naturopathic Physicians. And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I do not accept donations, though I appreciate those who have offered to help.
During the eighteen years my site has been online, it's proved to be one of the most popular of all internet sites for undergraduate physician and allied-health education. It is so well-known that I'm not worried about borrowers. I never refuse requests from colleagues for permission to adapt or duplicate it for their own courses... and many do. So, fellow-teachers, help yourselves. Don't sell it for a profit, don't use it for a bad purpose, and at some time in your course, mention me as author and William Carey as my institution. Drop me a note about your successes. And special thanks to everyone who's helped and encouraged me, and especially the people at William Carey for making it still possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
BIBLIOGRAPHY / FURTHER READING
I urge anyone interested in learning more about neuropathology to consult these standard textbooks.
In my notes, the most helpful current journal references are embedded in the text. Students using these during lecture strongly prefer this. And because the site is constantly being updated, numbered endnotes would be unmanageable. What's available online, and for whom, is always changing. Most public libraries will be happy to help you get an article that you need. Good luck on your own searches, and again, if there is any way in which I can help you, please contact me at scalpel_blade@yahoo.com. No texting or chat messages, please. Ordinary e-mails are welcome. Health and friendship!
|
|
Niels Bohr
|
|
Stroke and Hemorrhage: 2-19, 22-27, 69-85, 162-230, 311-312 CNS Infections: 85-161, 289 Neurodegenerative disease: 232, 234-242, 244-248, 250-254, 256, 258, 262-266, 273, 276-282, 284-286, 291-294, 297-300, 302-304 Demyelinating Disease, Poisons: 231, 233, 243, 249, 255, 257, 259-261, 267-272, 274-275, 283, 287, 290, 295-296, 301, 305-310, 313-333, 387 Tumors: 334-384 |
No one is born wise.
-- Ptahhotpe, c. 2350 B.C.
I do not understand my own behavior.
-- Paul of Tarsus, Romans 7
Be not angry that you cannot make others as you wish them to be, since you cannot make yourself as you wish to be.
-- Thomas of Kempis
"It must be inconvenient to be made of flesh," said the Scarecrow, thoughtfully, "for you must sleep, and eat and drink. However, you have brains, and it is worth a lot of bother to be able to think properly."
-- Scarecrow, The Wizard of Oz
How many psychiatrists does it take to change a light bulb?
Only one, but it takes a long time, and the light bulb has to WANT to change.
-- Anonymous
A good person can be stupid and still be good. But a bad person must have brains.
-- Maxim Gorky
Ah, it is the fault of our science that it wants to explain all, and if it explain not, then it says there is nothing to explain.
-- Dr. Abraham Van Helsing (pathologist), Dracula (Bram Stoker)
I'd rather have a free bottle in front of me than a prefrontal lobotomy.
-- Anonymous
Volumes are now written and spoken upon the effect of the mind upon the body. Much of it is true. But I wish a little more was thought of the effect of the body on the mind.
-- Florence Nightingale
For botulism![]() ,
click here.
,
click here.
For tetanus![]() , click here.
, click here.
* Autopsy on brain and muscle: Arch. Path. Lab. Med. 119: 777, 1995.
* Jung accused Freud of "regarding the brain an appendage of the sexual organs." Be this as it may, our brains are what tells us "happy" or "not happy". Some people report themselves to be happier than others, and this tends to stay constant over time. Contrary to what you've been told (by "liberals" or "conservatives"), there's little-or-no correlation with age, race, economic class, or educational level. There's a strong correlation between being happy and (1) being basically in control of your own destiny; (2) being physically healthy; (3) being happily married; (4) living in a country where there's opportunity. See Sci. Am. 274(5): 79, May 1996.
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
NEUROPATHOLOGY UNIT: LEARNING OBJECTIVES
Explain briefly what makes neuropathology more difficult than the pathology of other organ systems.
Describe the prevalence of CNS disease, and its impact.
Describe the behavioral correlates of "minimal brain damage", where there may be no demonstrable anatomic pathology.
Describe how brain lesions cause death, and what brain lesions will not in and of themselves cause death.
Describe the concept of selective vulnerability of neurons, giving examples.
Describe the common birth defects involving the brain, giving risk factors and clinical correlates insofar as they are known.
Give a full account of the etiology, anatomic pathology (brain and elsewhere), and clinical correlates of tuberous sclerosis.
Give the anatomic correlates of cerebral palsy, and what we know and don't know about its etiology.
Tell what leukodystrophies are, and what "sclerosis" means in the brain.
Describe how brain cells are injured and killed. Give a short account of excitotoxicity.
Recognize these developmental brain lesions:
Recognize these histopathologic features of brain cells:
Explain how cerebral edema occurs, and distinguish interstitial, intercellular and intracellular edema in terms of etiology and morphology.
Explain the causes of mass shifts in the brain, and the consequences of herniation.
Distinguish communicating and noncommunicating hydrocephalus, and hydrocephalus ex vacuo.
Tell about situation in which the brain is damaged from lack of oxygen, glucose, or blood flow. Describe factors determining the severity of the outcome. Give an account of the consequences of profound ischemia / hypoxia on the brain, and of hypoglycemia. Tell when damaged brain will liquefy, and when it will remain solid.
Describe the causes of cerebral infarction, and recognize them anatomically as applicable. Give a full account of the varying anatomic pathology of cerebral infarcts.
Describe the effect of blood in the ventricular system. Describe the causes, usual locations, and consequences of intracerebral hemorrhage.
Describe the causes and consequences of subarachnoid hemorrhage. Give a full account of berry aneurysms, including locations, histopathology, and known risk factors.
Explain the causes and consequences of germinal plate bleeds in babies. Describe the common neuropathology lesions in the premature nursery.
Describe the anatomic pathology and effects of hypertension on the brain.
Describe the impact of trauma directly on the brain. Distinguish concussion, contusion, and laceration. Give a full account of coup and contrecoup injuries, and of traumatic axonal injury. Describe the neuropathology of boxers.
Describe epidural and subdural hematomas, making sure to distinguish how they occur and how they impact on the patient.
Describe how the spinal cord is usually injured, and the anatomic pathology of acute and old spinal cord trauma.
Recognize these cerebrovascular problems grossly and/or microscopically as appropriate
Distinguish encephalitis, meningitis, and cerebritis.
Give a full account of common bacterial meningitis. Mention the most common bacteria producing meningitis in patients in various ages and situations. Describe the serious complications and how they occur.
Give the anatomic pathology, common agents, and clinical picture in viral meningitis. Mention non-infectious causes of meningeal inflammation.
Give full accounts of tuberculous![]() and
cryptococcal
and
cryptococcal![]() meningitis.
meningitis.
Describe the four different lesions of neurosyphilis![]() . Briefly discuss the neuropathology
of Lyme disease
. Briefly discuss the neuropathology
of Lyme disease![]() .
.
Describe how brain abscesses occur, why they are so treacherous, and what they do.
Describe the anatomic pathology and clinical correlates of viral encephalitis
caused respectively by arbovirus, childhood exanthems, von Economo's,
herpes simplex I![]() ,
herpes simplex II
,
herpes simplex II![]() ,
CMV
,
CMV![]() ,
rabies
,
rabies![]() ,
and HIV. Name the virus that causes tropical spastic paresis.
Give a pathology account of
poliomyelitis
,
and HIV. Name the virus that causes tropical spastic paresis.
Give a pathology account of
poliomyelitis![]() .
.
Describe the agents, pathology and clinical correlates of the slow virus infections (subacute sclerosing panencephalitis, progressive multifocal leukoencephalopathy).
Give a full account of prion disease.
Briefly describe the effects on the nervous system of
Rocky Mountain spotted fever![]() ,
amoebas, toxoplasmosis
,
amoebas, toxoplasmosis![]() ,
cysticercosis, and trypanosomiasis.
,
cysticercosis, and trypanosomiasis.
Tell the common causes of headache, and the causes to rule out in the emergency room!
Recognize these CNS infections grossly and/or microscopically as appropriate:
Tell generally what we know about the neurodegenerative diseases, and why we are coming to refer to them today as the "proteinopathies".
Distinguish delirium, dementia, and mental retardation. Tell how patients with dementia may present. Give a full "differential diagnosis" for dementia in older people. Give the lab workup that screen for the common treatable causes.
Give a full account of what we know about the causes and the pathology of Alzheimer's disease. Describe likely future preventions and therapies for Alzheimer's. Describe Pick's disease and its relatives (the frontotemporal dementias).
Recognize Huntington's disease, and explain how the genetic lesions, with trinucleotide repeats, causes the cell injury and the genetic anticipation.
Tell what we know and don't know about the causes of Parkinsonism. Recognize depigmentation of the substantia nigra, and recognize idiopathic and postencephalitic Parkinsonism microscopically. Distinguish Parkinsonism from essential (benign familial) tremor.
Briefly describe the multiple systems atrophy diseases, including Shy-Drager. Give an account of progressive supranuclear palsy, Lewy body dementia, and the spinocerebellar ataxias.
Describe what we know about the causes of the motor neuron disease complex.
Describe what we know about the causes and anatomic pathology of schizophrenia. Give a short account of how society has made decisions about how to care for mentally-ill people.
Review the cellular lesions that are seen in the dementias. Recognize these neurodegenerative diseases grossly and/or microscopically as appropriate:
Give a full account of the anatomic pathology of multiple sclerosis, what we know of the etiology, and how these relate to the clinical progression. Briefly describe some other autoimmune demyelinating diseases.
Tell what we know about central pontine myelinolysis.
Describe the common leukodystrophies.
Describe the effects of alcoholism, carbon monoxide, Reye's, methanol, arsenic, manganese, Wilson's, the common storage diseases, and radiation.
Give accounts of Guillain-Barré, and of the common peripheral neuropathies.
Recognize these demyelinating, toxic, and peripheral nerve diseases grossly and/or microscopically as appropriate
Mention the common paraneoplastic CNS syndromes.
Recognize these tumors grossly and microscopically:
HOW IS NEUROPATHOLOGY DIFFERENT?
Facts about the brain:
The brain contains around 100 billion neurons. Even the best neuropathologist cannot appreciate loss of fewer than 30% of neurons on an H&E section.
We have all our neurons when we are babies, but they aren't yet connected as in an adult. Further, the brain is not fully myelinated until age 10-12 years. This probably explains most developmental milestones, including those of Piaget.
The brain has a great deal to do with our learning, thinking, mood, speech and behavior.
* About half the human genome is supposed to be brain proteins. This leaves a lot of room for unrecognized syndromes and explanations for personality and interest variables.
Brain disease is common.
"Stroke" (i.e., cerebrovascular disease) is "the third leading cause of death" in the developed world, and an extremely important cause of disability.
Alzheimer's disease, once considered either "rare" or "a normal part of growing old" and therefore ignored, is finally being recognized as a major public health problem.
There are about 17,000 cases of primary malignant brain tumors in the US yearly; the majority prove fatal.
| There are about 500,000 people in the U.S. with severe sequelae of head injury. |  Memento |
In 1990, there were around 10,000 people in the U.S. in irreversible coma, at a cost of $130,000 per patient per year (Br. Med. J. 30: 1094, 1990). I have been unable to find more recent figures.
In prolonged coma, recovery with a return to a decent quality of life sometimes (though rarely) occurs if the coma is due to trauma, i.e., snapped fibers can grow back; NEJM 334: 24, 1996. It won't happen if the coma is due to ischemia / hypoxia, i.e., dead cells can't grow back; Acta Neurol. Belg. 97: 214, 1997. Obviously, in diabetic and renal coma and in poisoning, treating the underlying disease/poisoning is effective. But the very bad outlook of other non-traumatic coma lasting over three days is documented in Crit. Care Med. 30: 1382, 2002; the authors suggests Day 4 as the time to decide not to continue aggressive care. (* Make it Day 1 for me. -- ERF.)
Many more are LOCKED IN ("Monte Cristo syndrome", "The Diving Bell and the Butterfly", only able to move their eyes; ethicists see Am. Acad. Neuro. statement Lancet 342: 130, 1993) or otherwise profoundly damaged so as to be completely unable to care for themselves. Different people will come to different conclusions about what this means.
Since 2002, we have distinguished:
PET scans reportedly distinguish these, and newer techniques seem to as well (Brain 135: 1308, 2012; J. Trauma 72: 1024, 2012). In the MINIMALLY CONSCIOUS STATE, connections between the cortical association areas and the primary cortical areas preserved and recovery is sometimes possible (though the patients may have some ability to communicate and appear unhappy). In the PERSISTENT VEGETATIVE STATE, they are disconnected and recovery (especially after a year) isn't going to happen (Arch. Phys. Med. Rehab. 87(12 S 2): S-67, 2006; Mayo Clin. Proc. 80: 1037, 2005.)
In the persistent vegetative state, neuropathology is always widespread. It may be either laminar necrosis of the cortex after cardiac arrest (Terry Schiavo) or diffuse axonal injury (following trauma).
* The Rom Houben fiasco resulted from the use of the long-discredited technique of facilitated communication; simple scientific tests showed the "communications" from this man, in persistent vegetative state for 23 years, were fake (Lancet 375: 1337, 2010).
In the minimally-conscious state and other cases of severe disability, there may be a single focal lesion (Neurology 56: 486, 2001).
Don't confuse either with AKINETIC MUTISM, a poorly-named syndrome in which the patient lies inert, follows with the eyes, says nothing or a single word, and seems emotionless. When you see this, think of damage to both cingulate gyri or both paramedian portions of the thalamus (J. Neuropsych. Clin. Neuro. 21: 351, 2009).
You'll need to decide for yourself what all this means. The law is in a state of change.
* A lot of changes took place in the late 1990's, as managed care hit hard. In Canada, where the public pays for health care directly, they've been talking about ignoring families' wishes to do CPR on these patients (CMAJ 159: 18, 1998); not so long before, this would have been unthinkable.
* "Pathology informs bioethics." For the facts on the Terri Schiavo case, see NEJM * For the not-really-happy story of minimally-conscious Don Herbert, fireman hero
who came out of minimally-conscious state after ten years, see JAMA 299:
959, 2008. If we are keeping minimally-conscious people alive in the slight hope
that they can have the kind of experience that Don Herbert had, then please don't do it to me.
Thanks.
"Pathology informs bioethics." Of course, it is still very difficult to determine whether someone who cannot
communicate is conscious (i.e., it is not always possible
to tell persistent vegetative state from totally-unable-to-move
locked-in syndrome). The most recent work (NEJM 362: 575, 2010) used MRI's,
which can distinguish whether a person is (1) thinking about standing still lobbing tennis
balls; (2) thinking about navigating an automobile, or (3) doing neither.
Five of 54 people who seemed unable to communicate proved able to
answer "Yes" or "No" ("Do you
have any brothers?")
questions accurately by concentrating on "tennnis" for "Yes" or "driving" for "No".
After reading the article, I was left asking, "Did anyone ask these people if they wanted to
be forced to remain alive?" Another study with similar findings suggesting
a very few of these people can at least follow mental commands: Lancet 378:
2088, 2011. More people are doing work like this: Neurology 78:
816, 2012 ("Imagine moving the toes on your right foot.")
Follow this closely -- this is tomorrow's headlines.
The worst is not so long as we can say, "This is the worst."
-- Shakespeare, "King Lear"
Pretty much anything bad that happens to the brain can leave the person with minimal brain damage. Distinctive features are (1) poor judgement; (2) irritability; (3) poor impulse control; (4) lack of insight; (5) hyper- or hypo-sexuality; (6) inability to learn from experience.
As you might expect, we are coming to recognize the importance of past head injury in criminal misbehavior (for example, Am. J. Psychotherapy 44: 26, 1990, from Hopkins, past due; also J. Trauma 41: 972, 1996, army discharge followups). A kid hospitalized overnight after head injury is much more likely, years later, to have learning and/or behavioral problems (Pediatrics 94: 425, 1994) -- before you conclude that head injury causes behavioral problems, though, note that teenaged males in reform school who have head injuries (often with epilepsy / abnormal EEG's) are also much more likely to come from drug-infested homes and hence have been struck on the heads (Psych. Clin. Neuro. 59: 661, 2005).
Neurologic disease is seldom curable. Even more than other branches of medicine, neurology requires a special kind of physician. The focus is on rehabilitating, educating, finding resources, and helping people manage in spite of disabilities.
Neuropathology presents special difficulties for students at any level. "Big Robbins" lists several of the reasons. Brain disease is unlike disease in other organs because:
FUNCTION IS LOCALIZED in the brain, far more than in any other organ. Because of this, the site, rather than the nature of the pathologic process, typically determines symptoms.
A tiny lesion in an "eloquent" area may present striking clinical problems; a large infarct in a "silent" area is missed. Diverse lesions (infarcts, abscesses, tumors) in one site may produce similar problems, while similar pathologic processes at different sites will present different pictures.
A neuropathologist must be a good neuroanatomist, and it is essential to describe the location ("distribution") accurately in making clinico-pathologic correlations.
He or she will also describe diffuse processes (ischemic injury after shock, storage diseases), focal lesions (infarcts, abscesses, and tumors) and systematized lesions (i.e., Huntington's chorea, Parkinsonism, many others).
| * By convention, a coronal section of brain will be displayed as if you are looking at the head from the back, and a horizontal section as if you are looking at the head from above. |
 |
Remember:
CELLS OF NERVOUS TISSUE ARE SELECTIVELY VULNERABLE to various diseases.
For example, Alzheimer's disease hits the hippocampus and cholinergic nucleus
of Maynert harder than the rest of the brain. Mercury
selectively damages the cerebellar granular neurons, methanol poisons the retina
and putamen, and
poliomyelitis![]() destroys only the anterior horn cells.
destroys only the anterior horn cells.
Even short ischemia, severe hypoxia, or severe hypoglycemia will damage Sommer's sector (CA1) of the hippocampus (and other areas of the cortex), the Purkinje cells of the cerebellum, and the basal ganglia.
THE BRAIN CANNOT EXPAND without becoming deformed, because the skull is solid. (It has to be, or brain injuries would be much more common.)
THE INTERSTITIAL SPACE WITHIN THE BRAIN IS QUITE SMALL (gray matter 200 angstroms, white matter 800 angstroms).
THE SPINAL FLUID PRESENTS UNIQUE PROBLEMS (high pressure hydrocephalus, dissemination of infections and cancer cells.)
THE BLOOD-BRAIN BARRIER (when intact) alters brain tissue reactivity.
It is demonstrated by injecting the dye trypan blue (which is bound to albumin). It also explains why the lipid in the brain is not yellow (the yellow tryptophan metabolites do not cross the brain).
THE BRAIN HAS NO LYMPHATICS, making edema much more of a problem when it happens. (The absence of lymphatics does help prevent dissemination of infection to the brain.)
NEURONS HAVE LIMITED ABILITY TO HEAL / REGENERATE. This is probably a good thing, since regenerating neurons might lay down bogus memories (witness the adrenal medulla transplant patients, wait for the human stem cell experiments); it also prevents mature neurons (but not neuroblasts) from giving rise to tumors.
BRAIN LESIONS TOO SUBTLE TO SEE HISTOLOGICALLY OR ULTRASTRUCTURALLY CAN PRODUCE PROFOUND EFFECTS ON BEHAVIOR. (Many obviously organic brain diseases -- dyslexia, schizophrenia, attention-deficit disorder, genuine manic-depression, idiopathic epilepsy, and so forth -- still are pathologically ill-defined.) This contrasts with all other organs of the body, in which considerable deviation from normal structure may be consistent with good health.
Certain nervous system disease processes (i.e., gliosis, demyelination, neuronal degeneration, the many curious inclusions) are NOT FAMILIAR FROM GENERAL PATHOLOGY.
What makes all this even more difficult for beginners are the facts that...
* Future pathologists: The brain is fragile and decomposes rapidly
after death. Some hard-core pathologists deep-freeze the heads of
decomposed bodies and dissect them in sub-zero temperatures, just to
be able to see the anatomy.
* Tutorial on reading brain biopsies: Arch. Path. Lab. Med. 130:
1602 & 1639, 2006.
* One of the nut movements of the 1990's was
self-trepanation, i.e., drilling a hole in your own skull to
enable the brain to pulsate as it supposedly does before the sutures
are closed, enabling one to learn with a child's speed.
A few folks are stupid enough to try it.
This was presented on "ER" 11/12/98.

BRAIN DEVELOPMENT AND ITS PROBLEMS
Different patterns of malformation correlate with mishaps (known or unknown) at different times.
Known causes include maternal alcoholism, mercury poisoning, lead poisoning, radiation, and exposure to vincristine. Of course the links to folic acid deficiency, valproic acid treatment, and hypervitaminosis A / acne remedies in the case of neural tube defects are famous. But in the vast majority of cases, the etiology is never found.
Since the completion of the human genome project, dozens of genetic diseases have been found that cause malformations of the brain. Review: Neurology 65: 1873, 2005.
Week 3-4: The neural tube forms and fuses
DYSRAPHISM: failure of the neural tube to close properly. A generic term for all the following.
Folic acid deficiency is now very well-known as a cause, and has resulted in the fortifying of foods in the US; incidence dropped by about a third (Teratology 66: 33, 2002; from the CDC). Parts of Canada had a 78% reduction: Br. Med. J. 324: 760, 2004; as you'd expect, it is greatest where the rate was highest (NEJM 357: 135, 2007).
Vitamin A (retinoids, but not carotenoids) toxicity also seems to be a cause, with an effect appearing above 10,000 U/day (NEJM 333: 1369, 1995).
* The VANGL1 locus has alleles that greatly increase risk: NEJM 356: 1432, 2007.
ANENCEPHALY:
The most common congenital brain malformation (and among the most severe; * the ultimate is "anencephalus craniorachischisis", with the back of the vertebral column also fully open).
In anencephaly, there is little or no forebrain, merely nubbins of abnormal nervous tissue (* area cerebrovasculosa). There is no top to the skull or orbits, and the eyes protrude. There is generally a scrambled brainstem. Of course, the pituitary and adrenals won't develop right, either.
{10331} anencephalic
{39138} anencephalic
{39140} omphalocele; child also had anencephaly
* Anencephaly is very common in Ireland and Wales (maybe 1 child in a few hundred, compared with maybe 1 in several thousand in the U.S. before folic acid fortification); there is a modest female preponderance.
This works even when you control for the fact that abortion of
an anencephalic fetus is illegal in Ireland. The anencephaly rates also dropped in Ireland
during the late 20th century, probably due to
better diet (J. Epidem. Comm. Health 53: 782, 1999).
Currently, we screen for these problems by checking maternal serum for elevated alpha-fetoprotein, which oozes out of the defect in the fetus.
The most important known risk factor is lack of folic acid. The junk food diet is part of the problem, and some unborn children need much more folic acid than others do because of a mutant folic acid processing gene (Lancet 246: 1070, 1995). Mandatory fortification of cereal grains with folic acid went into effect in the US in 1998; this resulted in about a 25% drop in anencephalic births (MMWR 53: 362, 2004; I was hoping for a larger drop.)
Amniotic band syndrome can also cause anencephaly.
* "Pathology informs bioethics." It is now possible, once again, to bring these children to term as planned organ donors, although the child must still die of "natural causes" (i.e., get septic, which takes a few days) making some of the organs unusable. For an amazing and wonderful account, see Journal of Christian Nursing 25: 97, 2008.
ENCEPHALOCELE:
Deformed brain herniates out through a defect in the skull at birth, and bulges underneath the skin. This may be under the scalp, or in the neck; the latter may be a surprising cause of airway obstruction (J. Laryn. Ot. 113: 369, 1999).
{53752} encephalocele
{15843} encephalocele in amniotic band syndrome
{13397} encephalocele
Some of these children can survive and even lead useful lives.
Contrast "meningocele", in which only meninges (dura, arachnoid) herniate through skull or vertebral column.
RACHISCHISIS ("the worst kind of spinal bifida"): Complete failure of dorsal closure of the spinal canal. The spinal cord lies at the bottom of a furrow, covered only by a thin membrane.
CRANIOSCHISIS: Skull defect analogous to rachischisis.
CRANIUM BIFIDUM: Split skull with encephalocele. (* There are genetic syndromes.)
MYELOCELE ("meningomyelocele"; "bad spina bifida")
The spinal cord ("myelo-") herniates through a defect in the dorsal aspect of the vertebral column (much less often, the anterior aspect, for example, orbital and nasopharyngeal meningoceles).
Most are lumbar or sacral; in the cervical or thoracic areas, meningocele (i.e., the meninges herniate, but the cord does not) are more common.
With mandatory folic acid fortification, the "spina bifida" rates also dropped about 25% in the US (MMWR 51: 9, 2002).
{05224} myelocele
{12424} myelocele
{13396} myelocele
{13398} myelocele
Complications include distal weakness, incontinence, and meningitis.
Perhaps 80% have associated hydrocephalus.
The first children euthanized under the 2005 Netherlands "Groningen Protocol" wer all children with open neural tube defects. Parents from other nations are now taking these children to the Netherlands for this purpose.
SPINA BIFIDA OCCULTA: A radiographic defect in a vertebral body, perhaps as trivial as lack of a spinous process. These are quite common and a non-problem unless there is an associated CNS defect. (Unanswered question: If "the cause of spina bifida is failure of closure of the neural tube", why does the "mild version" involve only the bone?)
Weeks 5-6: The rostral CNS cleaves into two hemispheres
HOLOPROSENCEPHALY ("prosencephaly"; "holotelencephaly"; J. Clin. Invest. 119: 1403, 2009): Failure of the the hemispheres to separate fully; the most severe form being a single telencephalic hemisphere.
We now know that around 1 child in 250 is conceived with holoprosencephaly or one of its minor variants; most of these miscarry, only 1 in 16,000 live births is affected, and a huge number of genes are known to be involved, as are maternal drug and alcohol use (J. Clin. Inv. 119: 1403, 2009).
{10333} holoprosencephaly
{10336} holoprosencephaly
{25614} cyclops
![]() Holoprosencephaly
Holoprosencephaly
WebPath Photo
In the less-severe cases, there is likely to be absence of much of the limbic system ("arhinencephaly-plus"), and these brains are generally small.
The worst cases are CYCLOPS babies ("cyclopia"), with a single eye below the snout ("proboscis").
Cyclops or no, many of these kids have trisomy 13-15, and most will have some facial deformity (especially cleft palates/lips).
Weeks 6-14: Neurons migrate to their proper positions
AGYRIA (lissencephaly / "smooth brain"): No gyri.
* Lis1, the gene for the common hereditary form cloned: Nature 364: 17, 1993. Seven loci and a variety of phenotypes are now known (Neurology 72: 410, 2009).
PACHYGYRIA (formerly "macrogyria"): A few big, abnormal gyri. Now in the "lissencephaly" category. Several distinctive genes of the kinesin family are often identified here NEJM 371: 733, 2014.
POLYMICROGYRIA: Too many gyri, each too small, with shallow sulci.
* Thanatophoric dwarves tend to have large, polymicrogyric temporal lobes. You may see polymicrogyria in trisomy 18.
* Some people who have polymicrogyria only around the sylvian fissure have absent or poor language abilities without other obvious problems: Neurology 59: 245, 2002.
* Usually this is sporadic; a curious familial form resulted from mosaicism Neurology 76: 988, 2011.
NOTE: In all three of the above conditions, the involved cortex will typically have only four layers, if any layering is recognizable.
{32949} polymicrogyria, gross
{00141} polymicrogyria, gross
{01246} polymicrogyria, patient (severe disability)
AGENESIS OF THE CORPUS CALLOSUM:
Mild clinical syndrome, and in its partial variants quite common (maybe 1 person in 1000).
* Many of these patients supposedly have alexithymia (odd "Mr. Spock from Vulcan" affect, no fantasy life, inability to answer "How do you feel?")
* Look for a lipoma, ependymal cyst, or meningioma here. In "consanguinous families", it's very common and though no loci have been found yet, various subtypes have been identified (Neurology 76: 373, 2011). Have a radiologist show you the "bat wing" sign. There is now a detailed classification scheme: Neurology 56: 220, 2001. It gets discovered on prenatal ultrasound these days; there's a much-increased risk for mental retardation yet most of the kids are fine (Am. J. Ob. Gyn. 206: 337, 2012).
ARHINENCEPHALY: As above -- no olfactory nerves or bulbs. Often this is the only problem, and patients simply observe they cannot smell anything "except ammonia" (which is an irritant.) Sometimes there are other malformations as well, and this is now a continuum with the holoprosencephaly group.
* Pontocerebellar hypoplasia is a group of thankfully-rare illnesess with striking hypoplasia of the basis pontis and cerebellum. Patients are severely disabled. For some reason, the genes involved in tRNA-splicing are involved Neurology 75: 1459, 2010.
ECTOPIAS and HETEROPLASIAS: Neuron clumps in the white matter, where they don't belong. Nobody knows why most of these happen.
CORTICAL DYSPLASIA (Arch. Neuro. 69: 257, 2012) is a mysterious, local failure of migration; often with balloon cells (see below -- perhaps they cause the seizures). In the era of high-resolution imaging, we are recognizing this more and more as the cause of hard-to-manage seizures in children, and it is often removed.
Weeks 15-16: The brain is further modelled
PORENCEPHALY: "A hole in the brain". "Defective closure of the telencephalon" and/or ischemic injury, with destruction of nearby brain. There are cysts lined with ependyma, communicating with the subarachnoid space.
{32139} porencephaly
SCHIZENCEPHALY: A deep fissure in the brain, with a floor of brain substance.
ENCEPHALOCLASTIC PORENCEPHALY: The fissure is so deep that it reaches the ventricle.
{32943} encephaloclastic porencephaly
Most porencephaly cases are idiopathic. Known causes include TORCH and infarcts (Arch. Dis. Child. 78: F121, 1998).
* Your lecturer has long taught that many "idiopathic" cases are caused by trauma, i.e., somebody kicked or beat the pregnant woman in the abdomen. The shape is exactly what you'd expect. And the classic neuropathology literature describes this as being more common in children born out of wedlock and in the underclass. The defense in the Amy Grossberg ("prom mom" -- baby in the dumpster) was that the child had porencephaly and was therefore born dead. Your lecturer talked about this on the Johnny Cochrane show -- and brought up for the first time the likelihood that this was the result of inflicted trauma. She pleaded and the case is over. One known example of a blow to the unborn child causing porencephaly: Dev. Med. & Child Neuro 43: 52, 2001. Another J.A.Optom. 68: 519, 1997.
After six months: The brain is already formed and the gyri are largely modelled, but it can still be damaged (typically by ischemia, viruses, or some serious metabolic process).
HYDRANENCEPHALY: Replacement of the cerebral hemispheres by large cysts made of leptomeninges and glia. There is no ependyma.
This results from ischemia / hypoxia or infection (i.e., TORCH). It may be diffuse or localized.
{10339} hydranencephaly (this happens to have been a case of
toxoplasmosis![]() )
)
{53696} hydranencephaly patient
ULEGYRIA: An old term for loss of neurons in the depths of the sulci, and sparing of the apices of the gyri.
Like hydranencephaly, it may be diffuse or localized. You can also see
ulegyria anytime
after localized cerebral ischemia insufficient to produce generalized
liquefaction![]() .
.
* GRANULAR ATROPHY: Probably ischemic; a mild form of ulegyria.
* ÉTAT MARBRÉ ("status marmoratus"): "Marbling" of the corpus striatum from ischemic damage to the basal ganglia around the time of birth, especially if there is also severe jaundice (i.e., kernicterus). Myelin grows irregularly on these masses of gray matter, giving a marbled look. This is a hallmark lesion in children who have cerebral palsy despite being born at term (J. Clin. Neuro. 20: 940, 2005).
PERIVENTRICULAR LEUKOMALACIA: Loss of oligodendroglia around the ventricles, usually with some dystrophic calcification.
The deep white matter is relatively poorly vascularized in preemies, and perhaps this is the baby counterpart to "watershed infarcts" in the adult.
Mature newborns are more likely to get more damage to the cortex and deep nuclei -- it's a continuum. Whether the periventricular leukomalacia that affects a great many of the preemies who go on to have cerebral palsy, and the sort with which a term child may be occasionally born (which also produces cerebral palsy) are even the same entity is up for debate (Neurology 74: 1386, 2010).
Tough to place:
ARNOLD-CHIARI: Small posterior fossa with...
(1) Elongated cerebellar tonsils that hang through the foramen magnum;
(2) A Z-shaped kink in the CNS at the cervical-medullary junction;
(3) A large foramen magnum and a small, shallow posterior fossa.
(4) A "beak-shaped" tectum (the quadrigeminal plate becomes a single pyramid, perhas due to pressure from the tentorium)
Arnold-Chiari patients often also have hydrocephalus with thickened, adherent leptomeninges, a small cerebellum, and a lumber meningomyelocele. There are often other defects, especially aqueductal stenosis, syringomyelia and * polymicrogyria.
* The dreaded sudden-death from apnea (typically during sleep) may apparently be prevented by decompressive surgery on the skull base and C1 (J. Neurosurg. 112: 800, 2010).
{32996} Arnold-Chiari (there is also pus in the ventricles)
{17683} Arnold-Chiari, long cerebellar tonsils
There are a few syndromes with Arnold-Chiari, but usually it "just happens".
* Future neuro-pathologists: Arnold-Chiari is "Chiari malformation, type II". (Chiari I is long-tonsils-only.)
CEREBELLAR HYPOPLASIA may be seen in Down's or Arnold Chiari, or by itself.
DANDY-WALKER: Large posterior fossa. No cerebellar vermis. Instead, the fourth ventricle is much dilated, and the roof (if any) bulges out.
{05236} Dandy Walker, no roof on vermis
{15466} Dandy Walker, no roof
{16600} Dandy Walker
{39058} Dandy Walker, thin roof
There is generally hydrocephalus, and often a variety of associated malformations.
Physical diagnosticians: A tip-off is prominent occiput.
CRANIOSYNOSTOSIS: Premature closure of one or more of the cranial sutures. A common defect of unknown etiology (1 newborn in 2100). Sometimes it's part of a syndrome; other times it "just happens". Today's surgery usually gets good results, and if the children are of normal intelligence there's usually no behavioral or emotional problems (Plast. Recon. Surg. 124: 2054, 2009).
AMYELIA: At least a portion of the spinal cord is missing ("segmental spinal dysgenesis"; Ped. Neurosurg. 38: 102, 2003).
DIASTEMATOMYELIA: Double spinal cord, at least part of the way.
MICROCEPHALY: Well-formed, but under 900 gm.
MEGALENCEPHALY: Well-formed, but too big (>1800 gm). * Causes include tuberous sclerosis (often), neurofibromatosis (sometimes), Canavan's, cerebral lipidoses, and Alexander's leukodystrophy as causes.
TUBEROUS SCLEROSIS (* "hereditary multisystem hamartosis", * "Bourneville's disease", * "epiloia")
An autosomal dominant syndrome with extremely variable expressivity. Identical twins are often highly discordant for severity (Neurology 62: 795, 2004).
* The genes are TSC1 (chromosome 9, hamartin) and TSC2 (chromosome 16, tuberin); partners in a molecular sequence. Review Neurology 53: 1384, 1999. There are some modifying genes too. Of course, the tubers result from "second hits". Update Neurology 74: 1716, 2010.
Portions of the cortex lack the usual stratification of neurons into layers, and these feel hard and are white, hence the "tubers" (potatoes). There are likely to be various odd hamartomas ("tubers"), calcifications, and tumors in the brain and elsewhere.
Everybody knows of the "candle gutterings", giant-cell astrocyte proliferations on the inner walls of the ventricles in tuberous sclerosis.
This is a very important cause of epilepsy and mental retardation. Look for adenoma sebaceum (fibrous nodules on the muzzle area of the face) and "ash-leaf" spots (areas of hypo-pigmentation on the skin, with the long axes parallel to the dermatomes; these are common in normals too).
{27928} tuberous sclerosis, face; adenoma sebaceum
{27948} tuberous sclerosis, brain; note the white tubers
{01828} tuberous sclerosis, brain; the tubers appear as whiter areas of cortex
{01830} tuberous sclerosis, brain
SYRINGOMYELIA / SYRINGOBULBIA: Probably acquired later in life, but discussed here.
There is a tubular cavity in the center of the cord (generally cervical) and/or brainstem (bad), with surrounding gliosis and no ependyma. There is loss of pain and temperature (since the crossing spinothalamic tract is damaged) over the corresponding levels. Eventually, other sensory and motor pathways may be damaged.
{09022} syringomyelia; myelin stain; the tracts have been damaged by the syrinx above and below
Most often these conditions are idiopathic (and attributed to some mechanical problem involving heartbeat); known causes include old trauma (ask a traffic-accident lawyer), cord tumors and (most commonly) Arnold-Chiari.
* "Hydromyelia" is dilatation of the central canal, i.e., there is an ependymal lining.
NEUROEPITHELIAL CYSTS probably arise from faulty migration during embryogenesis. They gradually grow, and become symptomatic in adult life.
The best-known are the "colloid cysts" that occlude the foramen of Munro, often causing headache only when the head remains in a particular position.
{15678} colloid cyst, foramen of Munro
Most ARACHNOID CYSTS probably arise either from birth defects or trauma. They lie within the arachnoid and may be surrounded by a thin collagenous wall. Look very hard at MRI scans, and you'll find them in a few percent of normal people. They may be large and/or grow over time and require surgical removal.
{01251} arachnoid cyst
{01252} arachnoid cyst
{01253} arachnoid cyst
BRAIN DAMAGE FROM MATERNAL DRUG USE: The latest studies show less gray matter most especially if Mom has used cocaine. The harm from tobacco smoking seems real, and to as lesser extent alcohol. The Harvard authors weren't able to demonstrate an effect from marijuana (Pediatrics 121: 741, 2008).
CEREBRAL PALSY: a lay person's umbrella term for a nonprogressive brain defect present at (or presenting shortly after) birth, with motor and often cognitive problems.
Around 100,000 kids in the U.S. have at least some degree of cerebral palsy. In around 0.2% of kids, the problem is at least moderately severe. One quarter of kids diagnosed with cerebral palsy cannot walk; one third are mentally retarded; one third are epileptic. Some kids outgrow the motor problem.
Lay wisdom is that "cerebral palsy is the obstetrician's fault, the baby did not get enough oxygen to the brain." (Ask a lawyer; this is probably true only of a minority of cases; the advances in obstetrical and neonatal care in the last few decades have had no measurable impact on the rate of cerebral palsy.) What we DO know is that about 40% of cerebral palsy cases come from among the 1.5% of babies born weighing less than 1500 gm (NEJM 358: 1700, 2008). Other causes include almost everything on this list, or kernicterus.
Again, the most common anatomic correlate is periventricular leukomalacia (quantitating it: Brain 128: 2562, 2005). In the term infant with hemiplegia, the usual finding is either a malformation, or ulegyria or some other ischemic brain injury (sometimes just neuronal loss and gliosis), often in the distribution of one or both middle cerebral arteries (update Pediatrics: 118, 690, 2008).
Neuroimaging has revolutionized the study of brain injury in babies (Pediatrics 121: 906, 2008).
Premature birth is a major risk factor for cerebral palsy. For those weighing less than 1500 gm at birth, the risk is 30x that for term babies. Those under 2500 gm are also at increased risk, though less so. Again, in preemies who go on to develop cerebral palsy, the usual lesion is periventricular leukomalacia (JAMA 296: 1602 & 1650, 2006).
Children produced by in-vitro fertilization are at greater risk, but mostly just because they are more likely to be born prematurely and/or with low birth weight (Lancet 359: 461, 2002). Of course, meningitis in the neonate is another cause (Clin. Ped. 40: 473, 2001).
* For a still-helpul review of cerebral palsy, see NEJM 330: 188, 1994.
* "Cranial osteopathy" shows no benefit whatever in kids with cerebral palsy: Arch. Dis. Child. 96: 505, 2011.
{33069} cerebral palsy from birth hypoxia
{18763} kernicterus
{31972} kernicterus
{31989} kernicterus
{53734} kernicterus after-effects (small head)
Again, most developmental abnormalities of the brain are not inherited, and are of unknown etiology.
CELLULAR REACTIONS IN THE NERVOUS SYSTEM
|
|
|
|
|
|
|  |
Histology terms:
NISSL SUBSTANCE is just rough endoplasmic reticulum in neurons. It's easy to see using special stains.
NEUROFILAMENTS are intermediate filaments typical of neurons.
NEURONAL DROPOUT (nerve cell depopulation) is important in many disorders.
{01278} red neurons
{01279} red neurons
{31969} red neurons (Purkinje cells are dead)
ATROPHY AND DEGENERATION OF NEURONS is common in many neuronal diseases, and (to a much lesser degree) in simple aging.
Most of the time, loss of a single neuron provokes no reaction from adjacent glia, or any other specific morphologic marker.
Sometimes, loss of a neuron produces TRANS-SYNAPTIC DEGENERATION of the neurons with which it communicates. The best example is atrophy of the lateral geniculate body in people who have had an eye enuclated.
INTRA-NEURONAL BODIES (many of them characteristic of the "proteinopathies", a new fad name) include the following:
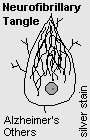
NEUROFIBRILLARY TANGLES are structures composed of twisted filaments, stainable with silver. They are composed of tau protein, ubiquitin, and sometimes Aβ (Neurology 40: 975, 1990). The immunostain for phosphorylated tau (formerly Alz-50) shows them up especially well.
Neurofibrillary tangles are typical of Alzheimer's disease, progressive supranuclear palsy, corticobasal degeneration, post-encephalitic Parkinsonism, amyotrophic lateral sclerosis of Guam, dementia of boxers, * Williams' microdeletion (Arch. Neuro. 52: 209, 1995), and bad * Niemann-Pick storage disease (Brain 118(1): 119, 1995).
|
{01288} neurofibrillary tangles; the stringy stuff in the neuron
is stained poorly here
{01291} neurofibrillary tangles; the black, stringy stuff in the neurons |
 |
|
LEWY BODIES are pink-staining spheroids made largely of ubiquitin,
parkin, and synuclein.
They are typical of idiopathic
Parkinson's disease (substantia nigra) and Lewy-body dementia (large numbers
in the cortex).
|  |
{01330} Lewy body
| PICK BODIES are large, ovoid intracytoplasmic bodies that stain best with silver. They're made of tau protein. On EM, they appear filamentous. A true Pick body lights up for phosphorylated tau. Other inclusions in frontotemporal dementia proved to be tau-negative, ubiquitin-positive, a discovery that led to the separation of the frontotemporal lobe dementias: Arch. Neuro 51: 145, 1994 -- much more later. | 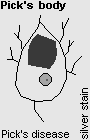 |
{01311} Pick body (the large black thing)
| BALLOON CELLS, swollen for unknown reason, are typical of Pick's and some of its variants, tuberous sclerosis, the cortical dysplasia that's infamous for childhood epilepsy, and corticobasal degeneration. They often stain both as neurons and glia, and no one's sure which they are (update Brain 130: 2267, 2007). |  |
| SPONGIFORM CHANGE (not to be confused with spongiosis, an obsolete word for edema and reactive astrocytes after brain injury) consists of watery vacuoles in the perikaryons and processes of neurons. It's typical of the prion diseases. | 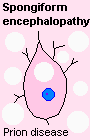 |
HIRANO BODIES are hyaline masses composed primarily of actin. They are typical of Alzheimer's
disease but occasionally pop up in a variety of cells in a variety of illnesses.
Look in the hippocampus.
|  |
{01303} Hirano body (you need EM to appreciate the corduroy effect)
| GRANULOVACUOLAR DEGENERATION appears as tiny vesicles with central, dense cores. It is typical of Alzheimer's disease. | 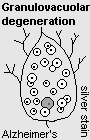 |
{01293} Granulovacuolar degeneration
LAFORA BODIES are masses of glucose polymer, mostly within neurons
(also liver and muscle; look especially in the dentate nucleus of the
brain). They are typical of the common hereditary form of
myoclonus
epilepsy (* gene "laforin" / EPM2A).
|  |
{01314} Lafora body (PAS stain, "red sunflower")
* Neuroserpin forms bodies in a rare autosomal dominant illness (Am. J. Path. 170: 1305, 2007).
* MARINESCO BODIES are small red ubiquitin-rich in the nucleus, without a halo. Usually you see them in pigmented neurons of the locus ceruleus / substantia nigra. Their significance is unclear.
| NEGRI BODIES in the cytoplasm in rabies |  |
|
|
|
|
![]() Rabies
Rabies
Negri bodies
Wikimedia Commons
MELANIN is normal in the substantia nigra, locus ceruleus, and dorsal motor nucleus of the vagus nerve.
{01272} neuromelanin
LIPOFUSCIN is common in older people (* "simple pigmentary atrophy").
{01270} lipofuscin; oil red O stain
INTRA-NEURONAL STORAGE is characteristic of certain inborn errors of metabolism (listed below). The cytoplasm is distended, and the nucleus typically appears displaced.
* FERRUGINATION is hemosiderin-encrustation of neurons near sites of past hemorrhage.
|
AXONAL REACTION is also known as CENTRAL CHROMATOLYSIS. If an axon is severed or otherwise injured, the perikaryon (neuronal cell body) swells, rounds up and becomes pale-staining. The Nissl substance disappears except just below the cell membrane, and the nucleus moves to the edge of the cell. * "Peripheral chromatolysis": The neuron is recovering! * Healthy Clarke's column and some other neuron groups can show central chromatolysis for some reason.
|  |
{01275} axonal reaction, central chromatolysis; you
can just see the RER as purple at the rims of the affected neurons
{01276} axonal reaction, central chromatolysis
AXONAL DEGENERATION is said to occur when a neuron cannot maintain the axon to which it is attached.
WALLERIAN DEGENERATION is the changes in an axon severed from its cell body.
{09602} Wallerian degeneration; corticospinal
tract is lost from a stroke higher up
{09591} Wallerian degeneration, corticospinal tract
is lost from a stroke higher up (myelin stain)
![]() Wallerian degeneration
Wallerian degeneration
WebPath Photo
AXONAL SPHEROIDS are spherical or sausage-shaped knobs when axons have been damaged by mechanical trauma ("diffuse axonal injury", the main lesion), ischemia, radiation (famous), or in axonal diseases.
* Clinicians please note: The term "Betz cells", used as a synonym for cortical neurons ("You have two Betz cells held together by an ethanol molecule / spirochete"), should be limited to the large cortical neurons that supply axons to the descending pathways.
| ASTROCYTES show on H&E only as relatively large glial nuclei in the neuropil. | 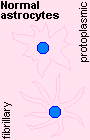 |
You remember that PROTOPLASMIC ASTROCYTES occur mostly in gray matter, FIBROUS ASTROCYTES occur mostly in white matter, and that their "foot processes" / "end plates" have to do with the blood-brain barrier.
The intermediate filaments in astrocytes are vimentin and GLIAL FIBRILLARY ACID PROTEIN (GFAP, a specific marker).
GLIOSIS is hypertrophy and proliferation of astrocytes at sites of injury, the counterpart of "scarring" elsewhere in the body.
Instead of laying down collagen or other extracellular material, the astrocyte cytoplasm itself becomes the "scar". There is still some "scar contraction" though not so much as in collagenous scar.
{01366} gliosis, special glial stain
{01368} gliosis, special glial stain
|
The only fibroblasts in the CNS are in the blood vessels, and these typically only contribute to healing when a hematoma must be organized or an abscess walled off.
* The clever pathologist distinguishes the wall of an abscess from a glioblastoma by observing that fibroblasts do not stain with GFAP, while spindle cell astrocytes do.
Gliotic scars, especially after penetrating injury, are considered to give rise to many cases of epilepsy. They're composed mostly of fibrillary astrocytes of course.
| GEMISTOCYTES are astrocytes seen in reactive processes. They are large, pink cells. |  |
{01357} gemistocytes
{01360} gemistocytes
FIBRILLARY ASTROCYTES (not to be confused with fibrous astrocytes, a normal cell) result when gemistocytes settle downward lose most of their cytoplasm, though not the complexity of their processes.
ANISOMORPHIC GLIOSIS is a proliferation of neoplastic, slightly-atypical protoplasmic astrocytes, the lowest-grade of astrocytoma.
ROSENTHAL FIBERS are pink-staining structures within the processes of large astrocytes. They are shaped like slightly-crumpled hot-dogs. You can see them at any site of gliosis / gliotic scar, and they help make the diagnosis of certain astrocytomas.
{01390} Rosenthal fibers
{01393} Rosenthal fibers in * Alexander's disease (mutant GFAP;
worked out Nat. Genet. 27: 117, 2001)
* CORPORA AMYLACEA ("polyglucosan bodies"; "fool's cryptococcus") are 10-50 spherical masses of polysaccharide within astrocyte end-processes. They become common as the brain ages; look for them in the subependymal and perivascular regions.
| ALZHEIMER'S TYPE I GLIA are monstrously enlarged astrocytes with huge, dark nuclei. You seen them in subacute sclerosing panencephalitis (SSPE) and progressive multifocal leukoencephalopathy. | 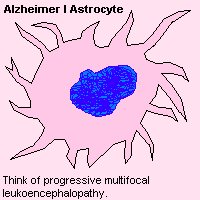 |
ALZHEIMER"S TYPE II GLIA are astrocytes with edematous-looking, swollen nuclei. They
are seen in
liver failure and other states with high blood ammonia
(Reye's, urea cycle problems). Look in the gray matter, especially the thalamus.
|  |
{00539} Alzheimer's type II glia (two of them)
{01383} Alzheimer's type II glia (one in the center)
NOTE: Neither type of "Alzheimer's glia" has anything to do with Alzheimer's disease.
* DECREASED NUMBERS OF ASTROCYTES is a maker for longstanding mild ischemia.
OLIGODENDROGLIA have small, lymphocyte-like nuclei with a halo (* formalin artifact).
They are primarily responsible for making myelin; unlike the Schwann cell, one oligodendrocyte can wrap several axons. In the white matter, they are easy to spot. In the gray matter, look for them around neurons ("satellite cells").
Diseases of oligodendroglia affect myelin. LEUKODYSTROPHIES affect all myelin, and are usually hereditary. DEMYELINATING DISEASES produce patchy myelin loss. You remember that PERIVENTRICULAR LEUKOMALACIA, the usual lesion in cerebral palsy, features loss of oligodendroglia around the ventricles. SCLEROSIS in CNS means loss of myelin and its replacement by astrocytes.
Morphologically, the reactions of oligodendroglia are usually limited to dying and disappearing.
Herpes![]() and JC viruses produce typical inclusions
and JC viruses produce typical inclusions![]() in oligodendroglia; chronic measles
in oligodendroglia; chronic measles![]() (SSPE)
may do so as well.
(SSPE)
may do so as well.
Cytoplasmic inclusions in the oligodendroglia (* Papp-Lantos inclusions) are masses of scrambled microtubules, specific for the multiple systems atrophy family (Shy-Drager, striatonigral degeneration, some cases of olivopontocerebellar degeneration). See Am. J. Path. 155: 1241, 1999. They are composed of synuclein, alphaB-crystallin, and ubiquitin. You won't see Lewy bodies.
EPENDYMA seldom show much reaction, either. If ependymal cells die, gliosis between the cells produces EPENDYMAL GRANULATIONS.
MICROGLIA is an ancient misnomer for macrophages in the brain. (* Philologists: Astrocytes and oligodendroglia are "macroglia".)
GITTER CELLS are actively phagocytizing macrophages in the CNS. They are typically "gitting" rid of dead myelin and other cell debris.
MICROGLIAL NODULES are clusters of macrophages around damaged tissue. Think of viral or rickettsial disease. (Don't expect to see good granulomas in diseases unique to the CNS.) You may actually see the macrophages eating neurons (NEURONOPHAGIA, naturally).
HIV GIANT CELLS are the familiar Langhans / foreign body type resulting from macrophages that fuse in HIV infection. They notice the HIV gp120 on each other's surfaces, and try to engulf each other.
|
|
{01461} neuronophagia
* Despite old teachings, there are always a few T-cells on patrol in the brain, and even finding a group of B-cells doesn't necessarily mean disease (Brain 126: 1058, 2003).
Worth noting: Neurons are very sensitive to ischemia (worst) and hypoxia (somewhat better tolerated as long as there's blood flow, but still not good). Oligodendroglia are less sensitive than are neurons. Ependymal cells are even less sensitive, while astrocytes are the least sensitive, capable of withstanding all but the most severe and prolonged hypoxia.
INCREASED INTRACRANIAL PRESSURE / HERNIATION
|
|
|
Increased intracranial pressure is said to be present when recumbent CSF pressure exceeds 200 mm water.
You know it's best to be cautious doing a lumbar puncture if there's a known or possible mass lesion in the cranial cavity -- the brainstem can hernia, causing instant death. If you do perform a lumbar puncture, you will measure the CSF pressure using the manometer during the procedure.
When brain volume (localized or generalized) increases for any reason (edema, trauma, hemorrhage, tumor, inflammation, abscess, echinococcus, gumma, etc.), some blood is first pushed out of the skull by venous compression, but this is minuscule. Any additional increase in brain volume will increase intracranial pressure. Some CSF will be lost, and then the brain itself will be forced to move within the skull.
Increased intracranial pressure first presents as headache, mental dullness, and nausea and vomiting (the latter are important and are curiously omitted from "Big Robbins"). Clinicians of course look for papilledema, pushing of the optic nerve forward into the eyeball.
The skull and even dural membranes are not going to budge for the expanding brain. Instead, HERNIATION will occur when brain volume is sufficiently increased. (The brain is being squeezed through openings and around corners like toothpaste.)
CINGULATE HERNIATION (SUBFALCINE HERNIATION) results when one cingulate gyrus is pushed underneath the falx. Occlusion of the callosal-marginal branch of the anterior cerebral artery can result.
{01465} cingulate herniation, view from above with falx removed
*Future angiographers: Detect these by finding displacement of the pericallosal arteries!
UNCAL HERNIATION (TRANS-TENTORIAL HERNIATION, HIPPOCAMPAL HERNIATION) results when the medial temporal lobe is pushed between the cerebral peduncles and the tentorium cerebelli.
{01471} tentorial herniation marks
{31975} Herniation marks
{01473} tentorial herniation marks
{01482} tentorial herniation marks
{00524} tentorial herniation, crushed cerebral peduncle
{00542} tentorial herniation, crushed cerebral peduncle
Stretching of the third cranial nerve produces the famous "fixed dilated pupil" on the IPSILATERAL side.
Crushing of the posterior cerebral artery against the edge of the tentorium results in occlusion, and explains the cortical blindness (if unilateral, "homonymous hemianopsia") that often follows head injury.
{01483} crushed posterior cerebral artery
Crushing of the cerebral peduncle on the same side as the expanding lesion causes hemiparesis on the opposite side of the body.
* You may also note paralysis of upward gaze (injury to the tectum) or sudden increase in intracranial pressure (crushing shut of the aqueduct of Sylvius), and so forth.
* Expanding lesions in the posterior fossa can give REVERSE TENTORIAL HERNIATION. This causes many of the signs above, and the tension on the fifth cranial nerves is painful.
* If there is bilateral uncal / tentorial herniation, we speak of "central herniation."
{01477} reverse tentorial herniation marks
TONSILLAR HERNIATION (CEREBELLAR HERNIATION, BRAINSTEM HERNIATION, CONING) results from herniation of the cerebellar tonsils out through the foramen magnum, compressing the medulla. The latter is the mechanism of death in most cases of brain swelling. It can also happen immediately if the brain is struck by one of today's high-velocity bullets.
{01474} tonsillar herniation damage
{01476} tonsillar herniation damage
![]() Tonsillar herniation
Tonsillar herniation
"Coning"
WebPath Photo
As the brainstem is pushed caudally, the penetrating vessels are affected, resulting in the centrally-located DÛRET HEMORRHAGES ("Duret hemorrhages", "secondary brainstem hemorrhages", "slit hemorrhages") in the pons and midbrain. This is bad, and can leave a survivor locked-in.
{01485} Dûret hemorrhage
* "Big Robbins" states the vessels are avulsed, causing hemorrhage. Or maybe they are occluded by stretching, and then the ischemic regions become hemorrhagic when re-perfused during heroic resuscitation attempts.
TRANS-CALVARIAL HERNIATION is said to be present when brain herniates out through an open fracture in the skull.
{01479} trans-calvarial herniation after-effect
Other causes of increased central venous pressure (cardiac septal defects, congestive heart failure, AV malformations) or obstruction to the venous outflow from the brain (i.e., little thrombi from hypercoagulable blood) also need to be considered.
* You will learn on rotations about surgery (shunts, optic nerve fenestration, now dural stents J. Neurosurg. 116: 538, 2012) for this relatively common clinical problem.
CEREBRAL EDEMA
Brain swelling is serious, since it leads to herniation (and maybe scrambles the neuropil, too.) Three types are classically listed.
VASOGENIC EDEMA (the most common type) is fluid in the extracellular space. Either (1) the capillaries have been damaged and are leaking protein (developing infarcts, infection, contusions, radiation injury, and notoriously lead poisoning though no one knows how Pb damages the endothelium) or (2) new, leaky capillaries are forming in an abnormal area (abscess, primary or metastatic tumor).
On imaging, the edema fluid may flow up the path of least resistance along the white matter tracts.
Grossly, the white matter will be soft and wet, and more affected than gray (since the intercellular space is larger in the white matter).
Microscopically, in vasogenic edema there are little vacuoles throughout the white matter. Also look for expansion of the Virchow-Robin spaces. If longstanding, axons degenerate and myelin is lost.
Note that this sort of edema will light up on enhanced scans (ask a neuro-radiologist about "ring enhancement" around tumors and abscesses.)
* Acute mountain sickness features ("high-altitude cerebral edema") is vasogenic cerebral edema, which now appears to be due to the vessels in the white matter becoming leaky (JAMA 280: 1920, 1998; update Lancet 361: 1967, 2003). Is high-altitude mountain climbing itself a risk factor for permanent brain damage? First systematic survey indicates "Yes": Am. J. Med. 119: 168.e1, 2006.
* Radiation injury to the brain may be unavoidable in people radiated for head-and-neck cancer. Edema in a patch of necrosis can cause mass effect and require surgical intervention (J. Neurosurg. 113: 293, 2010).
{01464} edema after trauma
{01344} vasogenic edema, note bubbles
{01345} vasogenic edema, note bubbles
{01438} vasogenic edema, note bubbles
Worth remembering: Cerebral edema can kill a child or teen even after a blow that does not cause loss of consciousness. Team doctors began noticing this in the 1970's (JAMA 266: 2867, 1991). Especially, remember SECOND IMPACT SYNDROME, in which a second blow to the head sustained in a person who's recently had a concussion causes disastrous edema.
| * His fans blame the aspirin he took for a headache and/or some paranormal martial-arts phenomenon. But Bruce Lee's death sounds like an example of this. He had been sparring during the day, felt sick and lay down, and was found dead of massive, unexplained cerebral edema. |
 Bruce Lee |
In the mouse model, the window of vulnerability for second-impact syndrome is 3-5 days (Neurosurg. 56: 364, 2005, photomicrographs). See below.
CYTOTOXIC EDEMA ("cytotoxic swelling" might be better) means excessive intracellular water, indicating cells have been damaged. The cell membranes of astrocytes become permeable to sodium, and water follows it in. The blood-brain barrier is intact, at least for now. Look for this in early ischemia, acidosis/hypercarbia, Reye's, and pseudotumor cerebri.
Grossly, the gray matter will be more affected, since that's where the business astrocytes cells are. Mass effect is much less than in vasogenic edema.
Microscopically, look for swelling and vacuolization of individual cells.
As you would expect, cytotoxic and vasogenic edema often occur at the same time. In an infarct, for example, cytotoxic edema occurs early (as the brain cells are dying), and vasogenic edema follows (as the endothelial cells are dying).
* Future radiologists: Of course the apparent diffusion coefficient (ADC) on diffusion MRI will be low in cytotoxic swelling, high in vasogenic edema.
INTERSTITIAL EDEMA ("transependymal edema") results from obstruction of the flow of spinal fluid ("non-communicating hydrocephalus"). CSF is forced across the ependyma, and the edema surrounds the ventricles.
* OSMOTIC EDEMA happens when the plasma is greatly diluted, as in way-out-of-control ketoacidosis.
In edema of any kind, expect to see flattening of the gyri against the skull, and narrowing of the sulci.
HYDROCEPHALUS ("water-heads")
|
|
You remember that CSF is produced by the choroid plexus within the ventricles, flows through the brain and out the foramina of Luschka and Magendie, and is resorbed at the arachnoid villi.
NON-COMMUNICATING HYDROCEPHALUS results form blockage within the brain. These problems may be
congenital (stenosis or malformation of the aqueduct of Sylvius, Dandy-Walker, Arnold-Chiari, fetal
CMV![]() )
or acquired (tumors, meningitis with ventriculitis, large intracerebral bleeds or shifts
compressing a foramen of Munro).
)
or acquired (tumors, meningitis with ventriculitis, large intracerebral bleeds or shifts
compressing a foramen of Munro).
COMMUNICATING HYDROCEPHALUS results from over-production of CSF (choroid plexus papilloma),
obstruction in the subarachnoid space (i.e., after bacterial or tuberculous![]() meningitis or subarachnoid
hemorrhage) or problems with the arachnoid villi (i.e., dural sinus thrombosis).
meningitis or subarachnoid
hemorrhage) or problems with the arachnoid villi (i.e., dural sinus thrombosis).
{00191} hydrocephalic child
HYDROCEPHALUS EX VACUO means nothing more nor less than brain atrophy from cell loss. There are fewer cells, and more room for fluid. This may be due to atrophy, or to loss of brain from infarct or injury.
{32766} atrophy, attributed to alcoholism
![]() Hydrocephalus ex vacuo
Hydrocephalus ex vacuo
WebPath Photo
Regardless of etiology, all forms of hydrocephalus produce enlarged ventricles.
Before the sutures fuse (i.e., in young children), untreated hydrocephalus produces huge heads. Traction on the optic nerves forces downward gaze ("the setting sun sign"). Up to 1 child in 1000 has obstrcutive hydrocephalus (Ped. Neurosurg. 32: 119, 2000); today, the disastrous outcome is preventable by spinal fluid shunting.
{00191} hydrocephalic child
{13394} hydrocephalus
{13395} hydrocephalus, transilluminated
{00194} hydrocephalic brain
{00197} hydrocephalic brain
In adults, rapidly-progressive hydrocephalus produces rapidly increasing intracranial pressure. If the onset is more slow, patients merely suffer dementia.
The entity "normal pressure hydrocephalus", with dementia, apraxia of gait, and urinary incontinence, is now known to be caused by a failure of the arachnoid granulations to keep up with the choroid plexus (Am. Fam. Phys. 70: 1071, 2004). It gets treated empirically with ventricular shunting, usually with good results.
If increased intracranial pressure is severe, fluid will be forced through the ependyma ("interstitial edema"; see above).
Physicians: Please don't miss CSF LEAKS, following surgery or trauma. Fluid running out of the nose or ear is spinal fluid until proved otherwise. You can confirm your impression with a glucose reagent pad. (Remember that spinal fluid contains glucose, while snot does not.) The hard-core may check for beta-2 transferrin which is a marker for CSF.
HYPOXIA, ISCHEMIA, AND INFARCTION
{09443} atherosclerosis of major arteries
{53786} perinatal hypoxia case
|
|
|
You are already familiar with the various types of hypoxia ("anoxia"), and with the causes of hypoglycemia.
The brain tolerates ischemia (low blood flow) very poorly, and much "brain damage from lack of oxygen" is probably due in large part to damage from low pH (i.e., when there is no blood to remove by-products of metabolism from the brain).
You already know that incomplete infarction (i.e., a few minutes without
blood flow) will be enough to kill neurons but will not
liquefy![]() the brain.
The brain will remain solid if perfusion is restored within a few hours, since
the glia will survive.
the brain.
The brain will remain solid if perfusion is restored within a few hours, since
the glia will survive.
Why the brain should be so vulnerable to poor perfusion is mysterious.
There's no question that under some conditions, glutamate- and aspartate-based synapses getting stuck in the "on" position, allowing influx of calcium ("excitotoxicity"), harming the cell. It seems unlikely (as was once thought) that this has much to do with neurodegenerative disease (I still wonder about schizophrenia as do others Eur. J. Pharm. 682: 1, 2012), but it's probably a component of ischemic injury. Drugs have been under investigation for the past two decades to prevent cell death from excitotoxicity; no miracles yet. Still good reading: Science 268: 239, 1995.
The reason for brain damage following hypoglycemia is even less-well understood. The morphology is the same as "hypoxic encephalopathy".
Full necrosis (neurons and glia, liquid) of the brain following ischemic injury is called ENCEPHALOMALACIA (literally, "brain-softening"; remember that other things can make the brain soft).
{31968} widespread encephalomalacia, recent (purple / "lilac" cortex)
ISCHEMIC / HYPOXIC ENCEPHALOPATHY is said to be present when the whole brain has suffered the effects of poor perfusion.
In people with good arteries, there is no compromise of cerebral blood flow until systemic blood pressure drops below 50 mmHg. People with narrowed arteries (usually from atherosclerosis) can have brain damage following less severe drops in pressure.
The clinicians are finally recognizing what the public has known for a long time: that cardiopulmonary bypass carries a real risk of subtle temporary or permanent brain damage ("pump head", Ann. Thorac. Surg. 59: 1296, 1312, 1336 & 1340, 1995).
The morphology is generalized brain ischemia is familiar to general autopsy pathologists.
By twelve hours after the insult, you'll probably be able to see "red neurons".
The pyramidal cell layers of the cerebral cortex are much more severely affected than the other layers, so that milder degrees of ischemic produce LAMINAR NECROSIS. The most vulnerable area of cortex is probably the h1 segment of the hippocampus. In the neocortex, look for liquefaction of layers III & maybe V.
{00168} laminar necrosis; this is the slit running down the middle of the cortex,
due to hypoxic damage long ago
{17731} laminar necrosis
In hypoxia due to poor perfusion (i.e., in shock survivors), the obvious necrosis may even be limited to the WATERSHED ZONES ("BORDER ZONES") between the distributions of the major arteries. Look for necrosis adjacent to the sagittal sinus, curving laterally over the outer surfaces of the occipital lobes.
Survivors of shock and/or respiratory failure during critical illness are often brain-damaged for the rest of their lives, especially if delirium has been present. See NEJM 369: 1306, 2013.
{09604} watershed infarcts; you diagnose this by location
{09607} watershed infarcts
![]() Watershed infarcts
Watershed infarcts
WebPath Photo
There is another border zone in the upper lumbar spinal cord, and paraplegia can follow a hypoxic episode.
The degree of recovery of function depends on a number of variables. These include:
Survivors may experience anything from transient confusion to persistent vegetative state or "brain death" ("apallic state").
While the classic teaching is that the brain can withstand 3 minutes of poor perfusion "without damage", this assumes (wrongly) that a morphologically normal brain is a functionally normal brain.
Anecdotally, "high-functioning" people have found themselves disabled after as little as 15 seconds of cardiac arrest; measurable brain damage follows most away-from-the-defibrillator cardiac arrests (Br. Med. J. 313: 143, 1996).
Pathology of "persistent vegetative state" (survivals 1 month to 8 years): Brain 123: 1327, 2000. It is not rare for the cortex to be normal, but the thalamus and/or the deep white are never normal.
{00165} diffuse hypoxic-ischemic injury, old; note the laminar necrosis
{33033} diffuse hypoxic-ischemic injury, old
{31970} diffuse hypoxic-ischemic injury, old
![]() Diffuse hypoxic-ischemic injury
Diffuse hypoxic-ischemic injury
Old; patient kept alive on respirator
WebPath Photo
The most severe variant is SPONGE BRAIN ("multi-cystic brain"), in infants who have severe hypoxic-ischemic injury around the time of birth but are kept alive for weeks afterwards.
{15469} sponge brain
* Your lecturer is no expert on neurology or rehabilitation, but from what he's observed as a physician, he shares a widespread concern about the cost-effectiveness of "neuro rehab" for the profoundly injured. See Lancet 357: 410, 2001 for a bitter editorial on the failure to show any benefit for neurodegenerative disease; the sorry truth about stroke rehab is summarized in Stroke 34: 801, 2003. Even in the most upeat reports of stroke rehabilitation, the benefits seem small (Lancet 377: 1693, 2011). Even Sweden's physicians cannot agree whether patients in persistent vegetative state should "always" or "never" be sent to "neuro rehab" (Am. J. Phys. Med. Rehab. 90: 482, 2011), or what the benefits to the individual or community may be. If you have other information, I'd like to hear about it. One of my correspondents (2009), a neuro nurse with much experience, was impressed anecdotally, and suggests that it might reasonably be taught to and tried by family members. Anyone with clinical experience will recognize the wisdom of her last remark: "Also, the hope the family has is sometimes all they have, and puttng their loved one through the motions can give the family something to do, some control and if it helps, less reliance on caregivers."
CEREBRAL INFARCTS
"Stroke", the sudden onset of a permanent, localized neurologic deficit, may result either from infarction or hemorrhage, and has a multitude of specific causes. The most common cause of stroke (75%) is cerebral infarction (annual incidence 190 per 100,000 people per year).
|
|
Infarcts have many causes.
THROMBOTIC INFARCTS usually result from atherosclerosis, when a plaque ruptures. Favored sites are the carotid bifurcations and the vertebrobasilar system.
EMBOLIC INFARCTS typically result from atheroemboli or emboli from intracardiac thrombi (i.e., thrombi from fibrillating atria, mural thrombi over old infarcts). Especially, remembers an ulcerated atherosclerotic plaque in the ascending aorta. See NEJM 334: 2126, 1996; Am. Heart J. 139: 329, 2000). Emboli most often go to one or the other middle cerebral artery.
In a kid with a stroke, think of patent foramen ovale and pulmonary hypertension (* easy screen using trans-esophageal sonography: Am. J. Card. 74: 381, 1994; still an important problem Heart 98: 485, 2012).
Nobody understands why for sure, but current smoking greatly increases your risk of stroke (Ann. Int. Med. 120: 458, 1994).
* Some folks lack one or both posterior communicating arteries, and these people are much more vulnerable to embolic stroke (i.e., no collaterals): NEJM 330: 1565, 1992.
* Over the past few years, measuring the thickness of the carotid intima via ultrasound has become popular. It's known to correlate with risk for heart attack and stroke, but despite its being promoted as an "independent risk factor", it is probably worthless when the other risk factors are taken into account. By the way, this tells me that all the important risk factors for heart attack and stroke have been discovered (Lancet 380: 2053, 2012).
You also remember that the little arteries that supply the thalamus and basal ganglia don't have collateral circulation, so little strokes here are common.
We have already seen infarcts due to compression of vessels during herniation, and "border zone infarcts / watershed infarcts" in which there is hypoperfusion but no obstruction.
You already know SUBCLAVIAN STEAL SYNDROME (Robin Hood syndrome, etc.), in which a patient with occlusive atherosclerosis of a proximal subclavian artery suffers brainstem syndromes upon exercising the arm on the involved side. The arm is being perfused via blood that goes up the contralateral vertebral artery, and back down the ipsilateral one.
* (Primary) GRANULOMATOUS ANGIITIS OF THE CNS is a thankfully rare entity that may be suspected on scan, but needs confirmation on leptomeningeal biopsy (Neurology 53: 858, 1999). Immunosuppression (as for Wegener's and polyarteritis nodosa) is the basis of treatment.
MOYAMOYA DISEASE, a poorly-understood process in which the vessels of the circle of Willis and nearby become narrowed (fibrosis of the intima) and may also bleed (fragile new vessels sprout), is yet another cause of stroke. This is fairly common in both children and adults (J. Neurosurg. 77: 84, 1992; J. Neurosurg. 80: 328, 1994; Arch. Neuro. 58: 1274, 2001). The etiology is still obscure; it may occur in syndromes (Am. J. Op. 127: 356, 1999), including Down's and sicklers, and a gene is known (Neurology 78: 803, 2012). Prognosis after a pial revascularization procedure is excellent: J. Neurosurg. 100(S2): 142-9, 2004; J. Neurosurg. 111: 927, 2009. Update NEJM 360: 1226, 2009.
CADASIL, or cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy, is a grisly disease caused by buildup of granular material in the basement membranes between the smooth muscles of arterial walls. The diagnosis is made when the pathologist examines a skin biopsy. The arteries have fragmented internal elastic membranes and basophilic, PAS-positive granules throughout their walls. It is underdiagnosed; this may change since there is supposedly a pathognomonic MRI. The gene's name is Notch3. See Lancet 350: 1490, 1997, Nature 383: 707, 1996; alleles Brain 132: 1601, 2009; Arch. Neuro. 68: 1584, 2011; anatomic pathology Neurology 51: 844, 1998. Progressive loss of cognitive function correlates with the little strokes and bleeds (Neurology 72: 143, 2009).
* SUSAC SYNDROME ("retinocochleocerebral vasculopathy"; Medicine 77: 3, 1998); is another, thankfully rare (but perhaps underdiagnosed) syndrome of small vessel spasm in the eye, inner ear, and brain (famously the corpus callosum). The physician will see occlusions of branches of the retinal artery plus sensorineural hearing loss. It usually affects young adult women and vanishes after a year or so. It appears to be caused by autoantibodies against endothelium which seem specific and may someday define the disease (Am. J. Clin. Path. 136: 903, 2011.)
Future hematologists: Remember LEUKOSTATIC INFARCTS throughout the brain when the white count is extremely high and stops up the microvasculature (i.e., chronic granulocytic leukemia).
The ability to survive a stroke depends on the availability of collateral flow.
For example, an intact circle of Willis supplied by good arteries renders complete occlusion of a carotid artery innocuous, and collateral flow from the anterior cerebral artery may protect much brain during occlusion of the middle cerebral artery. (Basilar artery atherosclerosis, however, generally cannot be overcome by good collateral flow).
For some reason, the small, deep-brain cerebral arteries do not anastomose much. When one is occluded, an infarct is inevitable. This is unfortunate, since these arteries supply such key structures as the internal capsule.
The classic brain infarct is ISCHEMIC ("anemic", "bland"), and the morphologic changes are stereotyped.
Six to twelve hours after the "stroke", the brain becomes slightly discolored and soft, blurring the gray-white junction. You usually see at least a few petechiae at the edges (why?).
Two to three days after the "stroke", the cerebral matter becomes very soft, and starts to break up. At this time, surrounding edema may be quite severe, enough to produce herniation.
{00180} infarct with early softening
{17792} infarct with early softening
|
|
|
Australian Pathology Museum High-tech gross photos
|
As the infarct heals, the dead tissue liquifies, leaving a cavity that is typically still crisscrossed by little surviving blood vessels. The overlying leptomeninges (when involved) become thick and form the roof of the cavity. It takes months for a big infarct to transform into a RESIDUAL CAVITY ("cyst", a time-honored misnomer).
{00189} infarct, breaking apart
{06348} infarct, old; frontotemporal area
{10350} infarcts, old and recent
{10960} infarct, old, basal ganglia
{17694} infarct, old
![]() Fresh stroke
Fresh stroke
Some small hemorrhages
Wikimedia Commons
Recovery of function after a cerebral infarct (or hemorrhage) is due largely to resorption of edema fluid.
Microscopically, polys and then macrophages clean up the debris, just as in a myocardial infarct. Unlike in the rest of the body, the macrophages stay around for years. Instead of a fibrous scar, the infarct is surrounded by gliosis.
HEMORRHAGIC INFARCTS are "anemic infarcts" complicated by dissolution of an embolus or backflow of blood from the margins. The result is perfusion of non-viable blood vessels, which rupture.
Hemorrhagic infarcts consist of lots of petechiae (since the vessels that break are capillaries); they may be confined to the gray matter (the vessels in white matter typically do not rupture in this setting).
* The traditional wisdom is that "emboli cause hemorrhagic infarcts, thrombi forming in situ cause pale infarcts." An embolus produces sudden, complete occlusion, which is likely to kill off the vessels as well. A thrombus forming slowly -- perhaps with stuttering clinical symptoms -- may give the brain time to adapt and let the small vessels survive.
{18760} hemorrhagic infarct; note it consists of petechiae
{00145} hemorrhagic infarct
Of course, if somebody anticoagulated the patient, the hemorrhage will be much more impressive and dangerous. Anticoagulation is a two-edged weapon in stroke.
VENOUS INFARCTS result from hypercoagulable states (remember polycythemia vera, sickle cell disease, lupus anticoagulant, and the post-partum state in adults, and dehydration in children) or infected (TB, H. 'flu, others) venous sinuses. Infarction will not occur without thrombosis either of very large venous sinuses or many small veins. The typical case shows hemorrhagic infarction, symmetrically around the superior sagittal sinus.
{15696} venous infarct
{15697} venous infarct
| * Lenin's brain contained multiple, bilateral, old infarcts. See Neurology 42: 241, 1992. This disproves his friend Maxim Gorky's maxim that a bad person needs a good brain. |

|
INTRACEREBRAL HEMORRHAGE
|
|
|
There are many different types of brain hemorrhages. Some rules:
Blood in the ventricles is noxious, and if the fourth ventricle is suddenly dilated under pressure, death results.
Blood in the subarachnoid space is excruciatingly painful.
Bleeding in the brain substance itself is more subtle, and can present merely as nausea.
Fresh bleeding produces spinal fluid of normal color, or slightly pink. Xanthochromia results when breakdown products of hemoglobin stain the CSF yellowish.
Bleeding into the brain substance is attributed to a variety of causes.
NOTE: This "clinical truism" ("He popped his cork!") is disputed by some autopsy pathologists who note that there is a reflex rise in systemic blood pressure when intracranial pressure rises ("Cushing reflex", remember?), and that victims of intracranial hemorrhage often lack other stigmata of longstanding systemic hypertension (i.e., no big heart, no bad kidneys). Wait for my series -- so far, mine all have cardiac hypertrophy from high blood pressure.
Taking all these causes together, these bleeds are fairly common, with an incidence of 35 per 100,000 people per year.
The classic "hypertensive" hemorrhage (whether or not hypertension is the cause) is classically thought to result from rupture of a little "Charcot-Bouchard" micro-aneurysm (<=2-3 mm) on the trunks and at the bifurcations of small intracerebral arteries. We do not know why these form, and we don't know whether hypertension contributes to their formation, makes them rupture once formed, or whatever.
* Medical history buffs: Dr. Charcot is famous as teacher of Freud and the other great neurologists of the era, discoverer and namer of multiple sclerosis, characterizer of Charcot-Marie-Tooth disease and the nerve-deprived Charcot joint, and the founder of "Arch. Neuro." Probably his greatest legacy is studying the emotional overlay of illness.
The distribution of "hypertensive" hemorrhages given in "Big Robbins" is worth remembering:
55%... putamen
15%... deep centrum semiovale
10%... thalamus
10%... pons (very bad location....)
10%... cerebellum
{00144} intracerebral hemorrhage
{01813} intracerebral hemorrhage
{01815} intracerebral hemorrhage
{09476} intracerebral hemorrhage
Death results from herniation or distention of the fourth ventricle by blood.
Note that, in one sense, a hemorrhage is more serious than an infarct of the same size, since there will be more edema and opportunities for herniation.
When the clot is resorbed, however, the surrounding tissue generally regains much of its function. Survivors of hemorrhages are likely to have some disability, though not nearly so much as in an infarct of the same size.
Grossly, look for surrounding edema (and maybe herniation), extravasation of blood into the subarachnoid space and/or ventricles, and a big clot on sectioning.
If present for a while, you'll see blood pigments (bilirubin, biliverdin, later hemosiderin) near the clot.
If the patient recovers, you'll see a slit ("post-apoplectic cavity") surrounded by gliosis.
|
* Actor Richard Burton, just before he died of an intracerebral hemorrhage, scribbled these lines
from Macbeth in his notebook: "The multitudinous seas incarnadine, making the
green one, red"
(i.e., Macbeth sees his victim's blood flowing so copiously as to turn the sea red)....
|
 Macbeth |
NON-TRAUMATIC SUBARACHNOID HEMORRHAGES (Lancet 369: 306, 2007)
These bleeds are fairly common, with an incidence of 25 per 100,000 people per year.
The usual cause of non-traumatic bleeding into the subarachnoid space is rupture of a "berry" ("congenital" aneurysm).
Considerably less common is bleeding from a vascular malformation; ruptured mycotic aneurysms are thankfully rare but worth remembering (Am. J. Med. Sci. 339: 190, 2010).
You are already familiar with trauma as a cause of subarachnoid hemorrhage. In addition to skull fractures, they may be caused by a blow to the head with twisting of the neck Am. J. For. Med. Path. 24: 114, 2003.
Old ideas about "gaps in the internal elastica of the arteries at the bifurcations" as direct cause are wrong; just about everybody has these gaps.
Hypertension, often cited, is a dubious risk factor. Some people claim it promotes degeneration of the elastica over time.
There's a genetic component but it's not well understood.
One known risk factor is autosomal dominant ("adult") polycystic kidney disease. Checking these patients' heads for berries: NEJM 327: 916, 1992.
Having a relative who had a berry quadruples your risk: Lancet 349: 380, 1997. It's also clear that having a first-degree sibling is a risk factor even for the uncommon "non-aneurysmal subarachnoid hemorrhage", in which the wall ruptures without a berry being found (J. Neurosurg. 115: 621, 2011).
* People with type I neurofibromatosis may have unusual berry-like aneurysms, especially farther along the course of the middle cerebral arteries.
Berries are often multiple, and tend to undergo thrombosis and even calcification. They may grow over time, berries as small as 3 mm can rupture, and if they get to 6-10 mm, rupture is common.
"Big Robbins" lists these sites favored by berry aneurysms:
40%... Anterior communicating artery, adjacent to the anterior cerebral arteries
34%... Middle cerebral artery, where it bifurcates in the Sylvian fissures (less likely to rupture: NEJM 366: 2474, 2012)
20%... Posterior communicating artery, adjacent to the middle cerebral artery
4%...Bifurcation of the basilar artery into the posterior cerebral arteries
Although tiny "berries" are common at autopsy, you'll see a big one in about 2% of routine autopsies of adults.
The thin, fibrous wall of the aneurysm is the site of rupture.
The blood may be forced directly into the brain substance and from there into the ventricles. (Free blood is noxious to brain, especially under these circumstances.)
More classically, the blood erupts into the subarachnoid space, producing excruciating pain, followed by progressive neurologic problems.
Rupture can happen at any time; ruptures during intercourse and childbirth of course get extra attention (J. Neurosurg. 114: 969, 2011).
Organization of the resulting mass of blood produces hydrocephalus by plugging the basal foraminae.
Vasospasm (which develops after a few days) can produce additional cerebral damage.
Many patients die soon after the bleed, or during re-bleeding. Others recover fully. Still others suffer persistent vegetative state.
* An unruptured berry aneurysm can cause a III-nerve palsy, and this is an important consideration when a patient presents with this finding. Surgical treatment: J. Neurosurg. 117: 904, 2013.
* When a berry aneurysm is discovered, neurosurgical consultation will be obtained, and sometimes after the clips are placed, the mass will be wrapped in cotton. Usually this incites no foreign body reaction, but occasionally a "muslinoma" will expand and cause symptoms / signs (J. Neurosurg. 112: 640, 2012).
| * In 1986, fireman-hero Paul Brophy became the first American to die following court-authorized discontinuation of nutrition and hydration. Prior to the subarachnoid hemorrhage that put him in persistent vegetative state, he very explicitly and unequivocally stated that he did not want to live under such conditions, and thought nobody else should be forced to do so, either. His family had to drag the attending physician and hospital -- and the "militants" -- all the way to the Massachusetts Supreme Court to win him (and us) the right to die under these circmstances. Some details of this case are especially grim; you may enjoy reading about it. |
 |
* Long-mysterious, the hyponatremia and excess urinary sodium loss in patients with ruptured berries now seems to be due to brain natriuretic peptide (Lancet 349: 245, 1997).
{15656} berry aneurysm, ruptured
{15667} berry aneurysm,
{17699} berry aneurysm, PICA
{17712} berry aneurysm, ruptured
{18754} berry aneurysm, ruptured
|
|
VASCULAR MALFORMATIONS may bleed into the subarachnoid space, the brain substance, or both.
ARTERIOVENOUS MALFORMATIONS (masses of large blood vessels) tend to be located in the hemispheres. Review Lancet 359: 863, 2002.
{10848} AV malformation
{10849} AV malformation
{18759} AV malformation
CAVERNOUS HEMANGIOMAS, when they occur in the brain, typically ooze small amounts of blood. They are unlikely to cause massive bleeding, but tend to cause seizures.
{15661} cavernous hemangioma
{15662} cavernous hemangioma
A large cavernous hemangioma in the meninges (as in Sturge-Weber syndrome) can steal blood away from a cerebral hemisphere.
TRAUMATIC RUPTURE OF A VERTEBRAL ARTERY occasionally causes hemorrhage. There may be an actual bursting or tearing in extreme trauma, or a medial dissection and/or a brainstem stroke in less severe trauma. Reported causes incude violence (For. Sci. Int. 182: e15, 2008), surgery, and angiography.
CAPILLARY HEMANGIOMAS do not bleed, and are incidental curiosities at autopsy.
GERMINAL PLATE HEMORRHAGES in premature babies are worth mentioning here. These are bleeds into the ventricles, rather than the subarachnoid space. The usual setting is a preemie with respiratory difficulty and cor pulmonale; the prognosis is grave if there is rupture through the ependyma into the ventricles ("intraventricular hemorrhages"; * a regrettable misnomer calls a bleed with no blood in the ventricles an "intraventricular hemorrhage grade I").
{00521} germinal plate bleed, small
{09518} germinal plate bleed, large
ATHEROSCLEROTIC ANEURYSMS in the head are typically fusiform dilatations of the basilar artery. These seldom rupture, but they may undergo thrombosis (bad!) or even damage the brainstem and its nerves by compression.
HYPERTENSIVE CEREBROVASCULAR DISEASE
In addition to its (questioned) relationship to hemorrhage, and its known relationship to atherosclerosis, hypertension causes several other cerebral problems.
LACUNAR INFARCTS ("lacunae") are little infarcts, typically a few mm across, typically in the deep structures of the brain (the basal ganglia and nearby structures are typical sites).
Classic neuropathology attributes them to hypertensive hyaline arteriolar sclerosis. However, there are often clusters of hemosiderin-laden macrophages at the periphery, suggesting that the real cause is microhemorrhages, which makes sense. Often, some of the lesions are brown-walled slits that must have resulted from hemorrhages from amyloid angiopathy (mostly in and just under the cortex) or hypertensive vasculopathy (deeper).
* Whether these are always caused by hypertension &/or amyloid &/or variants of the NOTCH3 gene &/or something else is being worked out (Brain 134: 3384, 2011). We know that hyaline arteriolar sclerosis is worst in the basal ganglia and deep white matter; if they are predominantly near the cortical surface, think of amyloid.
{09446} "êtat criblé", French for multiple lacunes
|
|
|
BINSWANGER'S SUBCORTICAL LEUKOENCEPHALOPATHY (Neurology 46: 291, 1996; Am. Fam. Phys. 58: 2068, 1998)
This describes demyelinization, gliosis, and maybe actual lacunar infarcts of the white matter of the centrum semiovale beneath the cortex ("white matter hyperintensities", "leukoaraiosis"), producing "Alzheimer-like" progressive dementia.
Along with multiple subcortical infarcts, this is one of the two common forms of "subcortical vascular dementia" / "vascular cognitive impairment."
We believe the cause of this lesion is ischemia secondary to hyaline arteriolar sclerosis of hypertension.
This is coming to be much better known than in the past, and with new imaging studies, we've found that when notable white matter changes are discovered incidentally in an older person, that person will probably have rapid, global decline in function (BMJ 339: b2477, 2009).
Since this is a subcortical process, expect rigidity, gait, and bladder problems.
In spite of what anyone else may tell you, Binswanger's is common, and is one of the great "unnoticed diseases" of the late twentieth century (common illnesses that until recently were overlooked routinely.)
It's fairly common for patients diagnosed as having "Alzheimer's disease" in life to turn out at autopsy to have Binswanger's instead. Stay tuned; the public will learn about "Binswanger's" soon.
Vascular dementia update: Med. Clin. N.A. 86: 477, 2002.
 Dr. Binswanger |
* Fun to know: Louis (Ludwig) Binswanger
It sounds corny today, but the idea that mental therapy should focus on the here-and-now, doing your own thinking (including "finding meaning" and "finding an answer for death"), accepting life even when it is not perfect, changing fixed ways of thinking, and taking responsibility for your outcomes was radical in its day (notably the 1950's). We can thank the existentialists (or maybe just common sense.) Click here for an English translation of the table of contents of Binswanger's book, and decide for yourself why the full work remains untranslated into English. Many existentialists wrote in jargon, much as did the late 20th century's "cultural studies / postmodernist / social theory" folks. Whether either is worth trying to understand is for you to decide. Whatever you think of existentialism (the dominant secular philosophy when your lecturer was growing up), I hope you will not be shy about talking with people about their personal searches for meaning, authenticity, commitment, being something real, and taking as much responsibility as they can for their own lives. |
MULTI-INFARCT / VASCULAR DEMENTIA
In the Baltimore study, atherosclerosis itself was correlated very strongly with dementia in the absence of Alzheimer's, especially in very old folks (Brain 133: 2225, 2010).
Especially if you've looked at the retinas of older folks -- and some folks in Iceland (Neurology 75: 2221, 2010) and Rotterdam (Neurology 76: 816, 2011) actually did this -- and reflect that this is probably happening in the brain as well, it's no surprise that dementia is strongly linked to the abnormal vessels in bad-looking retinas.
HYPERTENSIVE ENCEPHALOPATHY
Sudden or extreme rises in blood pressure produce brain dysfunction.
Patients complain of confusion, drowsiness, headache, and nausea. Seizures are also common.
After taking the blood pressure, clinicians look for retinal bleeds and papilledema.
We don't understand all the mechanisms involved, but at high pressures, autoregulation of blood flow breaks down, and the blood-brain barrier is compromised, with resulting cerebral edema.
In fatal cases, we find necrotic blood vessels, much like in the kidney in "malignant hypertension".

CNS TRAUMA
This is a common, grave problem that (as we have noted) causes much death and disability. There are perhaps 350,000 head injuries in the USA each year, and there are 3.3 million Americans living with disability from neurotrauma (J. Neurosurg. 112: 1125, 2010).
Damaged neurons undergo apoptosis, or their axons can be severed. The astrocyte foot processes are removed from the endothelium by trauma, with loss of the blood-brain barrier. New astrocytes migrate to the area where proteins have wandered in; they make matrix that seals the leaks ("glial scar").
Ten percent of disabling injury is brain injury.
In 1/3 of all "accidental deaths", the cause is brain injury.
In 2/3 of automobile deaths, the cause is brain injury.
| * Eye-opening article about brain trauma on the job (with suggestions as to who might do well to wear a helmet): Am. J. Pub. Health. 84: 1106, 1994. The "average" industrial worker has one chance in ten-thousand of suffering brain damage each year, but the risk varies tremendously from job to job. | 
|
* Head injuries in young athletes: Med. Clin. N.A. 78: 289, 1994. Safety stuff; required reading for any physician involved with sports. Whether stem cell treatment will help in acute neurotrauma, as it seems to do in acute myocardial infarction, remains to be seen (J. Neurosurg. 112: 1125, 2010). Beatings to the head (i.e., political prisoners) do seem to result in thinning of the cortex (Harvard torture survivor study); the study also confirmed that both past torture and past beatings do cause the amygdala to shrink (Arch. Gen. Psych. 66: 1221, 2009).
SKULL FRACTURES may be of many types (even "occult").
Bone fragments may injure the brain ("fracture contusions"), and infection may enter this way.
"Big Robbins" rightly points out that skull injury and brain injury do not necessarily go together.
An "open" ("compound") skull fracture (i.e., one with an overlying tear in the scalp will, of course, serve as a portal of entry for bacteria.
SUBARACHNOID HEMORRHAGE and SUBDURAL HEMORRHAGE are both common after severe head injuries; different authorities will cite one or the other as "more common".
EPIDURAL HEMATOMAS are accumulations of blood between the skull and the dura.
{18753} epidural hematoma
![]() Epidural hematoma
Epidural hematoma
WebPath Photo
Usually the middle meningeal artery has been severed (i.e., there has been a skull fracture crossing this vessel -- the temporal bone here is quite thin). Arterial bleeding causes these lesions to progress rapidly.
The typical story ("talk and die") is a blow to the head, with (or without) loss of consciousness, recovery, then progressive neurologic deterioration leading to coma and herniation. Once the process starts, death is almost certain unless the hematoma is evacuated (i.e., the bleeding will not stop on its own). This is a neurosurgeon's emergency, in which minutes count.
In 2009, Natasha Richardson's decisions not to wear a helmet on the ski slopes, and then not to accept care after a head injury, cost her her life.
SUBDURAL HEMATOMAS usually result from avulsion and rupture of the bridging veins that pass between the brain and the large dural sinuses.
These follow forceful displacement of the brain within the skull (i.e., inertial injury, when the skull stops but the brain continues moving); for this reason, look for them where the brain has the greatest opportunity to slide (i.e., over the cerebral convexities, often bilaterally).
Of course, the "subdural space" does not exist. Blood travels across the bottom of the dura, disrupting the loosely-connected meningothelial cells here. "Subdural bleeds" do not adhere to the brain. "Subarachnoid bleeds" do adhere to the brain.
In ACUTE SUBDURAL HEMATOMA following massive trauma, there is obvious severe injury and the prognosis is serious. Small ones after minor falls and so forth are more survivable.
SHAKEN BABY SYNDROME ("inertial brain injury"; Arch. Path. Lab. Med. 133: 619, 2009; Arch. Dis. Child. 91: 205, 2006) has had its share of dogmatists and faddists but is now being sorted out.
And the majority opinion is that most subdurals in infants under age 1 are from non-accidental trauma (Pediatrics 124: 1587, 2009).
In "shaken baby" cases, most kids are under age 2 but a few are older (Pediatrics 117: e1039, 2006. This is VERY controversial right now, with biophysicists and anatomists involved. Although I think that injury / death as a result of just shaking is uncommon, my common-sense makes me disagree with experts who believe there is always an impact. So does the NYC medical examiner, Arch. Path. 2009 above. A new series analyzing statements by perpetrators supports this: Arch. Ped. Ad. Med. 158: 454, 2004, do bear in mind that these confessions may not be truthful, as people would be less ashamed of shaking than of slamming.) Another series that suggests that shaking without impact can produce the syndrome, but that the shaking must be extreme: Pediatrics 126: 546, 2010. Shaking produces brain-damage in a three-year-old; with a credible confession Child Abuse Neglect 35: 74, 2011. A few anecdotes support this, for example the very rare but well-documented occurrence in previously-healthy people after roller-coaster rides (Am. J. Emerg. Med. 27: 517,e5-6,May 2009). I suspect that the repetitive shaking causes the brain to start oscillating relative to the skull, making the forces greater -- any biophysicists here?
By contrast, some physicians conclude that when a child has the classic retinal hemorrhages, sudural hematomas, and/or diffuse axonal injury, but no impact, it must be "shaken baby". This cannot always be true -- there is a famous video of a short fall with a head torque that produced a "shaken baby" catastrophe. The handful of credible perpetrator confessions attest to EXTREME violence in the shaking (Pediatrics 126: 546, 2010) -- and that it did make the kid stop crying.
Often the burning question in a shaken/slammed baby defense is that someone else did it and there was a lucid interval. Based on confessions and common sense, this probably does happen in a minority of cases and only with slammed-only, not shaken or shaken-slammed (Am. J. For. Med. Path. , Leeuw et al., 34: 130, 2013.)
As common sense would tell you, "shaken-baby" or the more common "shaken-impact" is a spectrum:
* Don't confuse any of these with the intradural bleeds that are commonly seen in babies dying from any cause, or the tiny subdural bleeds that are occasionally seen in babies dying of other illnesses or getting scanned. (Small subdurals result fairly often from the birth process and do not seem to be problematic. See Lancet 363: 846, 2004). This generated some pop-media confusion in early 2003. I have never taught that hemorrhages with folds near the macula are pathognomonic of child abuse, and it's now quite clear this was never true.
On the other hand, in my opinion, severe retinal bleeds in a child are much more likely to result from abusive trauma rather than an accident (J. Neurusurg. 102(S4): 380, 2005, others). The most recent credible counter-example: Ped. Neurosurg. 43: 433, 2007; of course, there has long been a large-minority opinion that retinal hemorrhages and death can result from short-distance accidental falls (Am. J. For. Med. Path. 22: 1, 2001). Or maybe unilateral retinal hemorrhages and unilateral linear skull fractures are characteristic for accidents.... (Pediatrics 118: 626, 2006). This remains extremely contentious ten years after the key paper and video -- but all parties agree that this is rare, with the vast majority being abusive. Where the "reasonable doubt" comes in is a matter for law, and I think pathologists must be humble here.
Optic nerve bleeds, retinal bleeds, and other mimics of "clearly it's inflicted trauma" from television sets falling on the heads of babies: J. For. Sci. 56: 1049, 2011.
* In 2012, the parents of Jaydan Wray, a young and foolish pair of parents who gave him severe rickets by a goofy diet, were acquitted of killing him by shaken-baby. After hearing the testimony of 60 medical experts from every point of view, the court's decision was one of the best and most cogent that I have ever read.
It's possible that the subdural hematomas of newborn babies, which tend to form a thin film on both sides of the head rather than a single mass lesion on one side as seen in older kids and adults, have a different mechanism of formation -- this is up for discussion (For. Sci. Int. 187: 6, 2009). Scan newborns and you'll discover maybe 50% have a small subdural from getting born.
Supposedly after shaking, the child is never normal and obviously needs medical care (remember there are some stupid caregivers, though -- Child Abuse & Neglect 21: 929, 1997), but may deteriorate later (J. For. Sci. 43: 723, 1998). Here's a tipoff for this very contentious area -- most non-abusers will call 911 immediately, most non-abusers will delay.
* Future pathologists: Assigning an accurate date to the hematoma will help rule a perpetrator in or our and/or establish reasonable doubt. There's some science to this. In 24-48 hours you'll see fibroblasts start to proliferate and neutrophils start to accumulate; in 48-72 hours, you'll see endothelial cells (i.e., little capillaries) start to grow in. As elsewhere, when the red cells lose their sharp borders, the bleed is probably more than 24 hours old. Especially, be alert to rebleeds -- areas that don't show the changes-over-time that others do; if a child has a subdural hematoma already, very minor trauma (or maybe no trauma at all) can cause a rebleed and the caregiver at the time gets a mistaken homicide conviction.
* NOTE: Extreme water loss can almost certainly make the brain shrink enough to tear the bridging veins in a child (Am. J. For. Med. Path. 33: 132, 2012).
{00533} acute subdural hematoma
{18758} acute subdural hematoma
{32107} acute subdural hematoma
{32110} chronic subdural hematoma
{32112} chronic subdural hematoma; despite the red, note the membrane
![]() Subdural hematoma
Subdural hematoma
Great x-ray
Pittsburgh Pathology Cases
Veins are more likely to break if the brain is a bit atrophic (alcoholism, old age) and/or there is some problem with coagulation (i.e., alcoholism).
The CT scanner has greatly improved our ability to find these lesions. (* The fictional Hans Brinker, of silver skates fame, became a neurosurgeon after seeing his father's remarkable recovery from a chronic subdural hematoma after surgery.)
* Future pathologists: Dating subdural hematomas depends on old studies from the 1930's. For example...
* As above, a SUBDURAL HYGROMA results from a tear in the arachnoid.
CONCUSSION simply means any change in mentation immediately following a blow (JAMA 266: 2867, 1991 sports). Consciousness need not be lost. The anatomic correlates are just being worked out (Neurosurg. 56: 364, 2005), and "Big Robbins"'s idea about twisting the midbrain reticular activating system sounds as good as any.
After even the slightest concussion, the brain's ability to adapt to a second blow is much-diminished; hence "second-impact syndrome". Keep the athlete out of play after even the slightest episode of wooziness. Review Clin. J. Sport. Med. 11: 194, 2001. This is a consensus nowadays. This is a very big deal in any contact sport right now.
CONTUSION (bruising) and LACERATION (tearing from being overstretched) are analogous to their counterparts in general pathology. Expect some hemorrhage with each.
All contusions result in some permanent brain damage.
COUP CONTUSIONS result from a blow to the unmoving skull that damages the underlying brain tissue without rupturing the pia. Look for cone-shaped lesions with their bases along the apices of the gyri; fresh contusions will show small hemorrhages (from capillaries) and necrosis, while old contusions show gliosis and hemosiderin pigmentation ("plaques jaunes", or "yellow plaques"); these are considered to be epileptogenic foci. Today, pathologists also look for axonal spheroids (traumatic axonal injury).
{00155} cone-shaped coup contusion. He got hit bad on the left side of the head.
{17779} old contusion
{17780} coup contusion
CONTRECOUP CONTUSIONS (contracoup contusions) result from the brain bouncing against the side of the decelerating skull opposite the point of impact (typically a floor or other large, immovable object). The pathology is similar to "coup contusions".
The bony structures of the skull itself can cause contusions in surprising places. Classic sites include the frontal lobes just above the orbital plate (from falling backwards off bar stools), and the bottom portions of the temporal lobes that overlie the petrous ridges.
The traumatic brain injury syndrome in returning veterans (chronic pain from headaches, behavioral changes, perhaps depression and a contribution to PTSD) needs no description (JAMA 300: 711, 2008). The usual cause is blast injury from improvised explosive devices.
* While "talk and die" is most typical of epidural hematomas, remember it also in frontal lobe contusions (the bruises eveutally swell and kill the patient: J. Trauma 71: 1558, 2011.
{00545} contrecoup contusion (classic site, bottom of temporal lobe)
{25618} contrecoup contusion
{25617} contrecoup contusion
TRAUMATIC INTRACEREBRAL HEMORRHAGES have been listed by "Big Robbins" as mysterious consequences of head trauma. Probably they result from tearing of the vessels themselves by mechanical forces.
TRAUMATIC AXONAL INJURY results from rupture of axons by shearing forces.
It probably accounts for residual brain damage after trauma that is not visible grossly, by classic histopathology, or on scans.
Grossly, look for petechiae in the corpus callosum, where the forces come together. Silver stains show many damaged axons with axonal spheroids (misnamed retraction balls, where axoplasmic transport has stopped).
Neuropathologists may see some reactive macrophages. Histopathology: Arch. Path. Lab. Med. 118: 168, 1994 (this crew prefers the good-old H&E stain over anything fancy; ubiqitin has been a popular immunostain though now amyloid beta precursor βAPP is preferred).
If the patient survives a long time, there may be loss of myelin, macrophage reaction, and so forth.
* Science marches onward. A standard rat model for traumatic axonal injury is now available, involving dropping a 1-pound weight 1 or 2 meters onto the animal's skull (J. Neurosurg. 80: 291 & 301, 1994).
* There is less traumatic axonal injury in "shaken baby syndrome" than one might expect, at least if we are to believe the immunostains. See Brain 124: 1299, 2001; J. Neurotrauma 20: 347, 2003. The damage is primarily "vascular axonal injury", from the massive edema stretching the axons.
* Traumatic axonal injury is the explanation give for traumatic brain injuries in returning veterans who have been injured in explosions. The boxing injury most likely to produce damage -- pushing back and twisting the head simultaneously -- probably damages the axons of the brainstem. We almost never had loss of consciousness or any injury like this in amateur boxing.
The histology of acute physical brain trauma is not very helpful in determining the exact time of injury. You can see neutrophils, swollen axons, and red neurons within an hour (and encrusted, i.e., calcified, neurons within 3.)
Patients "in coma" from trauma often are surprisingly aware of their environment and caregivers' behavior, and remember after. Be advised, and be kind. See J. Neurosurg. Nurs. 20: 223, 1988.
| NEUROPATHOLOGY OF BOXERS is seen years after blows to the head.
It begins with mild disturbances of mood and coordination.
Later, there is mild dysarthria, paranoid ideas, and/or resting tremor.
Eventually, immature and aggressive behavior, impaired memory,
hyperreflexia, and poor coordination are likely to develop.
Thankfully, only about 20% of boxers are ever affected;
risk factors include how much you've been hit,
and your apo-E type (JAMA 278: 136, 1997; Semin. Neurol. 20: 179, 2000) like in
Alzheimer's.
Where dementia has occurred, there
are neurofibrillary tangles histochemically very much like those of Alzheimer's (Am. J. Path. 136:
255, 1990; J. Neurol. Neurosurg. Psych. 53: 373, 1990).
Traditionally, it's been taught that there are no senile plaques --
reaffirmed Arch. Neuropsych. 65: , Sept 2007.
(This is being re-evaluated -- it's hard to tell whether an aging
boxer has chronic traumatic encephalopathy or just happens to have early Alzheimer's.)
Parkinsonism is common.
One classic study found the neocortical neurofibrillary tangles in boxers
to be in the superficial layers, while in Alzheimer's they were as abundant
in the deep layers (Acta. Neuropath. 85: 23, 1992).
Cavum septum pellucidum is
fairly distinctive for boxers. Boxing injuries JAMA 261: 1463, 1989.
Chronic traumatic encephalopathy in other sports -- infamously NFL football -- is under intensive studies. Some workers report that neurofibrillary tangles don't appear in the cortex at all but are abundant in the caudate, putamen, thalamus, substantia nigra and cerebellum. Watch this closely. |

|
* NOTE: Boxing has historically been poor-boy's sport in which the object is to scramble the other guy's brain enough to render him unconscious. Amateur boxing is a variant with headgear and tight regulations that keep injuries to a minimum; even minor concussions are fairly rare. It is far safer than tackle football. However, many people object to people hitting each other in the boxing ring more than they do on the football field. Whether or not physicians approve of the sport, it will continue to find participants who want to improve their fighting skills and/or who want to be respected and safe on mean streets and/or want to enjoy drug-free camaraderie with adults they can like and respect and/or who dream of big money. Some people say it's unethical for physicians to "support" the sport by caring for boxers. I respect this but do not agree.
* SHOCK THERAPY (ECT, electroconvulsive therapy) is an old psychiatric treatment that was popular for the mentally-ill in the pre-phenothiazine era. In the 1960's, office units made it extremely lucrative, and certain unethical psychiatrists made fortunes shocking every unhappy person who came to them. At the same time, leftist writer Ken Kesey misrepresented it as torture in his too-influential "One Flew Over the Cuckoo's Nest". The public believes that it dulls the mind over the long-term; though nobody has been able to show neuronal loss or other structural changes after shocking animals (Am. J. Psych. 151: 957, 1994), nobody's counted synapses or dendritic spines, either. I'll reserve judgement.
SPINAL CORD TRAUMA (review NEJM 330: 550, 1994)
This results from gunshots, stab injuries, or vertebral column injury. "Big Robbins" rightly points out that:
(1) In older people with cervical spondylosis, even small displacements of the cord can and do damage the nerves;
(2) The associated bleeding ("hematomyelia") and neutrophilic infiltrate probably exacerbate the neurologic damage.
Years after spinal cord injury, the old gliotic site of trauma will still be obvious ("myelomalacia"). Look also for ("Wallerian") degeneration of the tracts, especially the posterior columns above the injury, and the corticospinal tracts below the injury.
* The quadriplegic patient who had brain electrodes implanted and was able to move an upper extremity prosthesis well enough to do daily activities and draw pictures: Lancet 381: 557, 2013.
A perennial licensure exam item: Lots of petechiae throughout the white matter? Fat embolus!
|
|
|
|
|
INTRODUCTION
Any pathogen can probably affect the CNS. MENINGITIS is inflammation of the leptomeninges (pia and arachnoid), ENCEPHALITIS is inflammation of the brain itself, and MENINGOENCEPHALITIS is inflammation of both. CEREBRITIS is a term for a bacterial infection of the brain that has not (yet) formed an abscess.
One can have meningitis not due to infection (for example, a reaction to an intrathecally-injected
medication or the release of fluid from a tumor),
and there are autoimmune causes of
encephalitis, but the unqualified terms imply infection. "Carcinomatous meningitis" is a misnomer
for meningeal carcinomatosis, and sometimes the word "meningitis" is used to describe meningeal
infections in which there is no inflammation (i.e., many cases of
cryptococcosis![]() ).
Don't worry about it.
).
Don't worry about it.
ACUTE PYOGENIC MENINGITIS
|
|
|
|
|
|
|
|
|
|
|
|
Infection of the CSF around the brain, by classic bacteria. This was a classic infection that used to kill lots of people, including healthy young adults, and cause brain damage in many others.
Organisms reach the CNS via the nose (? "passing through the cribriform plate" is supposedly the route of entry for the meningococcus; the bloodstream seems more plausible), neural tube defects, middle-ear infections, sinus infections, surgery, etc., etc.
You will be quizzed frequently on the classically most-common etiologic agents:
E. coli... First days of life; today, a majority of nosocomial meningitis cases are gram-negatives in adults
H. 'flu... 1 month to 3-5 year old kids -- no longer chief culprit thanks to the vaccine. (Nowadays it's rare and probably the pneumococcus is most common.)
Meningococcus... Older kids and younger adults (remember epidemics, military recruits, and the subtle, dreaded hemorrhage-necrosis in the adrenal glands called Waterhouse-Friderichsen syndrome)
Pneumococcus... Oldsters and drinkers
Listeria... The third most common cause nowadays, especially in young children, older adults and/or somewhat immunocompromised folks. Review Medicine 77: 313, 1998.
It's a lawyer's disease, since contamined food is supposed to be the source.
* Increased CSF lactic acid as a marker for listeria: Heart & Lung 36: 226, 2007.
Anything... The immunosuppressed -- tough diagnosis
Note that all these organisms are (or can be) part of the "commensal flora".
Grossly, the CSF (normally crystal-clear) is turbid to frankly purulent.
In fatal cases, the pathologist can second-guess the etiologic agent by the distribution of infection. H. 'flu meningitis tends to be basal, and pneumococcal meningitis tends to be worst around the sagittal sinus.
{32838} acute pyogenic meningitis (this happens to have been E. coli)
{10857} acute pyogenic meningitis
{26174} acute pyogenic meningitis
{31992} acute pyogenic meningitis
On microscopy, neutrophils surround the leptomeningeal venules and may even pack the subarachnoid space. They will tend to follow the Virchow-Robin spaces into the brain matter itself.
Patients present with fever, malaise, and meningeal signs (i.e., headache, stiff neck, irritability, photophobia, obtundation). Dread complications are numerous, even in the antibiotic era.
Brain damage probably results mostly from occlusion of nearby blood vessels; only occasionally does the infection manage to penetrate the pia, but enough ischemia is produced to damage the nerve fibers (Neurology 62: 509, 2004).
Hydrocephalus results from fibrosis around the basal cisterns.
(Cryptococcal![]() capsular polysaccharide promotes
fibrosis.)
capsular polysaccharide promotes
fibrosis.)
Nerve damage may cause blindness, deafness, and/or other problems.
Please have a high index of suspicion for all dread, treatable illnesses, particularly bacterial meningitis. Perform a lumbar puncture whenever you think of bacterial meningitis.
Pneumococcal meningitis, perhaps because of its predilection for the elderly and drinkers, has the highest fatality rate of adult causes of meningitis.
A SUBDURAL EMPYEMA, between dura and arachnoid but sparing the latter structure itself, usually results from extension of a skull, aer or sinus infection. There is usually neck stiffness. If the pus is drained, the outcome is good. Today, imaging will show this.
SPINAL EPIDURAL INFECTIONS generally represent extensions of osteomyelitis; INTRACRANIAL EPIDURAL INFECTIONS typically spread there from sinusitis.
PACHYMENINGITIS is inflammation of the outer surface of the dura, almost always from nearby sinusitis or osteomyelitis.
The venous sinuses may become infected by draining bacterial lesions of the ears, sinuses, or face; thrombosis is a consideration.
ACUTE LYMPHOCYTIC MENINGITIS ("viral meningitis", benign "stiff neck", etc.)
Viral meningitis presents like bacterial meningitis, but usually is not so serious. Etiologic agents
include mumps![]() (thankfully rare nowadays), coxsackie
(thankfully rare nowadays), coxsackie![]() and ECHO viruses, lymphocytic
choriomeningitis (a ubiquitous, usually-trivial arenavirus caught
from house mice), and
herpes simplex II
and ECHO viruses, lymphocytic
choriomeningitis (a ubiquitous, usually-trivial arenavirus caught
from house mice), and
herpes simplex II![]() .
(Don't laugh; around 20% of people
who meet up with HSV II get an uncomfortable but mild viral meningitis with their first infection;
it may recur and prove baffling Am. J. Med. 122: 688, 2009.)
.
(Don't laugh; around 20% of people
who meet up with HSV II get an uncomfortable but mild viral meningitis with their first infection;
it may recur and prove baffling Am. J. Med. 122: 688, 2009.)
As you would expect, unless the CSF is tapped very early, there will be a predominance of lymphocytes rather than neutrophils. If the CSF pressure is very high (say, over 180 mm of water), you're probably not dealing with just viral meningitis.
Most patients recover well after several very uncomfortable days. Sequelae are rare.
* Future clinicians: Viruses and lymphocytes don't consume much CSF glucose as do bacteria and neutrophils, so CSF glucose levels will probably be normal in viral meningitis.
MOLLARET'S MENINGITIS, or "benign recurrent aseptic meningitis",
features real "ghostly" monocytes (making the diagnosis: Diag. Cytopath. 28:
227, 2003). Herpes I or (nowadays especially) II![]() is often but not always the apparent cause
(Eur. J. Clin. Micro. 23: 560, 2004). Some patients respond well
to acyclovir; others do not. Review CMAJ 174: 1710, 2006.
is often but not always the apparent cause
(Eur. J. Clin. Micro. 23: 560, 2004). Some patients respond well
to acyclovir; others do not. Review CMAJ 174: 1710, 2006.
* You'll learn how to work up "aseptic meningitis" clinically. Viral meningitis has many mimics, ranging from medication allergies (Neurology 78: 921, 2012) to juvenile rheumatoid arthritis (Heart & Lung 41: 177, 2012) to Lyme disease (Arch. Dis. Child. 97: 215, 2012; Pediatrics 129: e46, 2012).
CHRONIC MENINGITIS
"Big Robbins" has said this usually means MENINGEAL TUBERCULOSIS![]() , with granulomas, lymphocytes, and
thick caseous
, with granulomas, lymphocytes, and
thick caseous![]() debris concentrated around the basal cisterns, where cranial nerves are destroyed one by one,
hydrocephalus results from scarring, and tuberculous arteritis infarcts the underlying brain.
TB bacilli like the basal cisterns, because that's where the arteries come in and the oxygen
levels are probably highest.
Remember TB in AIDS meningitis, especially in communities with lots of TB: NEJM 326: 668,
1992. Remember that it takes weeks to grow the bug, and the bugs themselves may
even be inside the granulomas and not floating freely in the CSF.
For more on TB, click here.
debris concentrated around the basal cisterns, where cranial nerves are destroyed one by one,
hydrocephalus results from scarring, and tuberculous arteritis infarcts the underlying brain.
TB bacilli like the basal cisterns, because that's where the arteries come in and the oxygen
levels are probably highest.
Remember TB in AIDS meningitis, especially in communities with lots of TB: NEJM 326: 668,
1992. Remember that it takes weeks to grow the bug, and the bugs themselves may
even be inside the granulomas and not floating freely in the CSF.
For more on TB, click here.
|
|
CRYPTOCOCCAL MENINGITIS![]() usually affects the immunosuppressed, in whom it produces virtually no
inflammation. This is an indolent, insidious infection. Eventually, cryptococci can clog the CSF
with their mucoid goo, and distend the Virchow-Robin spaces, creating the familiar "soap bubble"
effect. (* NOTE: Dead cryptococci can persist in spinal fluid for years.)
For more on cryptococci, click here.
usually affects the immunosuppressed, in whom it produces virtually no
inflammation. This is an indolent, insidious infection. Eventually, cryptococci can clog the CSF
with their mucoid goo, and distend the Virchow-Robin spaces, creating the familiar "soap bubble"
effect. (* NOTE: Dead cryptococci can persist in spinal fluid for years.)
For more on cryptococci, click here.
|
|
|
|
|
{06050} cryptococcus, PAS stain
{06055} cryptococcus, India ink preparation
MENINGOVASCULAR SYPHILIS is an uncomfortable disease with plasmacytic vasculitis (with the familiar
"obliterative endarteritis") as in other syphilis![]() manifestations. It may turn up during secondary syphilis or later on. The headache may be intractable. Look for fibrosis of the leptomeninges around the arachnoid granulations.
Little strokes may result.
For more on syphilis, click here.
manifestations. It may turn up during secondary syphilis or later on. The headache may be intractable. Look for fibrosis of the leptomeninges around the arachnoid granulations.
Little strokes may result.
For more on syphilis, click here.
BACTERIAL INFECTIONS OF THE BRAIN
BRAIN ABSCESS may result from a dirty wound, extension (remember mastoiditis), or septic emboli (lung infections such as bronchiectasis, left-sided bacterial endocarditis, right-to-left shunts through heart or lung).
The usual etiologic agents are staph![]() ,
strep
,
strep![]() ,
or anaerobes / microaerophiles. But most any bacterium can be implicated;
nocardia
,
or anaerobes / microaerophiles. But most any bacterium can be implicated;
nocardia![]() and
actinomyces
and
actinomyces![]() both cause a disturbing number of these. Note that the CSF will be
sterile until the abscess ruptures.
both cause a disturbing number of these. Note that the CSF will be
sterile until the abscess ruptures.
Since vessels are damaged, you are likely to see some real fibrous tissue near the abscess as it develops, in addition to gliotic scar.
Brain abscesses are very bad, and patients have both systemic symptoms and focal signs. Death results from mass effect.
{00162} brain abscesses
{15544} brain abscess (three in the prefrontal lobes)
{27590} brain abscesses
|
|
MENINGOVASCULAR SYPHILIS (as above) produces headache and sometimes stroke.
GENERAL PARESIS ("paretic syphilis"; "dementia paralytica"; "luetic dementia") causes death of brain cells ("windswept cortex") and severe brain atrophy. Ask a neuropathologist to show you the "rod cells" (proliferated / wandering microglia). Patients seem to enjoy the early stages, with euphoria and mania; dementia eventually develops.
By contrast, nobody enjoys TABES DORSALIS, destruction of the sensory nerves in the dorsal roots, with ataxia, loss of pain sensation and deep tendon reflexes, and the characteristic "lightning pains". Both axons and myelin are lost in the dorsal roots (hard to see) and posterior columns (easy to see).
GUMMAS are important mass lesions, quite common in the poor nations.
Traditionally, we have taught that one diagnoses neurosyphilis by finding FTA-ABS positive spinal fluid, and that this may be positive even if the blood test has reverted to negative. (Don't forget to check.) Especially in the HIV era, people are coming in with neurosyphilis with negative CSF serologies, and physicians are now even talking about making a presumptive diagnosis on the history and physical exam (!: Mayo. Clin. Proc. 82: 1091, 2007).
* Neurosyphilis remains fairly common in the poor nations (J. Neurol. Neuros. Psych. 75: 1727, 2004).
* You usually monitor syphilis by watching the RPR go down (fourfold titer, two dilutions) in the blood; FTA-ABS may never disappear from the blood.
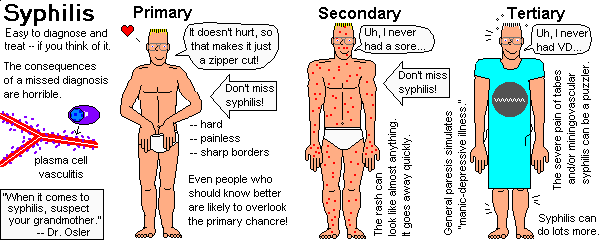
{09027} tabes dorsalis, spinal cord, myelin stain
![]() Tabes dorsalis, myelin stain
Tabes dorsalis, myelin stain
Dorsal columns at bottom
Classic drawing, Adami & McCrae, 1914
Everyone seems to know the Argyll-Robertson pupil, which accommodates but does not react (* "just like a commercial sex worker with syphilis!")
For more on syphilis![]() , click here.
, click here.
LYME DISEASE![]() can affect the brain much as does syphilis -- or it can
mimic multiple sclerosis on imaging and clinically. More often, it produces a polyneuropathy,
often involving the cranial nerves. Part of the story may be molecular mimicry -- flagellin from the
bacterium induces antibodies that cross-react with a major protein in axons (Infect. Immun. 65:
1722, 1997). As you'd expect, this is one of the few causes of plasma cells appearing in a nerve biopsy.
Use a Steiner silver stain to see the bugs.
can affect the brain much as does syphilis -- or it can
mimic multiple sclerosis on imaging and clinically. More often, it produces a polyneuropathy,
often involving the cranial nerves. Part of the story may be molecular mimicry -- flagellin from the
bacterium induces antibodies that cross-react with a major protein in axons (Infect. Immun. 65:
1722, 1997). As you'd expect, this is one of the few causes of plasma cells appearing in a nerve biopsy.
Use a Steiner silver stain to see the bugs.
TUBERCULOMAS, with caseous![]() debris in a granuloma, are still common mass lesions in the poor nations.
debris in a granuloma, are still common mass lesions in the poor nations.
![]() Lyme disease
Lyme disease![]() of the brain
of the brain
Pittsburgh Pathology Cases
CONVENTIONAL VIRUS INFECTIONS OF THE BRAIN
|
|
|
Many viruses affect the brain, and "tropism" determines which neurons or which parts of the brain they affect. The selectivity remains mysterious.
Acute viral brain infections are typically complications of systemic viral illnesses (i.e., "flu-like syndromes").
"Latent viruses" / "chronic persistent viruses" lie dormant for years (herpes 1 & 2, zoster, HIV; Epstein-Barr), while "slow viruses" (measles/SSPE, JC/PML) have a long latent period and produce a prolonged illness. Don't expect to always identify the virus from a case of fatal encephalitis, even with today's techniques.
Many but not all cases of viral (and rickettsial) brain infections feature microglial nodules, with the microglia forming clusters in which some of the cells start looking like generic macrophages again.
ARBOVIRUS ENCEPHALITIS may be due to the various "equine" (the reservoir is birds, not horses) or other encephalitis syndromes.
In the US, remember St. Louis encephalitis and West Nile; both are carried by mosquitoes, and the latter now kills at least 200 people yearly. Elsewhere in the world, Rift Valley and Japanese encephalitis are even more deadly. Review NEJM 351: 370, 2004.
In fatal cases, there is widespread perivascular inflammation (usually lymphs; polys too in eastern equine encephalitis) and widespread necrosis of the brain. West Nile (USA 1999): Lancet 354: 1221, 1999, JAMA 283: 997, 2000, Science 287: 2129, 2000, Am. J. Clin. Path. 119: 749, 2003; JAMA 290: 511, 2003.
The vast majority of West Nile infections never produce symptoms, but 20% of
immunocompetent people do develop fever, and perhaps 1% develop nervous system syndromes.
It is by far the most important epidemic encephalitis in North America;
the molecular biology of why one person gets sick and another doesn't is
just being worked out (J. Clin. Inv. 119: 3266, 2009).
West Nile is now leaving people paralyzed, as with old-style
polio![]() .
Brain damage, especially with uncontrollable anger outbursts, is also common
after clinically-apparent West Nile: JAMA 299: 2135, 2008 (sounds like Von Economo's all over again).
.
Brain damage, especially with uncontrollable anger outbursts, is also common
after clinically-apparent West Nile: JAMA 299: 2135, 2008 (sounds like Von Economo's all over again).
* Louping ill, a sheep encephalitis transmitted by ticks to humans: J. Inf. 23: 241, 1991.
ENCEPHALITIS AFTER CHILDHOOD EXANTHEMS (i.e., measles![]() ,
mumps
,
mumps![]() ,
chicken pox) is probably due in most
cases to autoimmunity. Mumps
,
chicken pox) is probably due in most
cases to autoimmunity. Mumps![]() and Epstein-Barr virus
and Epstein-Barr virus![]() occasionally really do affect the brain.
occasionally really do affect the brain.
VON ECONOMO'S ENCEPHALITIS ("encephalitis lethargica", movie "Awakenings") coincided with the vicious
influenza![]() epidemic of 1917-8. It struck with headache
and somnolence.
epidemic of 1917-8. It struck with headache
and somnolence.
The disease was (and is) variable, with extreme somnolence, agitation, dystonia, parkinsonism, stereotypy, echopraxoa-echolalia, and/or coprolalia.
Some survivors of the 'flu epidemic developed post-encephalitic Parkinsonism, with neurofibrillary tangles in the injured cells of the substantia nigra. It was not uncommon for patients to become "living statues", fully aware but unable to move.
Survivors who were able to move often exhibited hostility and aggression from the hypothalamic lesions Patients generally recognized these as unwanted and seemingly alien, and retained their intelligence and insight.
The conventional wisdom that influenza was the direct cause is challenged by the failure to demonstrate influenza virus genes in any of the archived material (Virch. Arch. 442: 591, 2003). The other large influenza pandemics of the last 100 years produced other neurologic problems but very little Parkinsonism (Parkinsonism & Rel. Dis. 16: 566, 2010). If the virus merely triggered autoimmunity, this isn't really surprising.
An illness with similar histopathology (i.e., a lymphocytic-plasmacytic inflammation of the midbrain and basal ganglia; supposedly no neurofibrillary tangles though) seems to follow other infections on an autoimmune basis (Brain 127: 21, 2004; Movement Disorders 22: 2281, 2007; Internal Medicine 46: 307, 2007; big series from London Brain 127(1): 21, 2004). The tendency is now to regard "encephalitis lethargica" as a syndrome (post-streptococcal Eur. J. Ped. Neuro. 12: 505, 2008; West Nile Am. J. Med. 115: 252, 2003).
HERPES SIMPLEX I![]() encephalitis is fairly common in children and young adults, and produces severe,
fulminant, necrotizing encephalitis, mostly of the temporal lobes.
Pathologists examine brain
biopsies for the characteristic intranuclear herpes inclusions
encephalitis is fairly common in children and young adults, and produces severe,
fulminant, necrotizing encephalitis, mostly of the temporal lobes.
Pathologists examine brain
biopsies for the characteristic intranuclear herpes inclusions![]() (check the oligodendroglia).
(check the oligodendroglia).
Nobody knows why some people suddenly get it. Susceptibility genes are known (J. Allerg. Clin. Imm. 131: 1157, 2013).
The prognosis has improved since the introduction of anti-viral therapy.
{01335} herpes; look closely, the thing really is in the nucleus (the dark structure adjacent to the
inclusion is the nucleolus)
{15473} herpes encephalitis, residual
|
|
HERPES SIMPLEX II ENCEPHALITIS![]() is why we deliver babies of mothers with HSV II by C-section.
Around 50% of babies delivered normally during the primary infection are affected, often
producing severe brain damage.
is why we deliver babies of mothers with HSV II by C-section.
Around 50% of babies delivered normally during the primary infection are affected, often
producing severe brain damage.
SIMIAN B HERPES VIRUS MYELOENCEPHALITIS is a dreaded, fulminant complication of a macaque monkey bite. Like
rabies![]() ,
it follows the nerves to the brain, and requires post-exposure prophylaxis.
,
it follows the nerves to the brain, and requires post-exposure prophylaxis.
HERPES ZOSTER ENCEPHALITIS![]() is usually a problem in the immunosuppressed, especially AIDS patients.
is usually a problem in the immunosuppressed, especially AIDS patients.
| POLIOMYELITIS is usually a mild viral summer gastroenteritis that sometimes produces a viral meningitis and/or attacks the lower motor neurons. Immunization has made the disease much less common in the developed countries, and its occurrence in recent memory among anti-immunization cultists (four among the Amish MMWR 46: 1194, 1997; Netherlands "orthodox reformed churches" Lancet 344: 665, 1994 has 68 sick, two dead; Minnesota Amish get vaccine-derived reverted polio J. Inf. Dis. 199: 391, 2009 -- nobody ended up paralyzed) or those who received weak vaccines (Lancet 335: 1192, 1990) proves it is still around. |
 Christina's World -- After Polio (?) |
|
|
There's still paralytic polio in the poor nations.
The history of polio vaccines is interesting. The original Salk vaccine was a killed strain; the oral Sabin vaccine was a live attenuated strain. The live virus has a tendency, every once in a great while, to revert to the virulent form, and this can then spread if there isn't herd immunity (huge problem J. Inf. Dis. 197: 347 & 1427, 2008; horrible outbreak in Nigeria NEJM 362: 2360, 2010; J. Inf. Dis. 203: 898, 2011; patient with common variable immunodeficiency dies NEJM 364: 2316, 2011). In the US, we have herd immunity but want our vaccines ultra-safe, so we have returned to the killed form.
* Japanese Encephalitis Virus is evidently now the major cause of an acute polio-like paralytic illness in Vietnam: Lancet 351: 1094, 1998.
* Colorado's outbreak of enterovirus D68 left a group of children with gray-matter lesions in cord and/or brainstem and muscle weakness / paralysis (Lancet 385: 1662, 2015). Similar outbreaks are happening elsewhere.
RABIES (* "lyssa", "hydrophobia"; Lancet 363: 959, 2004) results when a rhabdovirus follows the nerves up to the brain (1 mm/day or so) after the bite of a rabid animal (in the U.S. nowadays, most often a bat; remember cows, raccoons, and skunks; overseas remember monkeys and of course dogs).
Rabies was the first disease to be controlled by the methods of science (Louis Pasteur and Emile Roux prevented the disease in little Joseph Meister, who had been mauled by a rabid dog). Different animals harbor different strains. People with bat strains often do not remember a bite (Ann. Emerg. Med. 39: 528, 2002; the authors conclude that aerosol transmission is unlikely and that the bat bite went unnoticed). Hence a need to give rabies prophylaxis when a bat is found in a bedroom.
You are probably wise to be immunized against rabies if you plan to travel to a zone where it's rampant, especially India / Southeast Asia (Am. J. Trop. Med. 82: 1168, 2010).
Rabies is among the most rightly dreaded of diseases. It kills at least 60,000 people every year (J. Comm. Dis. 36: 195, 2004), and historically the disease has been incurable once the symptoms and signs appear. (In animals, the virus does not always produce disease.)
The distinctive "Negri bodies" are bullet-shaped intracytoplasmic
inclusions![]() in the neurons. The dramatic clinical syndrome includes headache, fever, irritability,
paresthesias around the wound (helps make the diagnosis), excruciating spasms on movement or the
thought of drinking ("hydrophobia"), and mania or stupor.
Foaming at the mouth results from inabiity to swallow. Finally coma and death occur.
in the neurons. The dramatic clinical syndrome includes headache, fever, irritability,
paresthesias around the wound (helps make the diagnosis), excruciating spasms on movement or the
thought of drinking ("hydrophobia"), and mania or stupor.
Foaming at the mouth results from inabiity to swallow. Finally coma and death occur.
* Rabies is most rampant in India, where stray dogs outnumber pet dogs 2:1 (J. Comm. Dis. 33: 245, 2001; strays infect both people and pets who then infect their owners), ordinary decent people do not have guns to protect themselves from rabid dogs, and the government's priorities do not include effective animal control or immunization (BMJ 331: 255 & 501, 2005). There are around 20,000 human rabies cases (all fatal; CMAJ 178: 564, 2008) in India alone every year, and 500,000 people need to be immunized; the typical Indian must pay 144 day's wages to be immunized (JAMA 1996; J. Trav. Med. 5: 30, 1998). India's "complementary and alternative practitioners" also think / pretend they can prevent rabies -- they can't (Int. J. Inf. Dis. 6: 236, 2002). The government of the "new India" is now wising up, and immunizing school children (Hum. Vacc. 4: 365, 2008).
* By contrast, in 1994, the finding of one rabid kitten in a pet store (no clue how the kitten got infected) resulted in 665 people getting post-exposure prophylaxis, which was silly, painful, and expensive (Am. J. Pub. Health 86: 1149, 1996).
Rabies transmission from an organ donor: Arch. Neuro. 62: 873, 2005; NEJM 352: 1103, 2005. Raccoon rabies, with a long latency, transmitted by organ donation: JAMA 310: 398, 2013.
* V-RG vaccine is a recombinant vaccinia virus bearing rabies antigens, which is distributed as food to wild animals. This is now widespread though low-profile, and it seems to work nicely (Vaccine 18: 3272, 2000).
* DNA-based immunization is cheap and seems to work (Nat. Med. 4: 949, 1998) but isn't available for humans yet (updates Vaccine 25: 4020, 2007; Vaccine 26: 6936, 2008; Vaccine 27: 2128, 2009). The replication-deficient rabies virus-based vaccines: J. Inf. Dis. 200: 1251, 2009.
The disease appears to remain latent within feral carnivores, and can be activated by stress (Nature 359: 277, 1992). "One of the local wolves went rabid."
* In the Peruvian Amazon region, where vampire bat attacks happen, there are people who have antibodies against rabies but who have never been immunized. They may have survived contact with a strain that is nonfatal (Am. J. Trop. Med. Hgiene 87: 206, 2012).
| {01337} Negri body |

|
CYTOMEGALOVIRUS ENCEPHALITIS![]() ("ventriculoencephalitis")
causes necrosis and (typically) dystrophic calcification of the brain in children
infected before birth.
The ependymal cells / periventricular region is selectively affected. Radiologic correlation Radiology 230: 529, 2004. The
pathology in acquired
CMV
("ventriculoencephalitis")
causes necrosis and (typically) dystrophic calcification of the brain in children
infected before birth.
The ependymal cells / periventricular region is selectively affected. Radiologic correlation Radiology 230: 529, 2004. The
pathology in acquired
CMV![]() encephalitis (as in AIDS) is similar (Neurology 55: 1910, 2000) -- you'll make the
call on PCR of the spinal fluid.
encephalitis (as in AIDS) is similar (Neurology 55: 1910, 2000) -- you'll make the
call on PCR of the spinal fluid.
|
|
AIDS ENCEPHALOPATHY ("AIDS dementia complex") affects the majority of HIV-positive victims not controlled by medication. Patients may have acute viral meningitis shortly after meeting the virus, a peripheral neuropathy, a "vacuolar myelopathy" (very common; look at the dorsal columns), and subacute encephalitis. In the latter, groups of macrophages, lymphocytes, and multinucleated giant cells (fused macrophages/microglia) cluster in the white matter, with loss of surrounding myelin.
The majority of patients with clinical AIDS become demented, at least to some degree. We do not really know everything that's going on, or all the morphologic correlates. The clinical syndromes (motor, behavioral, mixed) are still being sorted out (Neurology 69: 1789, 2007).
Young children with HIV are prone to calcification of the vessels and white matter deep in the brain. Nobody knows why.
The most troublesome brain infections in AIDS are tuberculosis, toxoplasmosis, progressive multifocal leukoencephalopathy, and cryptococcosis.
The original HAART medicines didn't get to the brain well and much HIV encephalitis remained. Thankfully, today's antiretrovirals all penetrate the nervous system quite well, and there's less HIV encephalopathy (Neurology 76: 644, 2011).
{37378} HIV giant-cell encephalitis
|
|
HTLV-I ENCEPHALOPATHY (HTLV-I encephalomyelopathy, tropical spastic paresis) is well-known, especially in the Caribbean and Brazil (Neurology 48: 13, 1997). The virus is now established as the (probably only) etiologic agent. This may be an example of molecular mimicry (Nat. Med. 8: 509, 2002; in 2006 still only one group is writing about this). Many (perhaps most) people infected with HTLV-I have some symptoms (leg weakness / hyperreflexia / bladder problems), but the clinical picture is highly variable (Neurology 61: 1588, 2003). There are likely to be many lymphocytes in affected areas.
|
|
SLOW VIRUS INFECTIONS: Long incubation period (years), long relentless disease (months or years)
SUBACURE SCLEROSING PANENCEPHALITIS ("SSPE") is caused by measles![]() virus
(acting as a slow virus; victims had previously had measles). Despite "pan-", the white matter is most severely affected. Oligodendroglia,
and to a lesser extent neurons, are destroyed, and measles (one of many cases of "Cowdry A")
inclusions
virus
(acting as a slow virus; victims had previously had measles). Despite "pan-", the white matter is most severely affected. Oligodendroglia,
and to a lesser extent neurons, are destroyed, and measles (one of many cases of "Cowdry A")
inclusions![]() are seen in the nuclei of sick cells. Dementia and motor problems occur, with death
following within a few years.
are seen in the nuclei of sick cells. Dementia and motor problems occur, with death
following within a few years.
People who have received the live vaccine and do not remember clinical measles have occasionally come down with SSPE, but the rate is less than 1/10 of that for the natural infection (about 1 in 100,000). Most likely they had measles before, or in spite of, the immunization (Epid. Inf. 131: 887, 2003). In any case, the measles virus from these people is the wild strain, not the vaccine strain (Neurology 58: 1568, 2002; Acta Paed. 93: . 1251, 2007; BMC Pediatrics 5: 47, 2007). In each case, it seems to have undergone mutations to turn it into a slow virus (Virology 291: 215, 2001
|
|
PROGRESSIVE MULTIFOCAL LEUKOENCEPHALOPATHY ("PML") is an opportunistic infection (AIDS, cancer)
by JC (John Cunningham) papovavirus (less often, SV-40). It affects oligodendroglia,
blocking production of myelin basic protein and causing apoptosis (Arch. Neuro. 59: 1930, 2002),
and produces soft, gray patches,
especially around the gray-white junction. Affected oligodendroglia nuclei contain distinctive
inclusions![]() made of virus crystals, while
nearby astrocytes (which the virus has also infected) acquire bizarre, very large nuclei
("Alzheimer's type I glia", also seen sometimes in SSPE).
made of virus crystals, while
nearby astrocytes (which the virus has also infected) acquire bizarre, very large nuclei
("Alzheimer's type I glia", also seen sometimes in SSPE).
{31956} progressive multifocal leukoencephalopathy; Alzheimer I bizarre large glial nucleus
{31957} progressive multifocal leukoencephalopathy; this shows the inclusion bodies better
{01744} PML inclusions, schematic diagram
|
|
|
|
* "Progressive rubella panencephalitis" was a rare probable re-activation of the virus in children with congenital rubella who went on to develop inflammation of the brain and die (NEJM 292: 990, 1975.) Depending on the future successes of anti-immunization militants, you may see rubella with all its grisly after-effects once again.
* It's simply a mistake nowadays to speak of the spongiform encephalopathies as "slow virus infections".
SPONGIFORM ENCEPHALOPATHIES ("unconventional agent encephalopathies"; a better name today would be "prion dementias"; some people call these "transmissible amyloidosis"; others group them with the proteinopathies as "diseases of protein misfolding"). Update Arch. Neuro. 62: 545, 2005; Lancet 363: 51, 2004.
|
|
|
![]() Prion disease
Prion disease
Lots of amyloid ("kuru plaques")
WebPath Photo
These infectious disorders are caused by agents that, to scientists before the 1990's, seemed to break the rules of basic biology. It has been clear since the 1970's that they lack nucleic acid (Nature 349: 569, 1991). They are designated PRIONS (PR for "protein", I for "infection", "-on" to finish it up.) Nobel Prize 1997, Stanley Prusiner for figuring out how they work.
The most efficient means of transmission is direct inoculation of infectious nervous system material. Unfortunately, it takes autoclaving, hypochlorite or phenol to render the material non-infectious.
By definition, prions are protein-containing infectious particles that keep their infectivity after being subjected to procedures that specifically destroy nucleic acids. A portion of the prion protein is known to be a neurotoxin (Nature 362: 543, 1993).
By the late 1990's, the mystery was solved. All known prions are altered conformational states of "prion protein" (PrP; PRNP; Science 233: 364, 1986), a normal membrane glycoprotein coded in the mammalian genome (* human chromosome 20), and well-conserved over evolution, has its gene transcribed (but does not accumulate) in health (Neurology 40: 518, 1990), and is not homologous to other known proteins. No other components have been identified to date. THE ALTERED PrP CATALYZES THE TRANSFORMATION OF NORMAL PrP MOLECULES INTO MORE PRIONS.
The infectious particles in scrapie are designated PrPSc (for scrapie; protease-resistant) and the healthy cellular form itself is PrPC (for Creutzfeldt-Jakob disease; protease-sensitive). The exact sequences change when the infections are passed from one species to another, confirming that the new particles are coded by the host genome.
PrPSc transforms PrP to PrPSc by altering its physical conformation (Nature 349: 569, 1991; how Proc. Nat. Acad. Sci. 90: 10962, 1993).
A variety of human and animal syndromes are all really variations on the same theme.
SCRAPIE causes sheep to scrape themselves against fence posts, then become demented and die. (* Don't confuse scrapie with VISNA, which is caused by a retrovirus.)
TRANSMISSIBLE MINK ENCEPHALOPATHY was transmitted to minks by feeding them dead sheep that had scrapie.
CREUTZFELDT-JAKOB DISEASE (CJ disease or JC disease; the former is preferred now because this Creutzfeldt described it first and the disease has nothing to do with JC virus) is a relatively uncommon (annual incidence 1/million in most societies), dementing disorder that usually strikes between ages 40 and 60, no sex predominance. Motor symptoms (pyramidal, extrapyramidal, myoclonic, and/or cerebellar) and behavioral aberrations may be noted. The EEG is distinctive and establishes the diagnosis. The disease is relentless and untreatable, and death results within a year or so.
Usually sporadic, the disease has also followed exposure to corneal transplants, surgical instruments (Lancet 1: 478, 1977), pituitary extract (NEJM 313: 731 & 734, 1985; Lancet 337: 1441, 1991; of the many who were exposed, those getting sick had a mutant PrP), and formalin-fixed, paraffin-embedded brain (NEJM 318: 853 & 854, 1988, well, maybe). Pathologists treat this agent with great respect.
Early diagnosis of spongiform encephalopathy can occasionally be made in humans and animals by examining the tonsils. In humans with bovine spongiform encephalopathy it is supposedly always present; otherwise the yield is low. See Nature 381: 563, 1996; update Lancet 364: 1260, 2004. Unfortunately, this doesn't work as a way of screening for other prion diseases.
* The key clinical reviews: Br. Med. J. 300: 817, 1990; South. Med. J. 83: 141, 1990 (physician's duty; the disease doesn't seem to be catching from patients); Brain 113: 121, 1990 (electron micrographs). Genes for PrP seem to correlate with susceptibility: Nature 352: 340, 1991; as do other genes modifying the course of the infection (Nat. Genet. 18: 118, 1998).
* Congo red was tried as a treatment for prion disease; it failed miserably.
* Amyloid ligands to distinguish prion disease from atypical Alzheimer's on scans: Neurology 69: 283, 2007.
Knowledge makes you vain, education makes you humble.
-- Hans G. Creutzfeldt (worth repeating)
BOVINE SPONGIFORM ENCEPHALOPATHY ("mad cow disease") was transmitted to British cattle by feeding them meal that included sheep that had died of scrapie. Thanks to an altered method of preparing the feed, prions were no longer inactivated. That there was an epidemic was obvious by 1990 (Nature 343: 193 & 196, 1990; Nature 344: 297, 1990; molecular biology J. Inf. Dis. 167: 602, 1993).
About 170,000 cattle died of the disease. The British had also been using very, very poor slaughterhouse practices, with brain mixing with the meat. The "mad cow" flap resurfaced in 1996, with the claim (Lancet April 6, 1996, most of the issue) that a new strain of Creutzfeldt-Jacob disease, with early onset, more psychiatric changes, less myoclonus, and lots of amyloid, had perhaps resulted from the abundance of prions in beef.
Later that year, Nature (383: 685, 1996) demonstrated that these patients, as well as the cows, had a prion with some different physico-chemical properties, i.e., a differently-twisted prion that autocatalyzes normal PrP true-to-form. The beef strain is now called "nvCJD" ("new variant"), or Will-Ironside Syndrome (Lancet 352: 252, 1998). The patients live longer, and the abnormal behavior is more prominent than the dementia.
In human vCJD, a mutation (methionine at codon 129) in the PNRP gene is required for susceptibility (Lancet 364: 527, 2004).
First apparent transmission of vCJD by blood transfusion: Br. Med. J. 328: 118, 2004.
* Rocky Mountain deer and elk have an epidemic prion disease. Americans are eating them. Is anybody getting sick? Maybe, but probably not (Arch. Neuro. 58: 1673, 2001.) Nobody even talks about this. Compare this indifference to the media and political excitement whenever anyone suspects a single American cow might have "mad cow" disease.
KURU affected cannibals in New Guinea, and victims appeared to be those persons who rubbed raw brains of previous victims over their own bodies. Motor problems and dementia led to death within months to years. It is Creutzfeldt-Jakob disease, transmitted in an exotic ethnic group. You will enjoy reading Am. J. Med. 26: 442, 1959 and Science 197: 943, 1977.
HEREDITARY CREUTZFELDT-JACOB DISEASE (gCJD) features any of three mutations in PrP (* E200K, D178N, or V210I). These are transmitted as dominant genes and produce proteins that have a much greater tendency to misfold. Sooner or later, the cascade starts by itself.
* CJ disease in Libyan Jews (NEJM 324: 1091, 1991) turned out to be gCJD (E200K; Medicine 76: 227, 1997). This exonerated the ethnic custom of eating raw sheep brains and eyeballs.
GERSTMANN-STRÄUSSLER DISEASE is another hereditary prion disease. These patients have a different mutation in PrP (* P102L or A117V). Transgenic mice with Gerstmann-Sträussler: Science 250: 1587, 1990; the disease has been transmitted FROM these mice, strongly confirming what we were learning about CJ disease in general: Science 251: 1023, 1991.
Transgenic mice with no PrP seem to be okay mice (Nature 356: 577, 1992, except that they get the staggers late in life: Nature 380: 528, 1996) and of course they are immune to prion disease (Proc. Nat. Acad. Sci. 90: 10608, 1993).
* A different prion-related disease, FATAL FAMILIAL INSOMNIA, as bad as it sounds, involves rapid destruction of the thalamic AV and DM nuclei without spongiform change. The disease is autosomal dominant and involves a different substituted PrP allele (178 aspartate-->asparagine) plus methionine at 192. Read all about it: NEJM 326: 444, 1992, Neurology 42: 669 & 1859, 1992, further complexities Science 258: 806, 1992; review Proc. Nat. Acad. Sci. 91: 2839, 1994; Neurology 49: 552, 1997; produces standard-brand prion disease when transmitted to mice Nautre 377: 65, 1995.
* Yet another mutation produces a dysautonomia: NEJM 369: 1904, 2013.
In spongiform change, the neuropil appears vacuolated ("spongiform changes"); the vacuoles are in the cell processes and perikaryons. At autopsy of victims of the spongiform encephalopathies, the neurons are mostly gone, but there is a corresponding tremendous astrocytosis, so brains may not appear atrophic. Pathology: Neurology 39: 1337, 1989.
"Kuru plaques", made of beta-pleated ("amyloid") PrP, affect most patients with Kuru and * GS disease and around 10% of patients with Creutzfeldt-Jakob disease. Kuru plaque formers have leucine at codon 102 of PrP.
* The differences in clinical pictures from patient to patient correlates best with which thalamic cells are most severely damaged: Brain 125: 2558, 2002.
* Prions probably have nothing to do with any diseases except for the spongiform encephalopathies (Lancet 341: 127, 1993).
If tonsillar biopsy is negative (as it usually is in non-mad-cow prion disease in humans), the diagnosis requires correlation of clinical, imaging, and brain biopsy/autopsy findings. Suggested lab tests on CSF have proved unreliable at best (Arch. Neuro 60: 813, 2003). Everybody would like a way to establish the diagnosis without having to resort to brain biopsy. Prions are likely to be present in other tissues (NEJM 349: 1812, 2003) including peripheral nerves (Arch. Neuro. 61: 747, 2004), but so far nothing is reliable.
* An antibody that clears prions, in culture and perhaps in vivo: Nature 412: 739, 2001.
* Dr. Creutzfeldt managed to save all of his neuropsych patients, and some people in concentration camps, from the Nazis.
OTHER BRAIN INFECTIONS
|
|
You are already acquainted with aspergillus![]() and
mucormycosis
and
mucormycosis![]() ,
which invade blood vessels and can
infarct the brain. Candida
,
which invade blood vessels and can
infarct the brain. Candida![]() (the most common fungal brain pathogen) and
cryptococcus
(the most common fungal brain pathogen) and
cryptococcus![]() can
produce brain infections by spreading from fungal meningitis; Candida is likely to present
microabscesses.
can
produce brain infections by spreading from fungal meningitis; Candida is likely to present
microabscesses.
ROCKY MOUNTAIN SPOTTED FEVER![]() and TYPHUS
and TYPHUS![]() affect primarily the endothelial cells; they may produce
the familiar glial nodules ("typhus nodules") in the brain. Patients are likely to have severe
headache.
affect primarily the endothelial cells; they may produce
the familiar glial nodules ("typhus nodules") in the brain. Patients are likely to have severe
headache.
ACANTHAMOEBA is an opportunist that often produces a granulomatous response. NAEGLERIA, acquired by healthy people who swim in stagnant ponds, enters the CSF via the nose, and causes necrosis of the olfactory bulbs and nearby frontal and temporal lobes ("primary amebic meningoencephalitis"). BALAMUTHIA is yet another amoeba, larger than the others (J. Neurosurg. 111: 301, 2009); the newest amoeba is Sappinia pedata (J. Inf. Dis. 1139: 2009). Update on pathology of amoebas in the brain: Mod. Path. 28: 1230, 2007.
* Expect poison from standing water. -- William Blake
{08419} acanthamoeba, trust me
{08278} naegleria, trust me
|
|
|
|
|
![]() Amoebas in the brain
Amoebas in the brain
Fluorescence
Wikimedia Commons
TOXOPLASMOSIS![]() causes brain damage similar to that seen with CMV in the fetus (including
calcifications), or a necrotizing meningoencephalitis or discrete mass in AIDS patients.
causes brain damage similar to that seen with CMV in the fetus (including
calcifications), or a necrotizing meningoencephalitis or discrete mass in AIDS patients.
|
|
|
|
{15472} toxoplasmosis of the brain in AIDS
{53733} brain damage from toxoplasmosis before birth
{32317} cat, trust me
CYSTICERCOSIS is the larval stage of the pig tapeworm ("Taenia solium") in the brain. Single worms can serve as foci for seizures, a few can obstruct the flow of CSF, or masses of larvae can fill the ventricles ("racemose form").
|
|
CEREBRAL MALARIA![]() , once attributed to immune complex deposition in blood vessels,
is now clearly caused by plugging of the vessels by infected red cells that stick to each other
and to the endothelium
(Nat. Med. 10: 143, 2004). Vessels are prone to burst, producing "ring hemorrhages".
This is obvious from the morphology anyway.
The Malawi malaria study confirms that the majority of malaria childhood deaths are cerebral
malaria (Arch. Path. Lab. Med. 135: 220, 2011).
, once attributed to immune complex deposition in blood vessels,
is now clearly caused by plugging of the vessels by infected red cells that stick to each other
and to the endothelium
(Nat. Med. 10: 143, 2004). Vessels are prone to burst, producing "ring hemorrhages".
This is obvious from the morphology anyway.
The Malawi malaria study confirms that the majority of malaria childhood deaths are cerebral
malaria (Arch. Path. Lab. Med. 135: 220, 2011).
|
|
SLEEPING SICKNESS (African trypanosomiasis) is a worsening health problem in sub-Saharan Africa (Lancet 375: 148, 2010; Neurology 66: 1094, 2006; J. Clin. Inv. 113: 496, 2004).
The histopathology is distinctive.
The familiar trypanosomes are seldom seen in the blood. The diagnosis is made on serology; if positive, patients get a lumbar puncture to see whether CNS involvement has begun. If there is elevated protein / elevated WBC / anti-trypanosomal IgM (all can be done in the field), they are treated with trivalent arsenicals, the only effective remedy for the brain disease. The arsenical treatment itself carries a mortality rate of 5%, though of course the untreated disease is always fatal.
ONCHOCERCIASIS causes blindness and epidemic epilepsy in much of sub-Saharan Africa: Lancet 372: 1721, 2008.
HEADACHE
If it's not the person's usual headache, it is meningitis,
herpes encephalitis![]() ,
or a leaking berry aneurysm until proved otherwise.
,
or a leaking berry aneurysm until proved otherwise.
Anything that puts a stretch on the scalp or the dura will make the head hurt. But pain can also be generated within the brain itself.
The most common cause of headache in the U.S. is probably CAFFEINE WITHDRAWAL (i.e., less coffee today than yesterday).
* This fact explains:
The scientific community noticed the caffeine withdrawal syndrome during the 1980's. The headache, tiredness, irritability, dysphoria, and sometimes upset stomach are common and, fortunately, mild. See Br. Med. J. 300: 1558, 1990; Am. J. Psych. 149: 33, 1992; NEJM 327: 1109, 1992; Mayo Clin. Proc. 68: 842, 1993. I hope this does not surprise you.
MIGRAINE is a centrally-generated pain syndrome, and the old story about "vasoconstriction followed by reactive vasodilatation" was silly (Neurology 42(3S2): 6, 1992), as any thinking person who's had a throbbing headache realizes.
Current work on migraine deals with "spreading depolarization" (abrupt, massive ion translocation through neuronal membranes, with cytotoxic edema), which is nonlethal to healthy tissue (why people survive migraine without brain damage) but destroys compromised cells (stroke, ischemic brain damage, second-impact?)
Different people have different migraine thresholds (Arch. Neur. 49: 914, 1992). Ordinarily, the pain and nausea are disabling, but the attacks end almost as abruptly as they began.
In exceptional cases, the vessels can, indeed, spazz shut and produce a stroke (well, maybe; if it happens, it must be very uncommon BMJ 330: 63, 2005). When migraine is a problem in middle-age, infarcts are more likely to be found on scan, but curiously these are in the cerebellum (! JAMA 301: 2563, 2009).
The disturbance in chemistry and physiology is systemic (Neurology 43(6S3): S16 & S43, 1993) and mysterious; the new crop of drugs react with the serotonin receptors (aborter drugs like sumatriptan activate 5HT1 receptors on vessels, preventive medicines activate 5HT2 receptors in the brain substance itself; these also seem to be good for "muscle spasm tension headaches"). All about treating migraine: Am. Fam. Phys. 49: 33, 1994. One remedy is lignocaine onto the sphenopalatine ganglion.
CLUSTER HEADACHES (* Horton's headache) are usually unilateral and feature tearing of the eye and dropping from the nostril on the same side. Review Lancet 366: 843, 2005.
Both migraine and cluster patients have been reported to have various abnormalities of gray matter (early work Nat. Med. 5: 836, 1999.) Whether these are the cause of the pain or the result is still speculative (Brain 132: 1419, 2009).
UNCORRECTED REFRACTIVE ERROR is another important cause of headache. Humanitarians: Note that these "trivial" conditions can ruin the quality of a person's life, though they are not part of the classic content of pathology.
"Valsalva headache" following straining at stool / exertion / coughing probably has an interesting correlate (something somewhere in the dura must be getting stretched), but so far it has eluded us. One group actually looked on MRI and found nothing (Headache 36: 251, 2005).
HANGOVER requires no description here. Ask a pharmacologist about withdrawal, fusil oils, etc., etc.
We'll leave you to finish the list of causes of headache. They include all of the processes on this
handout that involve deformation of the cranial contents. The worst headache is supposed to be
ruptured berry aneurysm. Please don't send meningitis,
herpes encephalitis![]() ,
or berry aneurysm patients home on painkillers. When in doubt, scan and/or tap.
A history may tip you off to a very small longstanding spinal fluid leak.
Despite what was recently dogma, your lecturer does not
believe that "depression" is an adequate explanation for headache. Try getting "headache" patients
off daily analgesics and coffee (South. Med. J. 86: 1202, 1993).
,
or berry aneurysm patients home on painkillers. When in doubt, scan and/or tap.
A history may tip you off to a very small longstanding spinal fluid leak.
Despite what was recently dogma, your lecturer does not
believe that "depression" is an adequate explanation for headache. Try getting "headache" patients
off daily analgesics and coffee (South. Med. J. 86: 1202, 1993).
|
|
|
|
INTRODUCTION
The "degenerative diseases of the CNS" are a family of disorders, most involving accumulations of altered forms of our own proteins, in which neurons at certain locations are selectively lost and symptoms eventually result.
They range fron simple Mendelian disorders (for example, Huntington's and many others) through disorders that are probably polygenic and variably expressed (for example, Alzheimer's and schizophrenia) to "disorders in which heredity plays no part" (for example, common parkinsonism).
| The simplest "animal model" for these diseases is a dominant gene for late-onset degeneration of a few neurons in the roundworm; the effects of this gene are modified by a host of other genes (Nature 345: 410, 1990). |
 |
Watch for these to be renamed "the proteinopathies" soon.
DEMENTIA: Sustained permanent decrease in several dimensions of intellectual function, so as to interfere in normal social or economic activity.
When there is cognitive decline in old age, the brain will typically show neurofibrillary tangles and/or micro-infarcts and/or Lewy bodies in the cortex. When the decline is rapid / catastrophic, a classic dementing disease pathology will be found (Neurology 75: 1070, 2010 -- the Roman Catholic Religious Orders study, which followed older nuns, priests, and brothers over years and performed brain autopsies.)
AMENTIA: Mental retardation (misnomer)
OBTUNDED: Less responsive than normal, especially to pain
DELIRIUM: Reversible impairment of mental functioning, typically with some degree of disorientation, usually without permanent abnormalities, usually with some agitation. Whether brain damage is likely to result after an episode of delirium is under discussion; it's hard to study.
* ABIOTROPHY: Neurons "just decide to die". This word is passing out of use as we discover the real causes of these diseases. "Jargon is not insight."
The differential diagnosis of dementia in the older patient is a long one. Think of:
Poisoning
Pfiesteria piscicida, the dinoflagellate from Chesapeake Bay, and the coasts of Virginia and North Carolina, due to contamination by pig runoff, is another neurotoxin to watch. J. Tox. Env. Health 46: 501, 1997; Lancet 352 532, 1998. Anecdotal reports from fisherfolk and from two technicians at Duke who still complain of memory problems are alarming. It's now called "estuary syndrome". The toxin, long-unidentified and doubted, now is reported as a curious metal complex (Env. Sci. Tech. 41: 1166, 2007.) This is now a robust finding.
Certain cancer chemotherapeutic protocols produce
serious brain damage (for only one example, which suggests how badly
this problem has been overlooked, see Neurology 59: 48, 2002;
more Neurology 62: 548, 2004).
I would have added an anti-nuclear antibody, an anti-Ro, a serum magnesium (!),
and a Lyme![]() serology, plus lead and
mercury screens for those that might have been exposed.
Anti-microsomal antibody for anybody with a goiter (Hashimoto's encephalopathy
does not always feature hypothyroidism.)
serology, plus lead and
mercury screens for those that might have been exposed.
Anti-microsomal antibody for anybody with a goiter (Hashimoto's encephalopathy
does not always feature hypothyroidism.)
Of course, down the road (especially if Alzheimer's become treatable) we may have a host of assays on spinal fluid
(Alzheimer's proteins Arch. Neuro. 66: 382, 2009) and/or be making
extensive use of PET scans with specific markers to light up specific proteinopathies.
Stay tuned.
Brain biopsy for slow dementia: One center's experience: Arch. Neurol. 49: 28, 1992. Another's: Brain 128: 2016, 2005 (just over half are diagnostic; out of 90, one curable disease -- Whipple's -- was found). Still not a routine procedure! Brain biopsy for more rapid dementia seems much more worthwhile, with lymphomas and prion disease found most often (J. Neurosurg. 106: 72, 2007); still, it usually does not give information that guides effective treatment (Neurology 75: 419, 2010). No one questions that brain biopsy in known HIV infection or suspected non-lymphomatous tumor can often be essential.
* UCLA autopsy series for causes of dementia: Arch. Path. Lab. Med. 128: 32, 2004. Alzheimer's is most common, with vascular dementias second, and Lewy body dementia (6%), normal-pressure hydrocephalus, PSP, and Pick's (and variants; 4%) all common as well.
ALZHEIMER'S DISEASE ("pre-senile dementia", "senile dementia", "old timer's disease", "brain failure", etc.; "a primer for practicing pathologists": Arch. Path. Lab. Med. 117: 132, 1993; for general physicians Lancet 377: 1019, 2011)
|
|
|
This very common dementing disease affects several million Americans. It becomes more common with advancing age, and will be an even more serious a problem as the numbers of elderly increase.
If you control for how old people are, Alzheimer's is about equally common everywhere in the world.
The disease seldom begins under age 50, except in Down's syndrome people, who all get it in their thirties or thereabouts (N.Y. State Med. J. 90: 64, 1990). Estimates of its frequency vary widely, but around 5% of people over 65 are affected, and 20% of people over 80 are affected. There is no sex predominance.
The familial forms of Alzheimer's, which account for around 5-20% of cases, are mostly autosomal dominant. There are now several different loci known. See below.
We no longer distinguish between "pre-senile dementia" (Alzheimer's before age 65) and "senile dementia" (Alzheimer's after 65; formerly only "pre-senile dementia" was dignified with the Alzheimer's label, though the pathology and symptomatology are identical.)
Almost all very-old folks have some Alzheimer's type changes in the brain, but these correlate with dementia much more strongly at age 75 than at age 95 (NEJM 360: 2302, 2009). No one understands why.
More evidence that the "plaques and tangles" aren't central to the dementia: Folks with lots of "Alzheimer's pathology" at autopsy but whose brain weights and hippocampal volumes were still fairly large showed little or no dementia (Neurology 72: 354, 2009).
You will learn plenty about Alzheimer's disease during your medical education. Here, we'll focus on the pathology.
The gross pathology is that of diffuse cortical atrophy, with widening of the sulci, narrowing of the gyri, and hydrocephalus ex vacuo.
Once Alzheimer's disease declares itself, the worst-affected areas of cortex can shrink by around 15% per year (!! Lancet 343: 829, 1994).
{34478} brain atrophy
The microscopic pathology shows several distinctive features:
NEUROFIBRILLARY TANGLES are beta-pleated from over-phosphorylated tau protein, in the form of twisted paired helices ("curly fibers"), within neurons. They stain best with silver (*Bielschowsky).
{26762} neurofibrillary tangles
A major component of these tangles tau protein, a microtubule element (Proc. Nat. Acad. Sci. 88: 8910, 1991; Am. J. Path. 140: 277, 1992). Ubiquitin is added as they grow; you may also find some Aβ (see below).
Neurofibrillary tangles in the cortex-only strongly suggest Alzheimer's. You can see them elsewhere in post-encephalitic parkinsonism, progressive supranuclear palsy, chronic traumatic encephalopathy, corticobasal degeneration, ALS-dementia complex of Guam, and a few others.
* Counting neurofibrillary tangles in various areas gives the "Braak stage" for Alzheimer's, which its developers in the late 1980's felt was the best correlate with dementia (i.e., tangles are more important than plaques). This has some support (Neurology 62: 428, 2004).
SENILE PLAQUES ("neuritic plaques") are focal abnormalities in the cortex (check the hippocampus), 20-150 microns across, consisting of abnormal, tau-protein laden nerve processes, microglial cells, and turned-on astrocytes, in the later stages surrounding an amyloid core made of Aβ and apo-E (future pathologists read Am. J. Path. 137: 1383, 1990). Unless there is an amyloid core, the fibers are not disrupted or disorganized. The neuritic processes contain tau isoforms like those in neurofibrillary tangles.
* A few patients with dementia seem to have plaque-only disease -- a piece of the puzzle is missing. See J. Neuropath. 71: 266, 2012.
* The amyloid cores were originally described as containing some aluminum silicate. I have taught for 35 years that the aluminum silicate in the old studies got there as a result of binding during the tissue processing. I believe I was right. Aluminum caused neurotoxicity in "dialysis dementia" decades ago, but the neuropathology is completely different (Neuropathology 22: 206, 2002), and heavily-aluminum-exposured, relatively young brains do not exhibit more Alzheimer changes (proliferation of astrocytes and microglia in the cortex, basal ganglia, and thalamus; no NFT's or plaques -- Acta Neuropath. 101: 211, 2001). Further, a host of studies (summary CMAJ 162: 65, 2000) show that the brains, the tangles, and the plaques do not contain excess aluminum after all. Despite decades of trying, no "environmentalists" have been able to show an obvious risk from drinking water or dietary aluminum concentrations. Results of studies on aluminum concentration in drinking water and Alzheimer rates are mixed, and in any case drinking water contributes only a small amount of total aluminum in the diet (Brain Res. Bull. 55: 187, 2001). And having worked in an aluminum factory clearly does NOT put you at greater risk (Br. J. Psych. 168: 244, 1996). The other 1990's hoopla, about silicate in the drinking water causing Alzheimer's, crashed and burned when a retrospective French study found that the more silica in the drinking water, the less Alzheimer's (Am. J. Clin. Nutr. 81: 897, 2005).
{01339} senile plaques
{01341} senile plaques, silver stain
{01342} senile plaques, immunoperoxidase stain for amyloid
|
|
![]() Alzheimer's
Alzheimer's
Senile plaques
Wikimedia Commons
Lots of older people have a few plaques in the hippocampus. More than a very few plaques in the neocortex means Alzheimer's (Arch. Neuro. 50: 349, 1993).
Of course, dendrites and their complex patterns are also greatly diminished in Alzheimer's: Am. J. Path. 163: 1615, 2003.
ALZHEIMER'S AMYLOID ANGIOPATHY ("congophilic angiopathy") is usually present in the gray matter arteries by the time the patient is symptomatic. The fragile, amyloid-laden vessels seldom hemorrhage; the amyloid is made of Aβ (Proc. Nat. Acad. Sci. 90: 10836, 1993).
GRANULOVACUOLAR DEGENERATION (silver-positive granules surrounded by clear zones, within neurons; the granules were identified as tau by my old teacher, William Bondareff: Am. J. Path. 139: 641, 1991) and HIRANO BODIES are often seen and are of obscure significance.
WARNING: Many (if not most) older patients have similar changes, though to a lesser degree, without being demented, i.e., plaques and tangles in the hippocampus probably help explain a lot of the forgetfulness of some old people. We know that complaints of impaired memory tend to be proportionate to the extent of Alzheimer-like pathology at autopsy (Neurology 67: 1581, 2006). However, many forgetful older folks, even those with the "mild cognitive impairment" that is thought to precede Alzheimer's in many cases, have no senile/neuritic plaques and hence "cannot be considered to have early Alzheimer's disease" (Arch. Neuro. 63: 1771, 2006).
Alzheimer's disease presents a progressive, unremitting dementia. The first deficits are in mood, judgement, and recent memory. There may be motor problems. The end is always profound disability and death. Insight is lost very early; a patient who says, "I think I have Alzheimer's disease" is probably depressed instead.
Alzheimer's remains a diagnosis based on history and clinical examination, with imaging to rule out other entities.
* A claim that these people's pupils are more sensitive to anticholinergic pupillary dilatation was the basis for a mid-1990's test-claim for the disease. It just wasn't true (Mayo Clin. Proc. 72: 495, 1997).
* A proposal for early diagnosis of Alzheimer's based in finding tau in the easily-biopsied olfactory epithelium flopped: Nature 369: 365, 1994. Over the past few years, various cerebrospinal fluid markers for Alzheimer's (total tau, phosphorylated tau, and A-beta-42 -- the latter the amyloidogenic peptide) have been tested; these are less likely to become standard-of-care than amyloid / MRI imaging and the history / clinical exam (Med. Clin. N.A. 97: 369, 2013; Neurology 80: 132, 2013).
* Adults who seem to function normally but who have the genes for early-onset Alzheimer's have distinctively smaller hippocampi (Neurology 78: 1769, 2012).
* The one blood analyte that presently shows promise is serum clusterin (Arch. Gen. Psych. 67: 739, 2010).
They are still research tools, but in the cerebrospinal fluid, elevated p-tau 181 predicts Alzheimer's with lots of neurofibrilllary tangles / hyperphosphorylated tau, and LOW Abeta42 levels predict lots of senile plaques (Neurology 78: 1568, 2012).
Diffusion tensor MRI (a variant on the familiar imaging technique) seems also to show changes distinctive for Alzheimer's, in contrast with Lewy body dementia and other entities that resemble it clinically (Neurology 74: 1814, 2010).
* The "pop" claim that getting highly educated / "exercising your brain" prevents or slows Alzheimer's seems to have been disproved by the pathologists at U. Wash (Neurology 70: 1732, 2008); probaby folks who have a lot of practice with mental games simply do better on tests of cognition despite their Alzheimer's pathology.
* UMKC's past chief of pathology, Dr. Parker, was "Mr. Alzheimer's disease" for the Kansas City area. We provided post-mortem neuropathology at no charge to families. A significant number of ante-mortem Alzheimer diagnoses are wrong: Am. J. Psych. 147: 168, 1990; our figures from outside TMC were even more discouraging.
Most of the work in Alzheimer's is of course focused on the amyloid in the cores of senile plaques and the vessels ("amyloid beta" or "amyloid A4", or nowadays, "Aβ" or "AbetaP"), and the precursor protein of this amyloid.
The Aβ amyloid is beta-pleated from a fragment of a much larger protein (APP, amyloid precursor protein), coded on chromosome 21 ("just like Down's syndrome"). We don't know what it's for, but it's an integral membrane protein of healthy brain; it binds to GTP-binders (Nature 362: 75, 1993), etc. Similar proteins occur all over the brain and the body (Nature 344: 497, 1990; Science 248: 1126, 1990, lots more).
In the brain, the healthy way of processing these proteins involves breaking them down using a still-not-fully-understood protease called "alpha-secretase" or "the non-alzheimer's secretase", at positions 15-17, in the middle of the Aβ sequence, so none of the amyloidogenic peptide forms ("the good secretase pathway").
If the precursor is broken down instead by a different enzyme, "beta-secretase" or "the Alzheimer's secretase" (now "BACE"), an amyloidogenic peptide is produced and, since the body does not metabolize amyloid well, begins to cause damage. Enzyme isolated and characterized Science 286: 735, 1999; J. Biol. Chem. 275: 21099, 2001; knockout mouse Nature Neuroscience 4: 231, 2001.
* Valsartan, an angiotensin-II receptor antagonist that is also an inhibitor of Abeta amyloidogenesis, seems to work in a mouse model: J. Clin. Inv. 117: 3393, 2007.
* A newer player is neprilysin, which breaks down amyloids and is downregulated in the elderly and in late-onset Alzheimer's (Am. J. Path. 171: 241, 2007; Am. J. Path. 172: 1342, 2008).
Immunotherapy against the Aβ42 fragment of the peptide has been shown to protect and even clear plaques from the mouse model (Proc. Nat. Acad. Sci. 98: 8850 & 8931, 2001; Nature Medicine 7: 369, 2001; Nat. Med. 6: 916, 2000). This has received tremendous attention and was the basis of the push for the "Alzheimer vaccine".
In July 2008, the next study was published (Lancet 372: 216, 2008). The vaccine cleared plaques, but the clinical benefit is small (ultrastructural changes induced by the vaccine: Brain 133: 1297, 2010). In fact, some of the most-demented patients were nearly plaque-free. DARN!!
* Bapineuzumab, an anti-amyloid-beta monoclonal antibody, was not a striking success either (Neurology 73: 2061, 2009).
The failure of the Alzheimer vaccine matched work that had been going on for several years, especially from Harvard (Nat. Med. 14: 837, 2008) -- on the evidence, AMYLOID-BETA DIMERS (Abeta dimers) directly damage structure and function at synapses themselves.
* The new agent Pittsburgh Compound B (C11-PIB or [(11)C] PiB) is now being used to light up and diagnose Alzheimer's lesions on PET scan. Update Neurology 72: 1504, 2009; Brain 133: 3336, 2010; Arch. Neuro. 68: 232, 2011.
The known Alzheimer's genes
The presenilins (PS1, PS2) somehow modify the activities of one or more of the secretases, though the big picture is still far from clear (Nat. Med. 2: 864, 1996 was the key article); perhaps the mutant forms also fail to clear amyloidogenic Aβ: Nat. Med. 3: 67, 1997; Nat Med 5; 164, 1999. Newer work shows they're calcium channels (J. Clin. Inv. 117: 1230, 2007) and the mutations that matter disrupt this activity.
Clusterin, the "new" Alzheimer's-related protein, is a chaperonin that clears cell debris.
* Elevated homocysteine levels as a risk factor for Alzheimer's: NEJM 346: 476, 2002. Perhaps it is a marker for something that does damage to the white matter, accentuating the Alzheimer's (Arch. Neuro. 59: 787, 2002; if the relationship is real, it's elusive Neurology 65: 1402, 2005).
* Alpha-2 macroglobulin (the pentamer that perhaps cleaves Aβ) if partially deleted has been reported linked to sporadic Alzheimer's. Lancet 352: 293, 1998; less certain Neurology 55: 443 & 678, 2000; more Neurology 59: 756, 2002.
Since microglia
seem to be important components of senile plaques (Acta Neuropath. 77: 569, 1989, i.e., they are
inflamed, perhaps because Aβ activates C1q J. Imm. 152: 5050, 1994 and microglia too
of course Nature 374: 647, 1995), there is presently some empirical interest in anti-inflammatory
drugs to prevent Alzheimer's, and this is supported by its low incidence in rheumatoid arthritis
(aspirin) and lepers![]() (dapsone).
Despite some earlier optimism,
Johns Hopkins undertook a prospective study and so far, naproxin and celecoxib
haven't prevented Alzheimer's (Neurology 68: 1800, 2007; also Neurology 70:
2219, 2008). They also do
not slow the established disease (Arch. Neuro. 65: 896, 2008) and
survivors of the studies are coming in with more neurotic plaques than
controls (Neurology 75: 1203, 2010).
(dapsone).
Despite some earlier optimism,
Johns Hopkins undertook a prospective study and so far, naproxin and celecoxib
haven't prevented Alzheimer's (Neurology 68: 1800, 2007; also Neurology 70:
2219, 2008). They also do
not slow the established disease (Arch. Neuro. 65: 896, 2008) and
survivors of the studies are coming in with more neurotic plaques than
controls (Neurology 75: 1203, 2010).
* Nobody knows why Alzheimer's patients tend to become acutely delirious as the sun sets ("sundowners"): Neurology 42: 83, 1992.
* In 1995, I predicted the 1997 media flap about smoking preventing Alzheimer's. It doesn't.
* We are now observing that people who have been on statin therapy for hypercholesterolemia in midlife seem to have a much lower rate of Alzheimer's. No one knows why. See Am. J. Med. 118 (S-12A): 48, 2005.
* Everybody wishes we had more for treating Alzheimer's. Update on the cholinergic enhancer drug donepezil: Neurology 69: 459, 2007. Obviouly this can't replace neurons once they're gone. Today's anti-Alzheimer drugs really don't work very well at all: Ann. Int. Med. 148: 379, 2008; in 2008, the FDA advised that the evidence of effectiveness was so lacking that the drugs shouldn't be used routinely (JAMA 299: 1763, 2008). Dimebon, an old Russian antihistamine, found serendipitously to help Alzheimer's (Lancet 372: 207, 2008 -- watch this one). A heroic study in which older folks were randomized to forced exercise over two years versus just sitting showed that fitness training has no effect on progression of dementia (JAMA 314: 781, 2015). Some "totally gone" Alzheimer's patients seem to enjoy headphones playing the music that was popular when they were teens. These may be the people whose right temporal cortex is relatively spared (Brain 134: 2523, 2011). I respectfully request that, under these circumstances, I receive a general anesthetic and organ-harvest instead, but that is probably not going to be legal any time soon.
* An Alzheimer's variant with similar chemical markers (Neurology 76: 1782, 2011) and histopathology, but involving the posterior brain is now distinguished as POSTERIOR CORTICAL ATROPHY. Vision, reading, language, and arithmetic skills are more affected than memory.
* HIPPOCAMPAL SCLEROSIS OF OLD AGE features loss of neurons and their replacement by gliosis; it appears in the old-old and rapidly increases after age 85. It can be distinguished from other causes of hippocampal atrophy only on autopsy. Update Brain 134: 1506, 2011.
FRONTOTEMPORAL DEMENTIAS ("lobar atrophy", "FTLD", formerly all lumped as "Pick's disease" and now sub-sub-classified Arch. Neuropath. 114: 5, 2007) is a pattern of cortical dementia, less common than Alzheimer's. Update of the frontotemporal lobe dementias for clinicians: Med. Clin. N.A. 86: 501, 2002; pathologists Brain 128: 1996, 2005 and Arch. Path. Lab. Med. 130: 1063, 2006 and (autopsy pathologists) Arch. Path. Lab. Med. 137: 314, 2013.
The gross pathology is distinctive, with selective, extreme ("walnut", "knife blade") atrophy of the prefrontal cortex and anterior 2/3 of the superior temporal gyrus.
Microscopically, we look for balloon-swollen "Pick cells", and silver-positive intra-neuronal "Pick bodies" (made from tau; they define "true Pick's"). There is widespread neuronal loss, with virtually none remaining in "walnut" areas.
The molecular biology is just starting to become clear. Not surprisingly, the problem in "true Pick's" is with the processing of tau microtubules (Ann. Neuro. 51: 730, 2002).
Frontotemporal dementia patients have a course similar to Alzheimer's disease. The presentation is variable. The social graces are likely to be lost earlier, as are semantic skills, while memory may be better preserved.
* Some clinicians distinguish, and correlate with areas of volume loss scans, "behavioral variant" (bvFTD -- mesial frontal lobe -- clinical-pathologic correlates Neurology 80: 561, 2013), "semantic dementia" (talks fine but can't remember the names of things and eventually the meanings of words, SEMD -- rostral temporal lobe), and "progressive nonfluent aphasia" (understands words but can't say them, PNFA -- left insula). There is less correlation with the presence of the pathologic lesions or their types (Neurology 72: 1653, 2009), which is no surprise, since the problem is loss of the brain cells themselves rather than the presence of inclusion bodies and so forth.
TRUE PICK'S DISEASE is now restricted to cases with the classic tau-based Pick bodies. (I can't recommend doing a biopsy to distinguish among similar, untreatable diseases.)
FTLD-TDP (formerly "frontotemporal dementia with ubiquitin-only" / FTLD-U, renamed as I predicted, now the most common of the frontotemporal dementias (Arch. Neuro. 65: 1481, 2008; Brain 130: 1148, 2007). FTLD-U photos Am. J. Path. 169: 1343, 2006. It is now clear that the "ubiquitin-only" bodies are composed largely of TDP-43 (Science 314: 130, 2006; Am. J. Path. 173: 182, 2008). This links it to common and most familial amyotrophic lateral sclerosis, and there's now talk of these being a continuum ("multisystem TDP-43 proteinopathies" -- Arch. Neuro. 66: 180, 2009) and of the FTLD-U, TDP-43 positive patients having subtypes with different pathologies correlating with different clinical syndromes (Arch. Neuro. 64: 1449, 2007). This is now a robust finding with variations on imaging: Neurology 75: 2204, 2010.
* PRIMARY PROGRESSIVE APHASIA is still described as a Pick variant (last big review Neurology 44: 2065, 1994) sometimes with more atrophy on the left and with speech going long before anything else. There are balloon cells, but no Pick bodies; there are often ubiquitin-positive inclusion bodies that remain to be characterized. Just as in FTLD-U, a few percent of patients have progranulin mutations (Arch. Neuro. 64: 43, 2007; Brain 131: 732, 2008). Exacty where this disease fits is up for grabs right now (Neurology 72: 1562 & 1653, 2009). Probably most cases were what we now call the progressive nonfluent aphasia variant, but some Alzheimer's patients present with language problems before anything else and this may become the name of a syndrome, the precise diagnosis waiting for autopsy.
We can distinguish Alzheimer's presenting as similar speech problems from "primary progressive aphasia" by scan (Neurology 70: 25, 2008 -- the neuropathology itself remains a puzzler Brain 135: 1554, 2012). More recently, the four entities likely to present primarily as speech problems -- Alzheimer's, argyrophilic grain disease, TDP-43 frontotemporal dementia, and tau frontotemporal dementia -- are being distinguished by scans (Neurology 74: 42, 2010).
* Yet another variant features a combination of frontotemporal lobe dementia and motor neuron disease, complete with Bunina bodies (Arch. Neuro. 63: 506, 2006).
* We have gone from thinking of the frontotemporal dementias as mostly sporadic to thinking of them as genetic; some are single-gene, some are polygenic. A tau/MAPT mutation causes familial Pick's with tau inclusions as you'd expect: Brain 127: 1415, 2004. Mutations of the gene GRN ("progranulin") produces FTLD-U (mutations and pathology Brain 129: 3081 & 3091, 2006) -- evidently detectable by a blood assay (Brain 132: 583, 2009). A genetic syndrome (VCP / p97) causes frontotemporal dementia, Paget's of the bone, and inclusion body myositis (Brain 130: 381, 2007). We'll see the genetics of FTDP-17 (Pick's-and-Parkinson's) below. A current line-up of today's five "usual suspects" for polygenic disease: Neurology 73: 1451, 2009).
Two other Pick variants are BASOPHILIC INCLUSION BODY DISEASE and NEURONAL INTERMEDIATE FILAMENT INCLUSION DISEASE / NEUROFILAMENT INCLUSION BODY DISEASE (Acta Neuropath. 114: 5, 2007)
|
HUNTINGTON'S DISEASE ("Woody Guthrie's disease")
This is an autosomal dominant disease (gene Htt, protein huntingtin, * chromosome 4, gene cloned Cell 72: 971, 1993, Nature 362: 408, 1993) with complete penetrance. Neurons disappear, most spectacularly in the head of the caudate nucleus.
* There is also plenty of cell loss in the cortex, and its extent in the motor and cingulate cortex areas correlates with symptoms Brain 133: 1094, 2010. Between age 20 and age 50, mental function diminishes (* "subcortical dementia"), behavior, insight, and mood change for the worse (one group coins the phrase "beyond disgust" for the inability to recognize negative emotions and the things that should provoke them: Brain 130: 1715, 2007; more on the altered emotions that precede the movement disorder Brain 135: 1165, 2012). Then a movement disorder (chorea and athetosis, resembling a jerky dance) develops. Profound disability and death occur after 10-20 years. |
 Woody Guthrie |
The gene (for "huntingtin") is a "Sherman's paradox" gene, confirming the clinicians' impression that Huntington's appears earlier from generation to generation. The mutation involves expansion of CAG sequences. The proteins that are produced have poly-glutamine sequences, which un-solubilize the protein, causing it to accumulate and gum up the nucleus (Cell 90: 537, 1997; Nat. Genet. 18: 150, 1998). All about Huntington's genes around the world: NEJM 330: 1401, 1994. The age of onset of the motor symptoms is entirely a function of the number of repeats (Neurology 78: 690, 2012).
At autopsy, there is moderate atrophy of the whole brain, and striking atrophy of the head of the caudate nucleus (* to a lesser extent, the putamen and globus pallidus); there is generally considerable atrophy of the frontal cortex and locus ceruleus as well.
* In a series of 523 banked Huntington brains, the one surprise is that some Huntington's brains have more severe changes in the striatum, and others in the cortex. The two groups are distinct. Some unknown factor not involving the Huntington's gene is modifying the disease (Neurology 79: 1708, 2012).
Of course, it's possible to predict who will get the disease. This is sensitive ethically and emotionally.
* Venezuela has a tremendous amount of Huntington's, centered on a single region; see Lancet 364: 569, 2004. All victims are descended from a single man. If someone has a parent with the disease, he/she tries to have as many children as possible in order for there to be a caregiver if he/she becomes disabled. Since genetic testing and prenatal screening are not options for Venezuelans because of the politics, the situation can only get worse.
* Some countries (and not just the Third Reich) have tried to control Huntington's by government policies. Review of this: Am. J. Hum. Genet. 50: 460, 1992. Some well-intentioned people believe that encouraging people to make their reproductive decisions with a thought to the good of society is fundamentally and profoundly immoral, and that this fact is not open to debate (Clin. Genet. 64: 327, 2003). A discussion (JAMA 290: 1219, 2003) of the "ethical dilemmas" posed by Huntington's testing ("No! No! Don't tell my children they and the children they're going to have may be at risk too!") showcased (at least for me) a lack of common sense and regard for the lives of others. ("Paternalism! Bad!") More recent discussions of the release of confidential genetic information have focused instead on the family's autonomy ("Autonomy! Good!"). Stay tuned, especially in these changing economic times.
* An inhibitor of the transglutiminase that cross-links huntingtin is the first medication to slow down Huntington's disease, at least in mice (Nat. Med. 8: 143, 2002). Trehalose and/or Congo red (!): Nat. Med. 10: 123, 2004. Nothing for humans yet, sorry.
* Fun to know: Huntington described the disease as a med student; he was from a long line of doctors on Long Island who'd observed the disease in a long line of neighbors over several lifetimes.
{32870} Huntington's brain, gross; not much caudate
 Huntington's
Huntington's
Pittsburgh Pathology Cases
PARKINSON'S DISEASE ("paralysis agitans") and its relatives: Parkinsonism review: NEJM 339: 1130, 1998; Lancet 363: 1783, 2004; J. Clin. Inv. 116: 1744, 2006; Lancet 373: 2055, 2009; Nat. Med. 16: 653, 2010
|
|
This is a family of disorders involving destruction of the dopaminergic neurons of the substantia nigra (i.e., the fibers that talk to the striatum) and locus ceruleus (* and the dorsal motor nucleus of X: Neurology 42: 2106, 1992; the raphe, and some others).
Grossly, you'll see "depigmentation of the substantia nigra", no matter what the cause.
{17754} Parkinson's vs. normal (midbrain sections)
The result of the neuronal loss is a movement disorder, with "pill-rolling" resting tremor, festinating gait, bradykinesia, cogwheel rigidity, and mask-like face. Many patients become demented (the pathology correlate seems to be beta-amyloid in the striatum J. Neuropath 67: 155, 2008; no correlation with co-existing Alzheimer's, but the atrophy of the hippocampus looks muich the same grossly Brain 135: 170, 2012). Parkinson's patients who have freezing of gait have gray matter atrophy in the frontal and parietal areas (Neurology 78: 409, 2012). Please remember how to distinguish dementia from the depression that is so often seen in Parkinsonism.
Known causes include Von Economo's encephalitis ("post-encephalitic parkinsonism", with neurofibrillary tangles in the substantia nigra neurons instead of Lewy bodies), some cases of chronic traumatic encephalopathy (professional boxers South. Med. J. 82: 543, 1989), and the "designer drug" (MPTP, "Ecstasy") fiasco of a few years ago. Dopaminergic neurons are the only ones that take the drug up, and it produces mitochondrial damage and a permanent Parkinson-like syndrome ("The case of the frozen addicts!") If you have had methamphetamine hospitalization since 1995, you have a 75% greater chance of now having Parkinson's -- this matches animal models (JAMA 306: 814, 2011).
Most cases of Parkinsonism do not seem to be familial. The known Parkinsonism genes:
In non-familial Parkinsonism having an identical twin with the disease does NOT increase your risk. This is now a robust finding (Neurology 63: 305, 2004). Since environmental risk factors are also elusive, and since twins tend to spend much of their lives together, your lecturer believes that there is a post-zygotic mutation involved -- and since the disease tends to announce itself asymmetrically, perhaps there is also a mitochondrial component.
* The epidemiologic link between insecticide and/or herbicide exposure and Parkinsonism continues to be discussed, especially since MPTP produces permanent Parkinsonism and works like many insecticides on the mitochondrial complex 1 system. Nobody's been looking hard at the epidemiology in recent years; living your life in farmland seems to be a risk, and there was a study where Dieldrin was found in 6 of 20 Parkinson's brains, and none of 14 controls (Ann. Neuro. 36: 100, 1994), and two pretty-good-looking epidemiologic studies (Neurology 43: 1150, 1993; Neurology 42: 1328, 1992). Rotenone, which like other insecticides resembles MPTP chemically and pharmacologically, produces Lewy body parkinsonism in mice (Science 290: 1068, 2000). An animal model showing enhancement of synucleinopathy by insecticides: Am. J. Path. 170: 658, 2007. So far there's no model of the chronic disease using herbicides, though some of these produce acute effects on the dopaminergic system as do many other substances (Science 290: 1068, 2000).
The claim that cigaret![]() smoking is protective against Parkinsonism is by now clearly
true
(Neurology 45: 1041, 1995; Epidemiology 10: 327, 1999). So is caffeine (Drugs & Aging 18:
797, 2001).
smoking is protective against Parkinsonism is by now clearly
true
(Neurology 45: 1041, 1995; Epidemiology 10: 327, 1999). So is caffeine (Drugs & Aging 18:
797, 2001).
Most Parkinson's cases are "idiopathic", and begin in later middle age. Look for the distinctive (but not pathognomonic) "Lewy bodies" in dopaminergic (and other) neurons. Big autopsy series: Arch. Neuro. 50: 140, 1993.
* Acupuncture and every other "complementary / alternative remedy" studied for Parkinsonism have been flops (Neurology 57: 790, 2001).
* Around 7% of Parkinson patients taking dopaminergic medications become pathological gamblers (BJM 334: 810, 2007).
The adrenal medulla autotransplantation experiment resulted in non-viable grafts. An animal model of Parkinson's responds dramatically to embryonic stem cell therapy: Proc. Nat. Acad. Sci. 99: 2344, 2002. Update Neurology 66(S4): S89, 2006. Even better Proc. Nat. Acad. Sci. 105: 5856, 2008).
Remember the parkinsonism mimics, which include multi-infarct disease,
manganese toxicity,
Lyme disease![]() (Arch. Path. Lab. Med. 127: 1204, 2003), and now West Nile.
(Arch. Path. Lab. Med. 127: 1204, 2003), and now West Nile.
* James Parkinson, the first person to distinguish and describe the illness, was a progressive political activist throughout his life. As a young man, he was implicated in the "pop-gun" plot to assassinate George III with a poisoned dart; thankfully, the business was soon forgotten. Later in life, he was a strong advocate for the protection of the mentally ill and their families, and became interested in the new sciences of paleontology and geology.
CORTICOBASAL DEGENERATION (formerly "Pick's Type B") is a dementing disease with balloon cells, a distinctive tau-based pathologic lesion around astrocytes, and motor problems (notably alien limb, "My hand escaped and is doing its own thing.")
* These people often have "globose" neurofibrillary tangles, with straight rather than twisted filaments, as in progressive supranuclear palsy. Also look for tau staining immediately around the nucleus.
A few genes are known or suspected, most notably a progranulin allele (Brain 131: 732, 2008).
The disease is notoriously unresponsive to therapy. Reviews: J. Neuro. Neurosurg. Psych. 68: 304, 2000; Arch. Neuro. 55: 957, 1998, pathology J. Neuro. 246 S-2: II 6-15, 1999.
* Today's clinician may diagnose "corticobasal syndrome" when there is non-fluent aphasia, alien hand, apraxias, and/or parkinsonism in some combination. Imaging can help distinguish true corticobasal degeneration from its mimics, including some cases of Alzheimer's, progressive supranuclear palsy, and TDP-43 Pick's (Neurology 75: 1879, 2010).
MULTIPLE SYSTEMS ATROPHY (NEJM 372: 249, 2015)is now considered a single disease, because of its distinctive inclusions in the oligodendoglia.
The inclusions (* Papp-Lantos bodies) contain alpha-synuclein. Nobody really understands them.
STRIATONIGRAL DEGENERATION (* multiple system atrophy P for "Parkinson-like") is a degenerative disease in which the caudate and putamen atrophy along with the substantia nigra. Patients have a similar clinical syndrome to Parkinson's, but do not respond to L-Dopa therapy and do not have Lewy bodies.
SHY-DRAGER (* multiple system atrophy A for "autonomic"; see Ann. Int. Med. 125: 194, 1996) is striatonigral degeneration with the loss, in addition, of the intermediolateral neurons of the spinal cord and resulting autonomic disturbances. I've never seen a case, though it's in the differential diagnosis of every patient with orthostatic hypotension, and is perennially discussed.
OLIVOPONTOCEREBELLAR ATROPHY / DEGENERATION (* multiple system atrophy C for "cerebellum") is still the name for a grab-bag of diseases with similar anatomic pathology -- loss of neurons from the basis pontis, cerebellar cortex, substantia nigra, and inferior olive. (The inferior olive is reported to disappear whenever the cerebellum is wiped out, due to post-synaptic degeneration.) It still includes the genetic spinocerebellar ataxias I and II. In non-hereditary olivopontocerebellar degeneration, one often sees the oligodendroglial inclusions typical of mutliple systems atrophy.
PROGRESSIVE SUPRANUCLEAR PALSY ("PSP", Steele-Richardson) is an underdiagnosed, fairly-common (Neurology 44: 1015, 1994; Med. Clin. NA 83: 369, 1999; J. Clin. Path. 54: 427, 2001) dementing disorder of older adults with eye movement disorders (especially, problems with downward gaze), other movement disorders, and often dementia.
* Ask a radiologist to show you the "penguin sign" -- atrophy of the tectum of the midbrain.
* Neurofibrillary tangles in PSP have straight, rather than twisted, filaments. PSP as a taupathy; Lancet 356: 170, 2000.
A parkinsonism/PSP variant that is rampant on the island of Guadeloupe, complete with the NFT's in the substantia nigra and subthalamic nuclei, and astrocyte tufts (Brain 125: 801, 2002) is probably caused by ingestion of the jungle-fruit Annona muricata neurotoxin annonacin (Brain 130: 816, 2007; J. Neurosci. 27: 7827, 2007). "Complementary medicine" folks take note: This is one of the supposedly-good-for-you alkaloids in the herbal cancer remedy "Graviola."
* A mutant tau allele is a feature of at least one kindred with the ultra-rare dementing disorder "progressive subcortical gliosis" (Nat. Med. 5: 454, 1999); another lacks it (Neurology 72: 260, 2009).
FTDP-17 ("frontotemporal dementia with parkinsonism linked to chromosome 17") is caused a mutation of tau itself (Mech. Aging 127: 180, 2006; Brain 128: 2645, 2005) or the nearby protein progranulin (Nature 442: 916, 2006; Arch. Nero. 65: 460, 2008). As with other subcortical taupathies, you might see tau inclusions in the oligodendroglia (J. Neurosci. 25: 9493, 2005).
ARGYROPHILIC GRAIN DISEASE, with silver-staining tau granules in limbic neurons (different from granulovacuolar degeneration, and without other Alzheimer features) is a common, newly-recognized entity seen in very old folks, with amnesia, delusions of persecution, and agitation (Acta Neuropath. 111: 320, 2006; now well-known Brain 131: 1416, 2008.) It's been under-recognized since special variants of the silver stains are required to see its lesions.
LEWY BODY DEMENTIA features neurons packed with synuclein-rich Lewy bodies throughout much of the brain. These patients have a rapid Alzheimer-like illness with some extrapyramidal symptoms (stiff and slow but usually no tremor), visual hallucinations (visual cortex lesions demonstrable on scan Brain 135: 569, 2012), and (often) exquisite sensitivity to the older neuroleptic drugs (chlorpromazine, etc. -- try one of the newer "atypical antipsychotics" instead.) It's not rare, but seldom diagnosed in life. See Br. Med. J. 305: 673, 1992; Neurology 42: 2131, 1992; clinico-pathologic correlation including tips on how to tell this from Alzheimer's in life Arch. Neuro. 59: 43, 2002.
* Update on selective involvement of neurons in the caudate, and a correlation with neurophysiology: Neurology 66: 1591, 2006.
* Glucocerebrosidase mutations and Lewy body dementia: Arch. Neuro. 66: 578, 2009.
TORSION DYSTONIA ("dystonia musculorum deformans") is a disease of children in which the muscle tone increases around the body, twisting it into curious positions. The one known gene is Torsin A (TOR1a / DYT1) which does not always express completely (Neurology 59: 445, 2002; Arch. Neuro. 57: 333, 2000.) The anatomic pathology in the brainstem includes inclusion bodies (not well-characterized; Ann. Neuro. 56: 540, 2004) and since the disease comes on over time, there's probably neurodegeneration involved. Neurosurgical procedures on the deep brain structures has resulted in spectacular recoveries (review Ped. Neuro. 14: 145, 1996).
* HEREDITARY SPASTIC PARAPLEGIA ("familial spastic paraparesis, etc.; Arch. Neuro. 60: 1045, 2003) is a family of thankfully-rare progressive genetic disorders (dominant and recessive) of varying expressivity. For some reason, the long axons in the corticospinal tracts that supply the legs undergo degeneration with the neurons themselves being preserved. At least eight loci are already known (J. Neuro. Neurosurg. Psych. 72: 43, 2002; pathology of the "spastin" mutant variant Neurology 55: 89, 2000).
ESSENTIAL TREMOR ("benign familial tremor") is a very common (1-2% of humankind), usually banal (sometimes severe) intention tremor. It is inherited as an autosomal dominant (possible loci Neurology 68: 790, 2007 and Brain 130: 1456, 2007), first manifests around age 20, and typically vanishes as soon as the "patient" drinks one beer (i.e., here's the three questions you need to ask to pretty-much clinch the diagnosis). If the patient really wants to be treated, or it's severe, try low-dose propranolol or gabapentin (Arch. Neuro. 56: 807, 1999) or mysoline or any of a variety of others (Am. Fam. Phys. 86: 292, 2012). More important, explain the nature of the process, and that it is NOT Parkinsonism or mental illness.
* Focused ultrasound to the ventral intermediate nucleus of the thalamus to treat severe essential tremor: NEJM 369: 640, 2013.
THE SPINOCEREBELLAR ATAXIAS (update Mayo Clin. Proc. 75: 475, 2000; the autosomal recessive group NEJM 366: 636, 2012.)
This array of autosomal degenerative diseases has recently been sorted out thanks to the Human Genome Project. Except Friedreich's and ataxia with vitamin E deficiency, all are autosomal dominant. The pathologist sees only neuronal loss and maybe gliosis.
TYPE I SPINOCEREBELLAR ATROPHY feature damage to the gene for "ataxin 1", and this also exhibits long tandem repeats and Sherman's paradox (see below; Nat. Neurosci. 3: 157, 2000). So do TYPE II (ataxin 2; Eur. J. Hum. Genet. 7: 841, 1999) and TYPE III (Joseph's, a Portuguese ethnic disease and probably the commonest in this group, ataxin 3). All these do their harm by producing a product whose long repeats gum up the nucleus. (I predicted in 1990 these would prove to be Sherman paradox diseases, and they did.) As in the "olivopontocerellar atrophy" variant of multiple systems atrophy, neurons are selectively lost form the basis pontis, inferior olives, cerebellar cortex, and substantia nigra.
FRIEDREICH'S ATAXIA is an autosomal recessive disease with somewhat variable expressivity. Onset is in late childhood, when pes cavus (high-arched feet), clumsiness and speech problems develop. Patients become wheelchair-bound after a few years, and may have a cardiomyopathy with thick walls (not the "classic" hypertrophic cardiomyopathy though). There is gliosis of the posterior columns, dorsal corticospinal tract, and spinocerebellar tracts; the cerebellar cortex and other motor areas may also be involved. The cause is trinucleotide repeats in frataxin, a gene responsible for keeping iron from accumulating in mitochondria; Gene and review: Science 271: 1423, 1996; update Arch. Neuro. 59: 743, 2002.
* Update for clinicians: Arch. Neuro. 64: 558, 2007.
ATAXIA WITH VITAMIN E DEFICIENCY mimics Friedreich's, but is caused by lack of vitamin-E transfer protein. Of course this is also autosomal recessive. Giving the vitamin in big doses is effective treatment. See NEJM 333: 1313, 1995. Though very rare, it's the only really treatable entity in this group, so be sure to think of it!
* Smith's dentatorubral atrophy is yet another Sherman's-paradox disease ("atrophin"; J. Biol. Chem. 274: 8730, 1999).
* The EPISODIC ATAXIA family of autosomal-domianants includes a mutation in the voltage-gated potassium channel gene; ataxic / dysarthric episodes especially follow a startle.
We've already mentioned ATAXIA-TELANGIECTASIA (gene ATM). The mechanism by which it causes neurodegeneration has remained elusive. The idea that it's a mitochondriopathy makes sense Am. J. Path. 172: 1445, 2008; Blood 119: 1490, 2012.
* Men carrying mild alleles of fragile X (i.e., not enough tandem repeats yet) are prone to develop cerebellar ataxias and dementia (Brain 125: 1760, 2002.)
|
AMYOTROPHIC LATERAL SCLEROSIS ("Lou Gehrig's disease"; "creeping paralysis";
motor neuron disease complex; Am. Fam. Phys. 59: 1489, 1999; NEJM 344: 1688, 2001;
BMJ 336: 658, 2008; Lancet 377: 942, 2011)
"Motor neuron disease complex" is actually four diseases, featuring loss of the motor neurons 1. Amyotrophic lateral sclerosis (loss of upper and lower motor neurons); this is the common one 2. Progressive bulbar palsy (cranial nerves are most severely affected) 3. Progressive muscular atrophy (lower motor neurons only) 4. Primary lateral sclerosis (upper motor neurons only) |
 Lou Gehrig |
ALS is a disease of older middle age, progressing to profound disability (usually without mental impairment) in a few years. Most ALS cases are sporadic (but see below). There is a slight male predominance
Current thinking has involved destruction of motor neurons by excitotoxicity (Mayo Clin. Proc. 66: 54, 1991; J. Neurol. 247-S1: I-7, 2000). This is supported by the finding that the anti-glutamate agent riluzole causes a modest slowing of the progression of ALS (NEJM 330: 585, 1994); it's now the only medication approved in the US for ALS and prolongs life by about two months (JAMA 298: 207, 2007; Clin. Pharm. Ther. 83: 718, 2008).
The sick neurons contain ubiquitin-positive inclusions of various sorts, thought to be altered or abnormal proteins that resist degradation (update Acta Neuropath. 113: 535, 2007). Most distinctive is the Bunina body of non-superoxide-dismutase-related disease, which looks like a string of beads, composed largely of cystatin C found in the remaining lower motor neurons.
There are other inclusions as well in most types of ALS; these are cystatin C-negative but stain with ubiquitin and TDP-43 (Science 314: 130, 2006; Am. J. Path. 173: 182, 2008); some of these patients have Bunina bodies, some don't (Arch. Neuro. 66: 121, 2009).
The link between cycad (false sago palm) flour and ALS-dementia-parkinsonism complex of the indigenous Chamorro people of Guam remains speculative. There is now an animal model using the toxin cycasin (Exp. Neurol. 155: 11, 1999). Thankfully the disease is becoming less common, but has not vanished. The locals have always washed the flour, supposedly being aware of the toxin; one group links the disease to the consumption of the ethnic delicacy -- a tasty fruit bat that lives on the sago palm (Neurology 58: 956, 2002). Like other ALS syndromes, this one is now known to be TDP-43 positive (Brain 130: 1386, 2007).
About 10% of ALS cases show simple mendelian inheritance. Many cases have a mutant C9ORF72 gene with a hexonucleotide repeat (Brain 135: 709 & 723 & 751 & 784 & 794, 2012). Others feature expanding CAG repeats in ATXN2 (ataxin 2, which we met earlier among the spinocerebellar ataxias): Neurology 76: 2066, 2011. The rest are probably polygenic with environmental modification.
As you'd expect, mutated TDP-43/TARDBP has been discovered as a cause of familial ALS (Arch. Neuro. 65: 1185, 2008; Neurology 77: 1427, 2011).
* Motor neuron disease from mutant dynactin: Nat. Genet. 33: 455, 2003. The FUS/TLS locus: Arch. Neuro. 67: 455, 2010 (some "sporadic" cases are new mutations).
* Another locus (alsin, ALS2): Nat. Genet. 298: 160, 2001; Arch. Neuro. 60: 1768, 2003. A juvenile form with mutated FUS and basophilic inclusions: Neurology 75: 611, 2011.
Amyotrophic lateral sclerosis is the classic disease cited in considerations of physician-assisted suicide. (Why?) About one Dutch patient in five now chooses this route (NEJM 346: 1638, 2002). And a majority will consider assisted suicide, but most will choose hospice instead (NEJM 339: 967, 1998).
The key illness to rule out in apparent ALS is MULTIFOCAL MOTOR NEUROPATHY, caused by autoantibodies against GM1 ganglioside. This responds to treatment as other autoantibody diseases (cyclophosphamide, gamma globulin, now rituximab Neurology 63: 2178, 2004).
* KENNEDY'S DISEASE is a bulbospinal atrophy and lack of masculinization of male patients, caused by lack of an androgen receptor. This is yet another trinucleotide repeat disease.
WERDNIG-HOFFMAN DISEASE (spinal muscular atrophy type I) is an autosomal recessive disease causing loss, in the few months before and after birth, of most of the lower motor neurons. It is the most severe of the spinal muscular atrophies, caused by various mutations at the SMN ("survival motor neuron") locus (Nat. Genet. 16: 265, 1997); we covered these under "Muscle".
Even in the DSM-IV era, I find Bleuler's "Four A's" helpful: Autism (apparent absorption in self and fantasy), Ambivalence (maintaining contradictory attitudes in logic-tight compartments, with striking lack of insight), loose Associations, and flat Affect. In schizophrenia, these are much more striking even than in us "normal folk".
Sensitive physicians know that the negativism, coldness, and lack of motivation of the schizophrenic can be as upsetting to family members as the delusions and hallucinations. Tell them it's nobody's fault and that it isn't that they are not loved.
Reasonably good models for schizophrenia (i.e., both being very crazy and being oriented in the
three spheres) include acute intermittent porphyria, lupus, chronic mercury poisoning, ergotism,
pellagra, neurosyphilis![]() , frontal lobe meningioma, and some of the psychedelic experiences.
, frontal lobe meningioma, and some of the psychedelic experiences.
 One Flew Over the Cuckoo's Nest |
 Shakespeare's Ophelia |
Until the mid-1990's, all public discussion of schizophrenia was dominated by ideology. In the 1960's
("B.F. Skinner says..."; "All people are
born the same and if you aren't getting what you want, it is society's fault"; etc.), behaviorists wrote
dogmatically about "the schizophrenogenic mother" ("She said to the child, 'I love you', but her body
language said otherwise, and this prevented the child from distinguishing fantasy from reality"; "the
double bind", etc., etc. Today's historians say a generation of mothers needs
an apology: Lancet 379: 1292, 2012.) In the early 1970's, it was all the fault of "the schizophrenogenic father"
instead; as with the "S-mother", evidence was "anecdotal" (i.e., the biological parents of crazy
people act screwy themselves; stress sometimes precipitates symptoms) and "based on sound theory"
(i.e., "all people are born the same", the left-wing/Skinnerian ideology of the day).
Some 'sixties
revolutionaries discussed schizophrenia as "a disease caused, more than any other, by our
reactionary society", or denied its existence altogether (a Dr. Thomas Szasz, author of The Myth of
Mental Illness, described witch-hunts and incarcerating people just for being different).
'Sixties rhetoric emphasized that traditional society was unreasonable
and thus the people in the mental hospitals must be the sane ones.
"The King of Hearts" put this on the silver screen.
Ken Kesey
(One Flew Over the Cuckoo's Nest) and Dr. R.D. Laing (The Politics of Experience) wrote their
best-sellers. (Dr. Laing's own life-story was an ugly one.) The ACLU defended the rights of crazy
people to refuse treatment (one 1970's study showed 99% were totally grateful after being brought
back to earth). And some psychologists inveighed against the use of the obviously-effective
phenothiazine drugs, which began cutting through hallucinations and delusions as soon as they were
introduced in the 1950's. Confusing fantasy with reality always causes problems,
and the beautiful 'sixties rhetoric resulted in disaster for the
mentally-ill and their families.
Today, only a few psychoanalysts still talk about curing schizophrenia
through psychotherapy, and the rest of the world (even the other psychiatrists) just laughs at them (Nature
354: 693, 1991 was the last gasp). There are still
occasional complaints from non-physicians
about psychiatry being wicked because
it is "authoritarian",
or obsolete because it is "culture-bound" or "institutionalized" or
"modernist rather than postmodernist"
(Br. Med. J. 322: 724, 2001). These people
ignore the fact that since the 1940's,
free-world psychiatrists have only used
coercion when a person cannot take care of himself/herself
or a danger to others, and an examination of any psychiatry textbook will show
that the discipline is characterized by a variety of perspectives and ways of
understanding a particular person's problems.
The end result of all of the "enlightened thinking",
of course, was de-institutionalization ("out of the back wards, into the back
alleys"). This pleased the Left ("We're for every individual's freedom to be different"; "Even though
the inmates got free food, clothing, shelter, medical care, and protection, and were otherwise
unemployable, it violated their civil rights to have them work in the laundry and not get minimum
wage and benefits"), the Right ("We're against able-bodied people living at public expense"),
optimistic physicians ("The grateful patients will come regularly to their community mental health
centers to get their medicines refilled"), and real humanitarians (there were, after all, serious abuses
in the old "asylum" system). Well, everybody was pleased at first.... Today, the non-compliant
mentally-ill whose families can no longer stand them are homeless, and this gets described as a
"human rights problem" by the same people who got the asylums closed in the 1970's. Do you think
Dr. Szasz ("Mental illness is a myth") has ever talked to his local "bag person"? By the way,
schizophrenics ARE more likely to commit crimes, including violent crimes, including murder (Psych.
Clin. N.A. 15: 575, 1994; a schizophrenic is 8 times as likely to commit murder as a non-psychotic
counterpart: Arch. Gen. Psych. 53: 497, 1996),
and only a fool believes that psychiatry can protect
the public in today's political-economic "mental-health" environment.
I hope that no one was surprised by an enormous study from Duke
(Arch. Gen. Psych. 63: 490, 2006) that withdrawn schizophrenics
rarely commit crimes but that people raging around and having delusions
of persecution are very likely to hurt somebody.
The best we're doing nowadays is "leveraging" --
the person doesn't get his/her welfare check if he/she does something
violent (Am. J. Psych. 163: 1404, 2006; and the lawyers are
all over this; it's emerged that during a six-month period, about 20% of those collecting
welfare for mental illness will admit to hurting someone or at least
threatening someone with a lethal weapon; same rate as the Duke study above.)
The truth is that schizophrenics are more likely than non-schizophrenics
to commit all categories of crime except sex crimes (Lancet 355:
614, 2000). In fact, people who stalk strangers (rather than
previous sex partners) are usually psychotic (Lancet 355: 199, 2000).
Even writers who seem to be advocates for "community mental health"
and who emphasize that a majority of stranger-murders result from fights
in bars or among druggies cannot hide the reality of senseless violence
from schizophrenics (especially against family members and friends: Br. Med. J. 328: 754, 2004).
As part of the illness, many schizophrenics
do not believe they are sick, and do not want to take their medicine.
Thanks mostly to "laws that
protect the rights of the specially-challenged", it remains
extremely difficult
to keep a schizophrenic confined
even after multiple episodes of dangerous behavior.
The
shooting of two guards in the US capitol by a
chronically belligerent, chronically threatening,
non-compliant schizophrenic named Russell Eugene Weston who had just
been given "Greyhound therapy" (a one-way bus ticket out of the state)
by the Montana mental-health system should have had an impact, but it didn't.
Michael B. Laudor, a schizophrenic who successfully completed
the curriculum at Yale Law School and who sold book and movie rights to his
success story for $2 million, stopped taking his medicine and a few days later
stabbed
his pregnant girlfriend to death. In both of these high-profile cases,
the families knew there was going to be trouble, but couldn't do anything.
In 1982, the parents of Larry Robison did everything they could to have him forcibly treated,
but were unable to prevent his committing mass murder.
Anders Breivik, the 2011 Norwegian mass-killer, went unnoticed because he hung out
with other political crazies.
A mental patient is most likely to kill
a family member when
the family denies, misunderstands, or "spiritualizes" the illness
(chilling reading: Crim. Behav. Mental Health 15: 154, 2005).
The much-hyped "study" (Arch. Gen. Psych. 55: 393, 1998)
finding that mentally-ill people in the community
were no more likely to be violent than their underclass
neighbors suffered from serious
flaws, including omitting anybody who had been in jail, and not counting
threats of violence, swinging-and-missing, fire-setting, or trashing rooms
as being violent.
The "study" also lumped in the burned-out schizophrenics, who are generally very passive and
withdrawn, with the active and obviously troublesome ones.
More recently, several studies have made it clear that
schizophrenics are much more likely to commit
violent crimes, especially violent sex crimes (Crim. Behav. Ment. Health 14:
108, 2004 -- note the conflict with some previous studies).
A schizophrenic (compared with a non-schizophrenic)
is over four times more likely to have been convicted of a
crime (21.6% vs. 7.8%), and a violent
crime (8.2% vs. 1.8%); the rate of substance abuse among schizophrenics
is tremendously high but this doesn't explain all of this (Am. J. Psych. 161:
716, 2004; also JAMA 301: 2016, 2009).
At present, there are maybe 300,000 or 400,000 chronically mentally ill Americans
confined in jails and prisons. (Many are in jails for vagrancy.) There are
only about 80,000 people in long-term mental health facilities.
The truth is that
this represents a conscious decision by society
to turn care of these people over to law enforcement personnel (who are,
for the most part,
reality-oriented and respectful of the legitimate rights of all people)
rather than non-physician (and non-scientifically-oriented)
"mental health experts".
But the damage has been done.
In the past decade, the phenomenon of "mental health courts", judicial-system
courts focused
on managing these people, has become widespeard; expect continued
growth (JAMA 297: 1641, 2007).
The New England Journal is troubled by the "epidemic of incarceration",
noting that a great number of these people are mentally ill
(NEJM 364: 2081, 2011), but offers no better solution
in a society where we cannot deal otherwise with the non-manageable,
non-complaint mentally-ill.
One of the major moral failures in my life was not speaking up when
a group of mental health professionals
called a nun a "self-righteous bitch"
for no other reason than saying that she preferred -- just for herself --
a celibate lifestyle
devoted to caring for the sick and needy. (My course evaluation
would probably have been
affected adversely, but I'm still ashamed I said nothing.
This happened in 1974 or 1975.) It was at that moment that I realized who was
really "caring for the mentally ill" in the community. Next year,
on my "psych" rotation,
the physicians talked to me again and again about how frustrating
it was to have to work with such screwy "fellow-professionals" who wielded so much power.
Perhaps things have changed since the mid-1970's.
Among my favorite articles from the 1990's was
"The Government-Sponsored Revolving Door" in NEJM 333:
777 & 794, 1995. Schizophrenics on welfare learn to act crazy and get admitted while they're broke
and waiting for their checks, and recover when the check arrives; and in the study sample, the
typical welfare-schizophrenic's largest single expenditure was for cocaine.
When psychotic symptoms are emerging, cognitive therapy
of course does not reduce progression to psychosis or the distress that it
causes, but seems to help these unfortunates cope somewhat better
(BMJ 344: e2233, 2012). Not surprisingly, group art therapy does not help schizophrenics (BMJ 344: 846, 2012).
It is now perfectly clear
that schizophrenia is a major organic nervous system
disease. Before the disease fully manifests itself, brain cells die off and
brain atrophy occurs (Am. J. Psych. 155: 1661, 1998); this is
already well-underway during the first episode (Am. J. Psych. 157:
1829, 2000). Certain
association areas in the cortex and thalamus are hit especially hard
(Am. J. Psych. 159: 59, 2002; Arch. Gen. Psych. 60:
878, 2003; counting dendritic spines Am. J. Psych. 162:
1200, 2005); the more cortex lost, the worse
the outcome (Am. J. Psych. 158: 1140, 2001); all patients have gray
matter lesions and enlarged third ventricles, while the more impaired ones
also have white matter lesions and enlarged lateral ventricles (Am. J. Psych. 166:
189, 2009).
For a review of various studies at the light microscopic level,
see Brain 122(4): 593, 1999; findings differ in different studies but
generally agree that there is neuronal
loss and cellular disarray in the cortex, without
gliosis.
The loss is selective, with the dorsolateral prefrontal cortex severely involved
and nearby Broca's area completely spared (Arch. Gen. Psych. 60: 69, 2003;
Am. J. Psych. 159: 1983, 2002); the more that's gone, the worse
the outcome (Am. J. Psych. 158: 1140, 2001).
The volume loss in the superior and middle temporal gyri is by now very
well-known and there is talk about its being specific for schizophrenia
(Am. J. Psych. 163: 2103, 2006).
A rigorous study shows a distinctive pattern of loss in the basal ganglia
(Brain 130: 678, 2007).
There is more loss of cortex (and poorer outcome) over time if the patient gets classical antipsychotic agents,
and LESS loss of cortex (and better outcome) than the untreated if the patient gets the newer agents
(Arch. Gen. Psych. 68: 871, 2011).
Counting dendrite intersections: Am. J. Psych. 161: 742, 2004.
Further, schizophrenics have by-now-well-characterized volumetric loss of
the white matter of the frontal, pareital, and fronto-parietal junctions at
onset, and these get worse over time (Am. J. Psych. 164: 1082, 2007).
Old studies of genetics are now giving way to the discovery of loci.
Familial schizophrenia locus Science 288: 678, 2000.
Neuregulin 1: Am. J. Hum. Genet. 71:
877, 2002; Am. J. Hum. Genet. 72: 83, 2003.
More on the genetics: Lancet 361: 417, 2003.
Update JAMA 299: 2017, 2008.
"The schizophrenia susceptibility pathway": Nature Medicine 17:
470, 2011.
Even in
cases without simple inheritance, the genes obviously dominate family environment (old work
on schizophrenia
genetics: Lancet 1: 79, 1989; Nature 339: 305, 1989; Nature
340: 391, 1989; non-schizophrenic relatives
tend to be a little-bit screwy and fill DSM criteria for schizophrenia-like illnesses Arch. Gen. Psych.
50: 527, 1993, J. Nerv. Ment. Dis. 182: 443, 1994; the adoption studies from Scandinavia, where
they keep good records: Arch. Gen. Psych. 51: 442, 1994; and the neuroimaging
studies show similar hippocampal changes Arch. Gen. Psych. 64: 297, 2007).
The three best known loci (and all are clearly real) that confer susceptibility to
schizophrenia are DYSBINDIN (DTNBP1), a protein expressed
on the glutamine neurons (J. Clin. Invest. 113: 1353, 2004); altered
forms run especially with schizophrenic negativism (Am. J. Psych. 162: 1824, 2005;
Am. J. Psych. 163: 532, 2006).
DISC1 ("disrupted in schizophrenia") and NEUREGULIN-1 (NRG1) are also major loci (update Nature 458: 976, 2009).
There are conflicting results as to whether RGS4 is a schizophenia locus or not
(Curr. Op. Psyc. 22: 154, 2009 -- reviews all the candidate genes and the
postmortem brain chemistry.) Of course, the candidate genes are interconnected in
the "schizophrenia susceptibility pathway" (Nat. Med. 17: 470, 2011).
This is centered on the glutamine pathway, not the dopamine pathway.
Watch for novel agents, but in a disease in which there are actually lost neurons,
don't get your hopes up.
Same or crazy, your DISC1 alleles seem to have to do with whether you're a socializer
or a loner (Arch. Gen. Psych. 66: 134, 2009).
KCNH2, a potassium channel: Nat. Med. 15: 448 & 509, 2009.
Another locus called PCM1 runs with low orbitofrontal cortical volume
and risk of psychosis (Arch. Gen. Psych. 63: 844, 2006).
In twins discordant for the disease,
magnetic imaging detects distinctive differences in the brains of the schizophrenic twin (NEJM 322:
789 & 842, 1990) which have been confirmed by neuropathologists (Schiz. Res. 3: 295, 1990; Br.
Med. J. 305: 327, 1992; South. Med. J. 85: 907, 1992; more on twins J. Nerv. Ment. Dis. 181: 290,
1993). In monozygotic twins who are clearly discordant for schizophrenia, being the crazy twin
correlates very strongly with obstetrical complications and/or problems during pregnancy or shortly
after birth (Am. J. Psych. 151: 1194, 1994; there was no relation to trauma or to substance abuse;
also Am. J. Psych. 157: 196, 2000; pre-eclampsia as a major risk Arch. Gen. Psych.
56: 234, 1999).
In the poor nations, where obstetrical catastrophes and infantile brain trauma are more common, the
rate of schizophrenia is supposedly no higher, but there's a strong link to these insults (Am. J. Psych.
151: 368, 1994). And prenatal exposure to famine and malnutrition is a strong
risk factor: Am. J. Psych. 157: 1170, 2000; strong confirmation JAMA 294:
557, 2005.
Currently, there's a lot
of interest in obstetrical complications and/or a catastrophe during the second trimester of gestation
as the added insult that makes the hereditary trait manifest itself: Br. Med. J. 305: 1256, 1992; Am.
J. Psych. 149: 1355, 1992. And so forth. Schizophrenia's gotta be
"multifactorial", with etiologies differing from patient
to patient,
and the psychiatrists had this settled by the early 1990's (Psych. Clin. N.A. 16: 269,
1993; Schiz. Bull. 19: 355, 1993).
Also impressive is the finding of a striking increase in sporadic
(not familial) schizophrenia following
influenza A
![]() infection in the fifth month of pregnancy
(Lancet 337: 1248, 1991; Arch. Gen. Psych.
47: 869, 1990; Am. J. Med. Genet. 48: 40, 1993).
There is a huge excess of schizophrenics born in February and March, and in the city
rather than in the country (NEJM 340:
603, 1999).
An arcane statistical study of mental and
behavioral illnesses that affect primarily the poor (Science 255: 946, 1992) concludes that (in
contrast to depression, criminality, and illegal drug abuse), the tendency to schizophrenia causes
downward social mobility, and is not the result of bad living conditions.
infection in the fifth month of pregnancy
(Lancet 337: 1248, 1991; Arch. Gen. Psych.
47: 869, 1990; Am. J. Med. Genet. 48: 40, 1993).
There is a huge excess of schizophrenics born in February and March, and in the city
rather than in the country (NEJM 340:
603, 1999).
An arcane statistical study of mental and
behavioral illnesses that affect primarily the poor (Science 255: 946, 1992) concludes that (in
contrast to depression, criminality, and illegal drug abuse), the tendency to schizophrenia causes
downward social mobility, and is not the result of bad living conditions.
| * Today's neuroleptic-antipsychotic drugs are potent dopamine antagonists, and dopamine-like drugs (notably amphetamine) can make a person act crazy and paranoid (but without the distinctive thought disorder of the schizophrenic). However, the old story about "high dopamine causes schizophrenia, low dopamine causes Parkinsonism, they are two ends of a continuum" just doesn't hold up to today's neuroscience; there are places in the schizophrenic's brain where dopamine is high, and other places where it is low (Am. J. Psych. 148: 1301 & 1474, 1991; striking decrease in D1 receptors in the prefrontal working-memory-processors that in turn correlates with the negative symptoms: Nature 385: 634, 1997). And the newer anti-schizophrenic drugs (clozapine, etc.) are "atypical neuroleptics" that selectively block the subset of dopamine receptors (D4) not involved in the extrapyramidal side effects of the more familiar anti-schizophrenic drugs, as well as 5HT2a receptors. Watch for more about D4 protein, which varies from person to person, and the origins of psychiatric illness: Nature 358: 109 & 149, 1992. D4 allele correlates with novelty-seeking / thrill-seeking (Nat. Genet. 12: 78, 1996). D2 claims flop: Science 264: 1696, 1994. |
 A Beautiful Mind |
* More plausible is the phencyclidine model for schizophrenia (ever see someone go crazy on "angel dust?"), and there's some new evidence that the N-methyl-D-aspartate receptor (blocked by phencyclidine and ketamine) is defective in schizophrenia (Am. J. Psych. 148: 1474, 1991; the ketamine model Arch. Gen. Psych. 51: 199, 1994). Not much more lately, but watch these.
 The Caveman's Valentine | De-stigmatize and de-mystify this dread illness -- and explain the hallucinations not as "evidence of being crazy", but as exaggerations of perceptual errors that happen to anyone under stress (J. Nerv. Ment. Dis. 179: 207, 1991). The more the family misunderstands (and therefore criticizes) the patient, the worse the prognosis (Lancet 340: 1007, 1992); your role as educator is extremely important here. Tip: To control "the voices", try one ear plug, or a Walkman, or singing softly to oneself (Br. Med. J. 302: 327, 1991). There was a flap in the early 1990's about neuroleptic treatment causing earlier onset of Alzheimer's in schizophrenics. It's evidently not so (Am. J. Psych. 154: 861, 1997 autopsy studies.) Today there is talk about returning motivated schizophrenics to near-normal function (meaningful work, meaningful friendships) through cognitive-behavioral therapy, support for individuals and families, and other training (JAMA 312: 16, 2014). |
CHILDHOOD AUTISM (formerly "childhood schizophrenia", semi-glamorized in the film "Rain Man"; reviews NEJM 347: 302, 2002; Lancet 374: 1627, 2009)
This is an inborn (usually), organic, sometimes-familial, usually sporadic disease of the brain that impacts dramatically on children's ability to imagine, socialize and communicate. The kids show intensive interest in one or two subjects, exhibit a narrow and repetitive lifestyle, lack intonation and body language, and show poor muscular coordination. You'll learn about the way these children think and behave on "Pediatrics". With the increased interest in autism, new criteria that seem to this observer to include a huge number of poorly-understood entities (language-delays, social-skills delays) that can't possibly be a real spectrum, and the fact that a child diagnosed with "autism" gets far more resources than a child who's "retarded", the frequency of diagnosis has increased spectacularly.
There's a consensus now that the disease generally arises from neuronal problems that begin before birth. By now, the morphometric differences between autistic and non-autistic populations are robust and consistent from nation to nation (Brain 128: 268, 2005; Arch. Gen. Psych. 61: 291, 2004; Brain 124: 1317, 2001). There is less gray matter in the fronto-striatal and parietal areas, smaller hippocampus, and less white matter in the cerebellum and fornices. Autistic children's brains actually average larger than those of typically-developing children (Neurology 59: 184, 2002). The neuropathology findings are also being clarified (small cells in places in the limbic system, abnormal microcolumn architecture in the frontal cortex, others: Brain 127: 2572, 2004; Neurology 58: 428, 2002), but this will be much more difficult.
A famous feature of a few (not all) children diagnosed today with autism is "loss of acquired speech or communication skills at any age" ("regressive autism"). In other words, some of these children lose circuitry at a point in time, as in other neurodegenerative diseases and in some of the autoimmune nervous system diseases. This is often sudden, and I suspect this is the reason that parents are convinced that immunizations are the cause. Whether this is ever true is for you to decide -- but it's devastating to families.
As noted, autism sometimes seems to have an onset sometime during the first three years of life, and again, this may be fairly sudden. This makes sorting out "possible causes of autism" much more difficult, and makes evaluating anecdotal evidence all the more frustrating. What's more, occasionally there IS a primary cause. Autism developing secondary to a brain tumor: Dev. Med. Child. Neuro. 34: 252, 1992. And exactly what "autism" is remains a question -- kids with common Rett's ("regressive autism", several loci, lethal to the male before birth), Down's, tuberous sclerosis, etc., etc., can have "features of autism".
It's also now obvious that epigenetics involving genes for communication, social behavior, and cognition are altered in many (perhaps all) kids with real autism (Arch. Gen. Psych. 69: 314, 2012).
* Norwegian mothers who supplement with folic acid are only about half as likely to have a baby with real autism (JAMA 309: 570, 2013.)
A finding that now seems robust is that members of occupations that do a lot of information-processing (i.e., engineers, scientists, and accounts) are over-represented among parents and grandparents of autistic children (Autism 5: 223, 2001), and to excel, as do the autistic themselves, on the Embededed Figures Test (Neuroimage 35: 283, 2007; J. Aug. 36: 677, 2006; J. Child. Psych. 47: 639, 2006; more). Most physicians will draw the same tentative conclusion that I have -- autism is polygenic, perhaps with an environmental influence, and results from homozygosity for alleles that make heterozygotes into effective student-learners-techies.
The genetics of autism are just now being worked out, In particular, watch SHANK3 (NEJM 365: 173, 2011). Whole-genome sequencing for autism families: Nat. Med. 21: 185, 2015. In three animal models of autism (mimics respectively of fragile X, Rett's, and tuberous sclerosis), molecular interventions have reversed the syndrome.
Autism is a continuum, with the totally uncommunicative person at one end, and the odd, disliked, clumsy, loner kid who grows up to be a high-functioning, academically-inclined single adult after learning (by trial and error rather than instinct) how to relate to people (Lancet 350: 1761, 1997). In 2000, I predicted the fad for diagnosing super-nerds (young and old) as "suffering from Asperger's disease"; there are now special organizations and helpful guidance, but happily no real interest in getting special entitlements. See below.
* Pseudoscientists have been particularly cruel to those who care about autistic children. Bruno ("I'm
on the child's side!") Bettelheim, of U. of Chicago, assumed a priori that autism was the result of
abuse and neglect, scapegoated the parents, and treated these children in an intensive, lucrative
"orthogenic" milieu therapy. Of course, he never published his statistics, and he's now remembered
as a charlatan (Pr. Kind. Kind. 41: 316, 1992, abstract 93109943;
Skep. Inq. 24(6):12, 2000).
More recent autism charlatanism has been reviewed (Dev. Med. Child Neuro 47:
493, 2005), including a $50,000/year technique that falsely claimed cures and was promoted
as an "entitlement" that had priority over expenditures on teaching
reading and arithmetic to ordinary public school
students (J. Autism 28: 91, 1998). The study also reviewed what was
known to work at the time.
The "behavioral" approach that worked best, unfortunately, in its classic
formulation made major use of electric shocks, like training a zoo animal.
This is now politically incorrect and sometimes is banned, forcing families
to go to court (sometimes it's the only way to keep their children from ripping out their
own eyeballs.)
"Inclusivity" (the effort to get kids with autism into the classroom with regular students)
had no beneficial impact whatever on any outcome(Pediatrics 130(S2): 179, 2012).
Asperger's kids and adults can and should
be taught social skills. A few Rx's help sometimes.
In the late 1990's, no one was expecting any miracles.
* In the early 2000's, everything changed because
of politicial activism.
Having an autistic child acting up in a home may be extremely disruptive
to a family, even in the poor nations (Arch. Ir. Med. 12: 487, 2009),
parents have trouble holding down jobs (Pediatrics 121: e821, 2008);
1000 hours per year spent caring for the child (Sweden: Autism 11: 453, 2007), etc., etc.
Parents of autistic children became well-organized,
and the government
recognizes that having to care for an autistic kid at home takes a worker
out of much or all productive employment.
(And it does -- Pediatrics 129: 617, 2012).
Now America pays ninety billion dollars per year for autism treatment; this is likely
to increase substantially especially as extremely labor-intensive treatments become entitlements
for desperate families.
In 2010, Missouri passed an insurance mandate for intensive treatment
("applied behavior analysis")
for every autistic kid of $40,000 per year through age 18 (i.e., four or five times the
cost of an Ivy Leage or medical education); the most recent studies showed no
advantage of a highly-paid therapist over supervised parents giving the intensive behavioral
treatments (Autism 13: 613, 2009) or which model worked better ("applied behavior analysis" vs. "TEACCH":
J. Autism. Dev. Dis. 40: 74, 2010), or whether spending just an hour a week
works just as well as the intensive, super-expensive stuff (Autism 13: 93, 2009).
The two decades of work on "applied behavior analysis" suggests that it does help
some in a significant minority of kids
but that there's a lack of scientific rigor and even controls in the studies (Behav. Mod. 31: 682, 2007).
THE paper on early intervention
(Am. J. Ment. Retard. 110: 417, 2005) had no non-treatment control,
found that time with "autism professionals" was no better than time with trained parents,
found that the children who were less sick to begin with did better,
and merely suggests that some children diagnosed with early autism
grow out of it.
The Australian meta-analysis found "inadequate evidence" that intensive interventions are
better than "standard care" and bewailed the amount of grotesque
junk-science (J. Ped. 154:
338, 2009).
One recent study that compared two groups (but no non-tretment group; J. Aut. Dev. Dis. 37: 1815, 2007)
decided there was a slight advantage to treating the kid for 30 hr/week rather than 15 hr/week
but "there was no evidence of recovery from autism" -- despite the hoopla you'll hear
showcasing "productive adults who were saved from autism by early intensive interventions."
"Parent-mediated communication-focused treatment"'s own developers
do a controlled study and decide they can't recommend it except to help
parents reach their child (Lancet 375: 2152, 2010.)
By contrast, the "early-start Denver model"'s non-blinded but
controlled study (run by
the "Autism Speaks" people, who are unabashed "advocates" and do media
ads and solicit money directly from the public -- "Autism affects 1 in 110 children") claims some
success for a hugely labor-intensive and extremely profitable "applied behavior analysis" program
requiring early
diagnosis (Pediatrics 125: e17, 2010). This is now hugely politicized,
with a recommendation from the American Academy of Pediatrics
that all toddlers be "screened for autism"
at 18 and 24 months -- from my reading, this is NOT standard of care at this time
and widely considered a terrible idea.
It is possible that some children, and perhaps society, will benefit.
Right now, there's talk of 20% of kids benefitting measurably
from intensive intervention (NEJM 365: 173, 2011), the rest being dismal failures.
There will also be a huge number of false-positives on the diagnostic
instrument (many of the questions
would get a "yes" from many different mentally-handicapped and slow-to-develop kids).
The popular "Modified
Checklist for Autism in Toddlers" involves
twenty-three yes-no questions
including "Does your child walk?" and "Does your child understand what people say?",
and looks to me as if it would probably diagnose almost all retarded children as autistic.
And even using standard instruments, different centers vary tremendously when it comes to
who they diagnose as "autistic" (Arch. Gen. Psych. 69: 306, 2012).
The facts that both "real autism" (whatever that is) sometimes appears to remit spontaneously,
and that slow-to-talk and slow-to-interact children suddenly catch up
on their own, will generate
heartwarming "success stories" that will keep the money flowing to "autism treatment".
"Late talkers" are fairly common (BMJ 343: 5181, 2011) -- physics genius Richard Feynman did not speak until he was three,
and one of my lifetime friends, now an expert on microsatellites, did not speak
until he was four -- "I didn't have anything to say." Today, both would probably
be snapped up by the autism militants who would have made lots of money and claimed "success".
In mid-2011, Pediatrics 128: e211, 2011 recommended against routine autism screening
because there's no clear benefit, it takes a lot of the busy pediatrician's time
to screen a kid who seems normal,
and a faulty diagnosis is stigmatizing
for the child and financially ruinous for the family
(follow-up JAMA 306:
691, 2011).
Autism United
in particular is aware of false-positives in screening.
In their series using their instrument "to screen for autism and other
developmental delays", 10479 babies were screened and after the false-positives were
reclassified, only
32 got a diagnosis autism or autism-spectrum disorder -- much lower than the activist claims --
and some remitted without any intervention.
The treatments from mainstream medcine / Big Pharma basically don't work
(Pediatrics 127: e1312, 2011), and not surprisingly
the charlatans beneft from this.
"Defeat Autism Now" is the big-money alternative-medicine (chelation therapy,
hperbaric oxygen, secretin -- fails 7 of 7 real studies Pediatrics 127: e1322, 2011 -- , "removing toxins", anti-immunization activism, etc., etc.).
Since the outcomes are subjective, and families are given warmth, attention, and
someone to blame, you will hear many anecdotes of success.
There is also an autism-pride movement ("pride in neurodiversity", by analogy
with the gay pride movement), etc., etc.
We have a natural controlled experiment going on now... In the USA, as much as a quarter of a
public school district's costs may come off-the-top for "applied behavior analysis"
of a few autistic kids, a family with an autistic kid will be ruined
financially, and the lifetime cost of a patient with autism was estimated by the
Wall Street Journal (2010) to be 3.8 million dollars. By contrast, in China,
both society and families spend very little on children who will not be productive
(Res. Dev. Dis. 32: 306, 2011). In twenty years, we will see whether our
interventions have helped.
In April 2011, with "autism therapy" 40 hours per week times $100 per hour
being the recommendation.
a major review pointed out the (already glaring)
lack of scientific rigor in studies supposedly showing effectiveness (only 2 randomized controlled
studies; even in the case series studies, only a minority of kids respond at all,
the improvements are subjective, there's wishful-thinking,
the miracle-stories are anecdotal, and the
illness can remit by itself): J. Ped. 127: 1303, 2011 (it ends with
a political-correctness disclaimer, of course).
* In the 1990's, a technique
called "facilitated communication" was developed, in which the operator used the child's hand as the
planchette of a Ouija board. Even if the child had never communicated or seemed to understand
language, the hand would spell out elaborate stories. If the child was shown one picture and the
(unknowing) operator was shown a different picture, and the child was then asked what the picture
showed, the "child" would describe only what the operator saw (Ment. Retard. 31: 49, 1993
and many, many more).
Gee whiz! The first commentators (1987, also J. Aut. & D.D. 21: 561, 1991) in the refereed literature
knew that "facilitated communication" was bunk, but supported it because it would make the public believe that autistic kids,
kids with cerebral palsy, and so forth were more like ordinary folks. In other words, politics and
propaganda are more important than truth. As you might expect, the "children" often produced
stories of elaborate secret sexual abuse, using the vocabulary of sleaze-pornography. Even after the
above-referenced article was published, at least one parent in Kansas was sent to prison entirely on
this evidence. The literature contains some accounts (notably by a group at SUNY; Arch. Ped. Ad. Med. 148: 1282, 1994) in which "the
child's story was proven to be true" by the confession of the accused (no good physical evidence
though); however, nowadays it is commonplace for a person accused of a sex crime, often on no
real evidence, to be offered leniency in exchange for a confession ("admit you did it and accept
counselling, or we'll send you to prison for life"). In 1994, "facilitated communication" (the subject
of a media "miracles of healing" hype in the early 1990's) got massive negative TV coverage (for example,
PBS, which
finished particular folly off). Freeing several dozen imprisoned people, all convicted of child
molesting solely on this evidence, took years even after the technique was
discredited. I am not making this up.
How this crock happened:
Child Abuse & Neglect 22: 1027, 1998 ("Its proponents' resistance
to allowing the technique's validation relying on the paradigm of normal
science has resulted in its broad dissemination without support", i.e.,
all this talk about "Thomas Kuhn paradigm shifts", "postmodernism", and so forth ruins
the lives of innocent people).
* The whole MMR-vaccine-and-autism
scare resulted from a study in Lancet with obvious selection bias;
the kids had supposedly been brought forward by parents who believed the MMR vaccine
had caused their autism. Lancet 351:637, 1998 also includes some
stuff on supposed intestinal pathology; when I read the article, I noticed
at once that the only "consistent"
lesions are normal findings (the authors claimed that groups of eosinophils
in the ileum are abnormal even though everybody's got them) and big lymph nodes with big germinal centers
(incredibly, they made a deal out of tingible body macrophages here,
everybody's got them too;
no controls of course).
During Wakefield's trial which resulted in his losing his license to practice
medicine, and public disgrace, it emerged that all these biopsies were read as normal
or near-normal, and that Wakefield's committee had changed them to "nonspecific colitis."
Was Wakefield right to fast-report a possible health hazard?
Right to falsify pathology reports and patient histories to build a case?
Wrong to rush to publication with no proper controls? To alter his data to make it
appear that there is a temporal relationship between MMR injection and sudden-onset
"regressive" autism. Reasonable people
will differ -- but he is ruined as a scientist and physician.
A paper from the Wakefield group
with PCR's purporting to show measles * Update: In June 2006, a media claim was made that a Dr. Arthur Krisgman,
pediatric gastroenterologist at NYU Med, and
a Dr. Stephen Walker of
Wake Forest University med school (where I did a year of training)
had replicated Wakefield's findings.
From the media reports,
all we have is recovery of vaccine-strain measles from a group of children,
without controls. We look forward to publication, peer-reviewed or not.
This is a very important question, and as I've said above
there may indeed be something real, despite all the politics, lawyering,
and emotion. Brain diseases that are reflected only in behavior
are the hardest of all diseases to study.
And no one questions the devastating impact and gravity of the question.
It would please me very much if an important contribution were to come
from the school where I trained. Stay tuned.
* Update: Formerly portrayed in the popular press as a "persecuted genius",
coverage of Wakefield has now become very hostile. Now he is a corrupt, mendacious charlatan
wilfully causing the deaths of children (review of media coverage
BMJ 336: 479 & 850, 2008). Although the
world has plenty of rotten people, I think perhaps
Wakefield is a man who perhaps saw faces in the clouds
and tried to do a good thing.
Knowing people as I do, I suspect the truth is closer to "the road to ____ is paved with
good intentions."
I've seen nothing further on the real-science front.![]() virus in the gut lymphoid tissue
of autistc children, but not controls (Mol. Path. 55: 84, 2002)
remains unreproduced by any other group, and curiously the group itself
admitted later that its own data had been corrupted (Mol. Path. 56:
248, 2003).
In Feb. 2004, the Lancet apologized for publishing the 1998 paper
and revealed that
Dr. Wakefield, the principal author,
was actually already being paid megabucks by lawyers hoping to sue
over immunizations.
Over the years, the parents of children in the study have come forward
saying that Wakefield falsified the histories (BMJ 342: c5347, 2011;
click here.
For those who are curious about "autisic enterocolitis", I recommend
the paper in Histopathology 50: 371, 2007, which reviews the problems
with the work, almost all of which has come from one group; just as I did
when I read the article in Lancet over a decade ago, they point out that
the original work called normal findings abnormal and weren't properly controlled;
they suggest that the hyperplasia is the result of the constipation seen
in autism, just as is seen in chronic constipation from other causes.
More about how this particular strangeness happened: West. J. Med. 174:
87, 2001. Dr. Wakefield, who still
holds out that he was right, admits that he's most impressed
with anecdotal evidence, and perhaps he's actually seeing an ultra-rare
phenomenon hidden in statistics (I think he could be right):
Br. Med. J. 324: 386, 2002. But his conduct ruined and disgraced
him publicly.
One of my cyberbuddies, a Ph.D. bioscientist who had a child with autism, is
confident of Wakefield's essential integrity, other professional
people have also written to me defending his genuineness and decency,
and at least early-on, Wakefield appeared to me to
be perhaps someone who thought he had discovered something
but presented his case poorly and without understanding
normal histology.
virus in the gut lymphoid tissue
of autistc children, but not controls (Mol. Path. 55: 84, 2002)
remains unreproduced by any other group, and curiously the group itself
admitted later that its own data had been corrupted (Mol. Path. 56:
248, 2003).
In Feb. 2004, the Lancet apologized for publishing the 1998 paper
and revealed that
Dr. Wakefield, the principal author,
was actually already being paid megabucks by lawyers hoping to sue
over immunizations.
Over the years, the parents of children in the study have come forward
saying that Wakefield falsified the histories (BMJ 342: c5347, 2011;
click here.
For those who are curious about "autisic enterocolitis", I recommend
the paper in Histopathology 50: 371, 2007, which reviews the problems
with the work, almost all of which has come from one group; just as I did
when I read the article in Lancet over a decade ago, they point out that
the original work called normal findings abnormal and weren't properly controlled;
they suggest that the hyperplasia is the result of the constipation seen
in autism, just as is seen in chronic constipation from other causes.
More about how this particular strangeness happened: West. J. Med. 174:
87, 2001. Dr. Wakefield, who still
holds out that he was right, admits that he's most impressed
with anecdotal evidence, and perhaps he's actually seeing an ultra-rare
phenomenon hidden in statistics (I think he could be right):
Br. Med. J. 324: 386, 2002. But his conduct ruined and disgraced
him publicly.
One of my cyberbuddies, a Ph.D. bioscientist who had a child with autism, is
confident of Wakefield's essential integrity, other professional
people have also written to me defending his genuineness and decency,
and at least early-on, Wakefield appeared to me to
be perhaps someone who thought he had discovered something
but presented his case poorly and without understanding
normal histology.
Advocacy groups, including the big-money "Autism Speaks", are bitterly divided over whether vaccines cause the disease, and whether to spend the donation you are invited to make at the movie theater "researching" this question. This helps no one.
![]() Ileal Lymphoid Hyperplasia
Ileal Lymphoid Hyperplasia
How the Wakefield
MMR business got going
Anyway, in children reported to have autism following MMR or other immunization, there's no dose-response relationship, and no relationship to whether a batch of whatever pediatric vaccine actually contained thimerosal (ethylmercury, the supposed toxin): JAMA 290: 1763, 2003. A huge case-controlled in Britain shows no link: Lancet 364: 963, 2004. Because of public concerns, thimerosal hasn't been in US vaccines, except for a few 'flu vaccines, since 2001, and there's been no corresponding decrease in autism (Nat. Med. 15: 119, 2009). When vaccines cannot always be kept refrigerated, as in much of the developing world, there has to be thimerosal.
* The vaccines-and-autism story took a further bizarre twist when the Bush administration granted citizen (i.e., activist) oversight of vaccine safety research (NEJM 358: 2089, 2008). The index case was Hannah Poling, a Hopkins neurology resident's daughter who appeared normal at birth, but had a genetic mitochondriopathy that causes encephalitis and brain damage after common childhood infections. When this happened to the child, the family "was sure" it was the vaccines causing autism. The Bush administration decided to compensate the girl in April 2008. Stay tuned.
ASPERGER'S ("high functioning autism") is a relatively newly-described "disease", supposedly affecting mostly boys, running in families. Asperger's boys tend to be of normal or high intelligence, strongly focused on single topics (for example, math, chess, computers, a musical instrument, train schedules, pathology, skydiving, flattop haircuts, etc., etc.), are physically clumsy, find other people baffling, but don't commit crimes (well usually, the ones who do are refractory to treatment: Med. Sci. Law. 42: 237, 2002). Speech is rapid and lacks intonation. As kids, they are "little professors." After many social failures during adolescent and young adult life, they tend to withdraw and become odd loners. As teens and adults, they have to work hard to learn to use and read body language and to relate to others. Asperger's seems to be real, and I predict that its study will show something about the wiring of personality. Adults with Asperger's have greatly reduced 5-HT2A receptor density (Brain 125: 1594, 2002), and differences in brain anatomy especially in the frontostriatal connections (Brain 125: 1594, 2002). Properly managed, Asperger's offers a set of unique plusses both for the individual and -- if the interests are useful -- for society.
| Of all the patient-care specialties, I am most intrigued by psychiatry. Many other pathologists share my fascination with the life of the mind. |  |
Right now, the study of the very-common OBSESSIVE-COMPULSIVE DISORDERS is a major topic in psychiatry; watch this elucidate different types of serotoninergic synapses (Mayo Clin. Proc. 67: 266, 1992; Postgrad. Med. 91: 171, 1992; Arch. Gen. Psych. 49: 21, 1992; subtle cues to basal ganglia dysfunction Brain 114: 2191 & 2203, 1991; Arch. Gen. Psych. 47: 27, 1990, notably such stuff as visuospatial coordination; this is no surprise because Sydenham chorea produces obsessions and compulsions: Am. J. Psych. 146: 246, 1989; caudate on PET scan display before and after therapy: Arch. Gen. Psych. 49: 681, 1992). For unwanted intrusive thoughts about a past or present problem, set the business down in a cohesive form on paper. When obsessive-compulsive appears suddenly, you'll probably find damage on scan somewhere in the cortex or basal ganglia (Neurology 47: 353, 1996). Moderate catechol O-methyl transferase deficiency and obsessive-compulsive: Proc. Nat. Acad. Sci. 94: 4572, 1997. Psychological tests and scans of patients and family members (who tend to have similar, milder changes): Brain 130: 3223, 2007. Tourette's is polygenic; a locus at L-histidine carboxulase gene: NEJM 362: 1901, 2010. Sociopathy / antisocial personality ("lacking the part of the brain that feels empathy and remorse") may have an organic component, but it's elusive (Arch. Gen. Psych. 57: 128, 2000).
| BIPOLAR DISORDER (when it's real, and not just common moodiness) is obviously genetic with several distinct syndromes and likely loci (Am. J. Psych. 160: 999, 2003; Arch. Gen. Psych. 60: 497, 2003). Most cases seem to be polygenic, and important genes are now being discovered, with well-established loci at CACNA1C, ODZ4 and NCAN (Lancet 381: 1654, 2013. I'm not the only physician who think that the drug companies have something to do with the greatly increased frequency with which the diagnosis "bipolar" is being made recently. One kind of UNIPOLAR DEPRESSION links nicely to the serotonin transport gene (Lancet 347: 731, 1996 -- I hope no one is surprised). | 
|
ATTENTION-DEFICIT DISORDER, with difficulty focusing (even on play), is wired in the caudate and its connections to the frontal lobe (Am. J. Psych. 151: 1791, 1994; update from neuroimaging is impressive: Lancet 362: 1699, 2003). The mouse model is the knockout mouse lacking dopamine transporter: Science 283: 397, 1999.
The big news in DYSLEXIA in 1996 was the discovery that if you help these kids distinguish different phonemes early, they do much better (Br. Med. J. 313: 1096, 1996, Child. Dev. 65: 41, 1994). As I predicted in the 1980's, the US fad to forbid the teaching of phonics resulted in a lot more cases of dyslexia (Psych. Sci. 2(2S): 31, 2001, big review, go figure); sadly, it took neuroscientists rather than people possessed of simple common sense to end this fiasco. Gene candidates for dyslexia: Lancet 379: 1997, 2012.
Whatever else we are, humankind is the talking animal. Almost everybody has the same FOXP2 allele, which indicates it swept through the human population rather recently. This includes the Neanderthals (Curr. Bio. 17:1, 2007); any other allele causes severe deficits in speech and language (Nature 413: 519, 2001). Many people are relatively non-verbal (speaking, reading, understanding) despite otherwise normal intellectual function; there's now a few known mutations that cause recipients to be unable to use suffixes or complex grammar. Some have a lot of trouble not only being understood, but moving their faces (Nat. Genet. 18: 168, 1998 -- discovery of the SPCH1 locus, where FOXP2 is located). As a college student in the late 1960's when B.F.Skinner was dogma ("Environment is everything"), I say I'm getting the last laugh.
PANIC ATTACKS have long been familiar to physicians. Hard findings include an exaggerated autonomic and respiratory response to infusions of lactic acid, and a rat model caused by chronic inhibition of GABA synthesis and the same vulnerability to lactic acid. The new work shows elevated levels of hypocretin / orexin in the CSF in patients with panic attacks, and that blocking the ORX-1 receptor prevents the panic attacks (Nat. Med. 16: 111, 2010).
We await effective therapy for BORDERLINE PERSONALITY ("I hate you, don't leave me!" and more), and I wonder whether it's hard-wired or simply a lack of living skills (which are hard to teach -- and they won't learn if you tolerate their behavior). When talking to a borderline, say "I feel" rather than "you...", and avoid getting entrapped by them.
You will hear plenty of GLOSSOLALIA (i.e., people who believe they are speaking a language they themselves do not understand) among people who are clearly mentally ill, the majority being psychotic; review J. For. Sci. 47: 305, 2002. Whether it is ever really of supernatural/paranormal origin is something you'll need to decide for yourself.
SOMATIZATION DISORDER ("somatoform disorder" JAMA 278: 673, 1997) is still considered "all in your mind" -- I believe this is wrong. The typical patient is a low-achieving young adult with anxiety, depression, and personality problems ("borderline", etc.) However, these folks also have lots of aches, pains, and symptoms that cause substantial disability. This is a patient type well-known across cultures (Am. J. Psych. 154: 989, 1997). I predict (2007) that it will be found to have a strong organic basis and eventually an effective organic therapy. (Uh, doc, you did rule out everything else, right?)
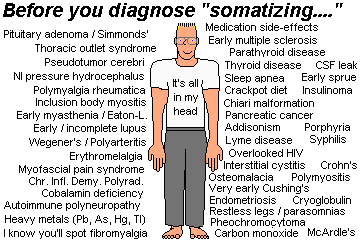
* Also watch KLEINE-LEVIN SYNDROME (spells of hypersomnia and polyphagia with bizarre behavior), or "sleep-related eating disorder". This in turn may or may not be related to compulsive nighttime icebox-raiding.
SEASONAL AFFECTIVE DISORDER: Arch. Gen. Psych. 41: 72, 1984 (said it all; wavelength Am. J. Psych. 148: 509, 1992; the atypical antidepressant agomelatine, which disrupts circadian rhythms, seems to help: Psychopharmacology 190: 575, 2007; I was surprised that melatonin turned out to be no beter than placebo Neuropsychopharmacology 30: 1345, 2005), though some folks do use it Chronobiol. Int. 23: 403, 2006).
NARCOLEPSY is real (Mayo Clin. Proc. 65: 991, 1990) and affects about 1 person in 5000; patients must have HLA-DR2 / DQ1 (Lancet 341: 406, 1993). They fall asleep without being able to resist, and also drop over suddenly like a rag doll from time to time without falling asleep ("cataplexy"). The brain lacks the neurotransmitter hypocretin, though this is usually not the locus (Nat. Med. 6: 991, 2000; update and additional complexity Lancet 363: 1199, 2004). Most often, the neurons that use hypocretin in the hypothalamus are destroyed (by autoimmunity, we now know): Lancet 369: 499, 2007; Brain 133: 1300, 2010.
THE TRANSSEXUAL BRAIN: Ordinary men have huge, and ordinary women have tiny, central divisions of the bed nuclei of the stria terminalis in the hypothalamus (BSTc). Among several male transsexuals (gender-dysphorics, "I'm a woman trapped in a man's body!!"), gay or straight, every one had a tiny BSTc nucleus (Nature 378: 68, 1995). More recent work confirms this even more impressively: J. Clin. End. Metab. 85: 2034, 2000. Despite the politics, some patients find their being unhappy with their sex organs disappears on low doses of medication (Aus. NZ. J. Psych. 30: 422, 1996).
HYPERSEXUALITY seems to be in the wiring (Can. J. Psych. 46: 26, 2001), so it's not surprising that the 1990's push to define "sexual addiction" as an entity to be twelve-stepped was a total failure (Clin. Psych. Rev. 18: 367, 1998). By contrast, the common PARAPHILIAS seem to be acting-out (as common sense would suggest), either a way of dealing with your hatreds or simply avoiding the problems of being "normal". Despite the greater tolerance of (and even promotion of) "minority sexual practices" among consenting adults, these people tend to have overall poor interpersonal skills. If they find real friendship in the "alternative" community, it seems to me it's a good thing, but not the best life could offer.
POST-TRAUMATIC STRESS DISORDER is nothing new (Sophocles' "Ajax" -- Sophocles was also a general in the army --; "Skipper Ireson's Ride", shell-shocked WWI veterans), and is serious and real, but is now highly politicized. It is most severe in torture survivors, but any brush with death or bad mistreatment (rape, child abuse) can leave a person jumpy, sleeping poorly, and suffering from flashbacks. Two accounts from physicians appear in BMJ Dec. 2, 2000. One found a deeper appreciation for how delicate and uncertain life is, and spirituality became far more important in his life. Not surprisingly, the policemen with PTSD are the ones whose "worst moment as a cop" involved seeing their own lives in danger (JNMD 194: 591, 2006). The volume of the hippocampus is lower in PTSD patients whose trauma took place in adult life (J. Clin. Psych. 62(S-17): 47, 2001, others), but not when the abuse happened in childhood (Biol. Psych. 50:305, 2001). We don't know whether this identifies people more at risk for PTSD after trauma, or whether this is due to beatings sustained to the head, or whether it is an effect of torture. A prospective study that might have helped didn't get results (Am. J. Psych. 158: 1248, 2001). There are glucocorticoid receptors in the hippocampus, and in some models, glucocorticoid excess itself (Cushing's in humans, mice given high doses) causes atrophy of the hippocampus via glutamate excitotoxicity (Arch. Gen. Psych. 57: 925, 2000; Biol. Psych. 45: 797, 1999). People who have long-term severe depression also have marked atrophy of the hippocampus (Proc. Nat. Acad. Sci. 100: 1387, 2003); interestingly, the volume of the hippocampus is apparently normal at the beginning of these patients' illnesses; another report finds normal volumes but altered shape (Am. J. Psych. 160: 83, 2003). In very severe depression, there's extensive loss of synapses and cells in the prefrontal cortex, and a gene profile to match in a rat model(Nat. Med. 18: 1413, 2012). You'll have to decide for yourself about just how prevalent post-traumatic stress disorder is in people whose "stress" seems only part of normal life; lawyers are now alleging PTSD after fender-benders, hearing off-color jokes, etc. (Science 301: 465, 2003). Today there is a strong backlash against "the medicalization of distress" (Lancet 369: 139, 2007): "There is value in focusing on adaptive coping during and after traumas. Striking a balance between a focus on heroism and resiliance versus victimhood and pathological change is a crucial and constant issue after trauma for both clinicians and society." Nowadays, especially after trauma or before entering dangerous situations, psychiatrists focus on resilience training, learning to be a hero, to survive by your own effort and toughness and find meaning in doing this. In the Congo war zones, where women in particular experience horrible sexual abuse and violence, getting groups together to talk seems to be a big help (NEJM 368: 2182, 2013). To be a survivor rather than a victim, it helps to have a supportive family and/or friend-making skills, to find some positive meaning in the unfortunate event, to have some sort of spirituality, to be good at solving problems, to believe you actually can manage your feelings, to be willing to talk, and to seek out opportunities to help others. "Victimhood" ("external locus of control"; "learned helplessness") instead may make you money in court / disability, get you an identity as a victim, and get pitied, but it leaves you an emotional crippple.
Must reading (when you have time!): A chilling article entitled "Violence: The Neurological Contribution"; Arch. Neurol. 49: 595, 1992 (it is simplistic to ignore either neurology or sociology). Mice without nitric oxide synthetase are hypersexual and hyperaggressive (Nature 378: 336, 1995).
One current big fad in psychiatry is "debriefing", i.e., they bring a psychiatrist to talk to you after any really bad experience, loads of "counsellors" after a natural or man-made disaster, in the belief that this expensive intervention prevents long term psychopathology; I can't see why it should, and now it's pretty clear that it doesn't work (Br. Med. J. 310: 1479, 1995). Curious exceptions, at least in Britain, home of the stiff-upper-lip: Br. J. Psych. 169: 405, 1996 notes the contrast between the way the system totally ignores kids who've seen their loved ones killed in car wrecks with the flood of "counsellors" who descended on Dunblane in 1996.
| * NOT TESTABLE, BUT WORTH YOUR ATTENTION: The never-ending series of old and new health-and-disease crazes are within the proper scope of any introductory study of pathology. Thankfully, the "repressed memories" business is now history, though thousands of lives were ruined. The craze began in 1985, and ended in 1999. I first mentioned the epidemic in class in 1987, and it proved to be as I described. Any doubts I had were dispelled by Psychoth. Psychosom. 57: 152, 1992 (among 100 kids who saw Dad kill Mom, every one of them remembered it in detail). For a history of this epidemic of iatrogenic disease, see J. Nerv. Ment. Dis. 192: 525, 2004. |  |
* Probably the worst feature of this and the several other phony-child-abuse fiascoes was that they tended to discredit stories of child abuse that are really true, and to transform concern over child abuse into a preoccupation of the right-wing and left-wing lunatic fringes. As usual, the real losers are the children. Litigation (especially "Ramona v. Ramona" in California) has redefined a therapist's duty to third parties, and the "therapists" are being sued like they should be. Medilegal articles: Med. Sci. Law. 39: 112, 1999, Am. J. Psych. 156: 749, 1999; NZ Med. J. 111: 225, 1998; Comp. Psych. 39: 338, 1998; Psych. Serv. 52: 27, 2001. Perhaps the turning point came when Geraldo reversed himself on "enhanced memories" in 1995, declaring it to be "cr_p". In 1999 I was pleased to meet an attorney who told me that he "makes a good living" in a practice devoted almost entirely to suing these therapists, who he tells me in his part of the country are mostly "social conservatives."
-- Cervantes, "Don Quixote"
-- Erich Fromm
Death: Uh-uh. It's always been like this. You probably just don't get out enough. -- Neil Gaiman, "Death: The High Cost of Living"
-- Brenda Starr, Reporter
-- Goethe
-- French wine-maker's proverb The different sorts of madness are innumerable. -- Avicenna You deal with the madmen. All men are mad in some way or other; and inasmuch as you deal discreetly with your madmen, so deal with God's madmen, too -- the rest of the world. -- Dr. Abraham Van Helsing (pathologist) to Dr. John Seward (psychiatrist), in Dracula (Bram Stoker) Pluck from the memory a rooted sorrow, Raze out the written troubles of the brain, And with some sweet oblivious antidote Cleanse the stuffed bosom of that perilous stuff Which weighs upon the heart?
DOCTOR: Therein the patient
|  |
SANE PSYCHIATRY FOR THE PRIMARY-CARE PHYSICIAN: A lot of the general practice of medicine is psychiatry. Here's how to be a good part-time psychiatrist most of the time. You get more information by asking open-ended questions and inviting the person to talk, but sooner or later you'll need to have things that are worthwhile to say, yourself. You'll need to know how to tell people things that they don't want to hear in a nice way that will not make them stop trying to change. If you actually want to help people with emotional and behavioral problems, focus on reminding them of what they can do, what's still intact (bad for any secondary gains, but good medicine), living in the present, and so forth. Today's psychiatrists give them "behavioral homework", which is simply common sense. Depression etc., both result from negative life events, and causes negative life events (J. Nerv. Ment. Dis. 185: 145, 1997). Cognative-behavior therapy actually changes the PET scan, but in complementary ways to what prozac does (Arch. Gen. Psych. 61: 34, 2003). Your fixed attitudes, beliefs, and behaviors can change if you work on implementing the things you've talked about. Keep reminding people of how their screwy behavior and unrealistic attitudes ("faulty core beliefs") hurt them and those around them. Today, the scientifically-minded mental-health community seems to think that "adverse life events in childhood" are not by themselves the cause of mental illness or personality disorders (J. Pers. Disorder. 11: 34, 1997; lots more), though of course growing up in a home full of crazy people will teach behaviors that need to change in adult life. Keep watch on one's own thoughts and try to keep them from going in directions that aren't wholesome ("Zen", if you like -- though every great world-faith gives this good counsel.) Help them learn living and coping skills (i.e., explain to them how to do stuff that the rest of us may take for granted) rather than jabbering on about ("working through") their past traumas and present follies. Spending too much time figuring out exactly caused the problem can enable ongoing, harmful behaviors. Everybody resists adopting new behaviors, and troubled people even more so. Get them to confront their fears as boldly as they can. Know your issues and move forward, with guidance. And don't call this "empowerment", the 1990's grandiose-trendy word; troubled people already have the power to do plenty. To alter your feelings, alter your behavior first -- "fake it 'till you make it." Be strong. Don't do that any more. Don't run back to things that are childish. If you keep doing that, all you'll get is _____. Find pleasure and meaning in some other way.
People growing up in crazy environments acquire behaviors and attitudes that enable their emotional (and even physical) survival there, but that serve them badly in the larger world. Whatever the circumstances, one's emotional ties to one's origins are strong and these people resist changing their self-defeating behaviors. Honor their struggles to survive even as you help them leave this behind. You can help people realize why this is and that they don't need to be locked into it forever.
You may disagree with what a crazy person says, but don't argue; people who are not psychotic will come around as they realize that their thinking is no longer helpful and that they can change their behavior to deal with a world that's saner than their own childhood homes. Don't expect most people ever to understand all that may be obvious to you. But most people can learn new skills. Learn how to use a modest selection of the psychopharmaceutical agents, and use them sensibly; if a medication isn't working in two months, change it or just drop it. Remember the basics: Neurotics are troubled (lots of things upset them), personality-disorder folks are troublesome (they will upset you), and schizophrenia and most of the bad-affect states respond to medication but not to talking. Non-psychotic people with ideas that they recognize as not making sense can usually figure out, with your help, what the obsession stands for, and try to get what they really want by some more realistic route. Marriage counselling is largely the delicate art of getting the two people to listen to, and try to please, one another on a daily basis, and to extend basic human kindness across gender-differences (i.e., a man and a woman can learn to be nice to each other even though they cannot possibly understand each other; the other person isn't acting that way just to be hateful; guide and teach rather than criticize; "the relationship is more important than being right", and so forth). I'm told it's helpful to make an effort to have sex often even if neither partner is interested. When a relationship fails, remind the person of the ways in which the former beloved / the rival are doing the person a favor. There is no physician-patient confidentiality when a human life is in danger. Please remember how unreliable memory is. Especially in the ICU on medication, people may come out "remembering" nightmares that never happened (AJRCCM 177: 976, 2008).
In my lifetime as a student of medicine, I've never seen a disease that was considered "organic" in the 1950's prove to be "psychosomatic", but I've seen the opposite many times (hypertension, asthma, stomach ulcer, inflammatory bowel disease, atopic eczema, blepharospasm, and torticollis are only the beginning; there are even genetic animal models for folks like your instructor who strongly prefer to keep our fingernails super-short). And a good psychiatrist, seeing mental illness as arising from brain, appreciates both the cognitive-insight and the pharmacological therapies (Science 275: 1586, 1997).
INTERPERSONAL THERAPY, a common-sense "innovation", was the 1990's term for psychotherapy for the financially-responsible era, where things have to be cheap and have to work. The focus was on improving people's abilities to relate to others, no matter what the circumstances. (1) Deal with any grief and loss issues, emphasizing what's still intact; (2) Solve interpersonal role disparities (i.e., conflicts over who is supposed to do what); (3) Deal with role transitions (that was then, this is now, focus on the future rather than the past); (4) Teach them interpersonal skills and make them practice between sessions. You can't make somebody love you. Talk about the other person's interests, and be a diplomat. Relationships are more important than being right. If you want a relationship to be successful, try to figure out what the other person wants, and then try to provide it. They also (5) learn to watch for goofy "I can't because..." thinking, and other unhelpful thoughts, that prevent them from doing the things they need or want to do, and having them report each week. It turns out that simply letting your patients learn and practice these skills from an internet site is more effective than talking to them in a nurturing and supportive way: Br. Med. J. 328: 265, 2004. The sites were Blue Pages and Mood Gym. Here is another site I've found helpful (follow the links). Update for online CBT: BMJ 344: e2598, 2012.
COGNITIVE-BEHAVIORAL THERAPY is now the model for psychotherapy for people capable of insight. The focus is on education, facing fears, and learning skills.
NON-EVIDENCE-BASED PSYCHOTHERAPY (often not even physician-supervised) remains one of the great causes of ill-health in the Western world. Providers are usually well-intentioned and it's a good way of making a living -- essentially no knowledge or real education is required. The "repressed memories" fraud has ruined tens of thousands of families; it's still widespread. The "facilitated communication" fraud sent totally innocent persons to prison, as well as giving false hope to families of the extremely sick. Generally, the "therapists" focus on the past rather than the present, offer pity and ideology rather than the kick-in-the-butt we all need from time to time, and reinforce their victims' sense of helplessness, entitlement and/or victimhood -- which keeps them coming back. Call me unspiritual if you want -- you'll see the tremendous harm this does when you're in practice. Whenever anybody says, "Therapy taught me to blame...." or "After years of talking about my past with my therapist....", be aware you're dealing with someone who has been done a grave disservice.
* Physicians respect the religious beliefs of each patient, as long as nobody's getting hurt in a big way; these beliefs are a good topic for discussion. If "religion is what deals with matters of ultimate concern", one need not believe or even care about the "supernatural / paranormal" for "faith to be important." Totally sane people often report experiences with the paranormal (whatever that is). When I was an intern, a group of 15 housestaffers at lunch got into a discussion of out-of-body experience, who among us had experienced it personally, and what you told the patients who came in all worried after experiencing it; we decided it was "normal but something we don't understand". Unlike many "spontaneous" out-of-body experiences, the one's I've read about from the experimental lab (for example NEJM 357: 1829, 2007) do not involve autoscopy or the ability to move one's frame of perception. And crazy people often report experiences with the paranormal (whatever that is; the crazies' experiences are much more diverse and atypical than the "normals"). No matter what your faith background, if you're interested in this sort of thing you may enjoy "The Interior Castle", by Teresa of Avila. She was a spunky, brilliant, non-dogmatic and often-hilarious writer from a Jewish-Muslim-Christian background. Her book, written for both cloistered and in-the-world folks, deals with trying to tell "the real thing" from dreams, hallucinations, big egos, fakery, spiritual evil, and mental illness.
DEMYELINATING DISEASES
|
|
MULTIPLE SCLEROSIS (J. Clin. Inv. 122: 1180, 2012) is a common, dread neurologic disease in which myelin is lost successively in many ("multiple") plaques throughout the white matter.
Although "MS" is clearly an autoimmune disease the exact pathology and pathophysiology have remained remarkably elusive. Older review Arch. Neuro. 58: 1975, 2001; further review, showing that it's still basically a mystery at the molecular level: Arch. Neuro. 63: 25, 2006.
There are about 400,000 MS patients in the USA and maybe 2.5 million worldwide. The onset is typically in young adult life. There's a strong Caucasian predominance and weak familial tendency and links to certain HLA antigens (Neurology 43: 548, 1993; Arch. Neurol. 50: 256, 1993). More interestingly, adults who spent their first 15 years entirely in the tropics are almost never affected; people born in the tropics who move to more temperate latitudes are at similarly increased risk. A link to vitamin D deficiency (common rickets, or a hereditary rare syndrome in which a person has a much greater need for the vitamin -- Arch. Neuro. 65: 809, 2008) are emerging as risk factors; getting plenty of sulight and vitamin D intake as supplements are somewhat protective (Neurology 62: 60, 2004) -- this is now a robust finding (Brain 133: 1869, 2010). What else sunlight may have to do with the illness remains mysterious.
In Europe, "Greens" and anti-immunization activists do not need any evidence to force major studies to be performed to investigate "pop" claims. It turns out that the HPV vaccine is not associated with an increased risk of multiple sclerosis: JAMA 313: 54, 2015.
Some familial MS links to the gene for myelin basic protein (Lancet 340: 987, 1992 Finland, Neurology 61: 520, 2003 other caucasians), an antigen that seems to be a principal target for immunity in MS. T-cells rearranged to attack myelin basic protein are abundant in MS lesions in humans, and rat T-cells bearing the same rearrangement cause experimental allergic encephalomyelitis in rats (both Nature 362: 68, 1993).
Although MS tends to run in families, usually these families have normal myelin basic protein genes (Lancet 341: 1179, 1993), and over the past decade it's been generally agreed that there are few or no "genes of large effect" involved in most MS cases (Brain 121: 1869, 1998; Brain 125: 150, 2002 -- "the Multiple Sclerosis Genetics Group" comes up with almost nothing).
In addition to the waxing and waning of the white matter lesions, it now appears that there is an ongoing, steady loss of neurons from the cortex (Neurology 68(S3): S-4, 2007). Watch for this to be targeted by new biological therapies. Further, demyelinization of the gray matter, long-overlooked, is often extensive and correlates with fatigue and cognitive problems (Arch. Neuro. 64 76, 2007; proposed mechanism NEJM 361: 1505, 2009).
Biopsy material from fresh MS plaques shows the oligodendroglial injury (not death) is the early injury in multiple sclerosis. They die at the center of plaques, and proliferate at the edges, and they can re-myelinate if they recover (Mayo Clin. Proc. 68: 627, 1993).
The vast majority of patients are
EBV-positive![]() ;
Epidemiology 11: 220, 2000; now JAMA 289: 1533, 2003;
molecular mimicry NEJM 349: 185, 2003; high EBNA-1 IgG titer as a teen,
an aberrant response, predicts
future MS risk JAMA 293: 2496, 2005 and Neurology 62: 2277, 2004; data
from stored sera Arch. Neuro. 63: 839, 2006; update Neurology 74: 1365, 2010).
Others occasionally still mentioned are
human
measles
;
Epidemiology 11: 220, 2000; now JAMA 289: 1533, 2003;
molecular mimicry NEJM 349: 185, 2003; high EBNA-1 IgG titer as a teen,
an aberrant response, predicts
future MS risk JAMA 293: 2496, 2005 and Neurology 62: 2277, 2004; data
from stored sera Arch. Neuro. 63: 839, 2006; update Neurology 74: 1365, 2010).
Others occasionally still mentioned are
human
measles![]() virus, herpes 6,
herpes 7, and canine distemper virus.
virus, herpes 6,
herpes 7, and canine distemper virus.
Support for the idea that Epstein-Barr virus![]() is a usual culprit comes from the finding that the vast majority of MS
patients are seropositive for this virus, usually at relatively high titer, and that
the mechanism of molecular mimicry between myelin and
EBV antigen may now be understood (NEJM above). However, PCR seldom shows
EBV RNA in active plaques (Brain 132: 3318, 2009; Neurology 74: 1127, 2010).
is a usual culprit comes from the finding that the vast majority of MS
patients are seropositive for this virus, usually at relatively high titer, and that
the mechanism of molecular mimicry between myelin and
EBV antigen may now be understood (NEJM above). However, PCR seldom shows
EBV RNA in active plaques (Brain 132: 3318, 2009; Neurology 74: 1127, 2010).
* HHV6 (roseola) is now being identified as replicating in active MS plaques of many (but not all) MS patients, but not in control brains. This is another bug that it's reasonable to think is ubiquitous in the tropics and less common in chilly regions. Since the main article (Science 278: 710, 1997), other groups have found HHV-6 nRNA (most recently Brain 128: 516, 2005). However, many MS patients have no sign of HHV6.
The mouse model uses (* Theiler's) virus, and mice that go on to get mouse-MS are those in which infection induces lasting expression of MHC-I antigens on brain cells: Mayo Clin. Proc. 67: 829, 1992.
* A claim from anti-immunization activists and tort layers about hepatitis B vaccine and other immunizations causing MS flopped: NEJM 344: 319 & 327, 2001. Predictably, the HPV vaccine was also alleged to cause multiple sclerosis -- again, not true (JAMA 313: 54, 2015.)
* Nitric oxide is produced in bulk in the acute lesions (confirmed Am. J. Path. 158: 2057, 2001), and nitric oxide scavengers almost totally prevent / treat one of the mouse models (Proc. Nat. Acad. Sci. 94: 2528, 1997). Further... the active species may be peroxinitrile, which is scavenged by uric acid (!), and large registries show no patient with both MS and gout (Proc. Nat. Acad. Sci. 95: 675, 1998). Follow-up with an animal model: Proc. Nat. Acad. Sci. 99: 16303, 2002. Definitely stay tuned.
Lesions form episodically in MS, contributing to its picture of exacerbations and remissions.
"Sclerosis" in this context means loss of myelin and oligodendroglia, sometimes preservation of axons and massive proliferation of astrocytes. The lesions are sharply-circumscribed, yellowish or grayish (pink if very active), firm areas. The can occur anyplace in the CNS; the favorite site is adjacent to the ventricles, often symmetrically.
* In a "mouse model", axonal loss seems important and at least one novel therapy addressing this is under study (J. Clin. Inv. 118: 1532, 2008). In humans: Nat. Med. 17: 495, 2011 (amazing electron micrographs).
Microscopically, demyelination begins around the blood vessels. During the active phase, the plaques are packed with T-helper and T-suppressor cells, and presumably there is some autoimmune component to the pathogenesis (providing the rationale for immunosuppression using ACTH).
There is some remyelinization (as you'd expect -- this is a disease with some resolution of acute neurologic defects), especially in the lesions below the cortex lesions and in early cases (Neurology 72: 1914, 2009).
* Future pathologists: In secondary progressive ("galloping") multiple sclerosis, you are likely to see clusters of B-cells in the meninges; these are suspected of damaging the underlying gray matter.
In the burned-out, chronic lesions, there are still oligodendroglia with processes wrapped around the axons, but they do not remyelinate the axons; the axons themselves appear abnormal, with thin and thick areas (NEJM 346: 165 & 199, 2002) and while axons are preserved, today's thinking is that they are damaged from the beginning.
* There are a few neuron cell bodies in subcortical white matter, mostly interneurons that regulate blood flow. In demyelinated areas, these neurons seem to proliferate. This is part of the ongoing mystery (Brain 131: 2366, 2008).
{01428} multiple sclerosis, myelin stain of white matter (note areas where the blue-staining myelin is
lost)
{31776} multiple sclerosis
{31779} multiple sclerosis
{31797} multiple sclerosis
{31994} multiple sclerosis
{00527} demyelination in the spinal cord
|
Pittsburgh Pathology Cases |
|
|
ACUTE HEMORRHAGIC LEUKOENCEPHALITIS ("acute necrotizing encephalitis", * "Hurt's disease"; considered today to be the hyperacute variant of acute disseminated encephalomyelitis, maybe -- both are believed triggered by structural homology between myelin basic proteins and an infectious agent) is a (fortunately rare) disease that tends to follow a minor viral respiratory infection (notably mycoplasma) by a few weeks. There is both perivenous loss of myelin (the small vessels themselves likely to be necrotic and axons preserved), and hemorrhage and necrosis throughout the white matter. There is a heavy, mixed inflammatory infiltrate (neutrophils, macrophages, and T_cells; unlike classic acute disseminated encephalomyelitis, which lacks neutrophils).
![]() Acute Hemorrhagic Leukoencephalopathy
Acute Hemorrhagic Leukoencephalopathy
Pittsburgh Illustrated Case
* There is a rare familial form;this suggests that there's a genetic predisposition in sporadic cases (Pediatrics 125: e693, 2010).
*The disease strikes down a young doctor: South. Med. J. 87: 851, 1994 (scary reading).
* Acute hemorrhagic leukoencephalitis after H1N1: Arch. Neuro. 67: 756, 2010.
The animal model for both disesaes is EXPERIMENTAL ALLERGIC ENCEPHALOMYELITIS, induced by injections of myelin basic protein; the disease can also be transmitted by T-cells specifically reactive for myelin basic protein Neurology 43: 1028, 1993.
LEUKOENCEPHALOPATHY FOLLOWING CANCER THERAPY is coming to be more widely recognized. Chemotherapy and radiation are both capable of doing serious or even fatal damage (Neurology 62: 451, 2004). The problem appears weeks to months after the therapy.
CENTRAL PONTINE MYELINOLYSIS represents demyelinization (with axon preservation) in the central pons. The histology resembles multiple sclerosis.
Central pontine myelinolysis can be quite extensive and render a person "locked in".
Once mysterious (or attributed to alcohol abuse), we now believe this usually represents an unfortunate result of too-rapid correction of severe hyponatremia (uh oh, Doc....) Puzzle THAT one out! The new name is OSMOTIC MYELINOLYSIS. I have seen this lesion three times in my autopsies; in each case, it was unexpected. (* This isn't the only possible cause: see J. Clin. Path. 44: 909, 1991). Review Mayo Clin. Proc. 76: 559, 2001 (replacing sodium "within recommended limits" doesn't guarantee safety). Picture NEJM 333: 1259, 1995. Of course other parts of the brain are likely to be involved as well (Br. J. Rad. 85: e87, 2012).
{31988} central pontine myelinolysis
OTHER METABOLIC DISEASES OF THE CNS
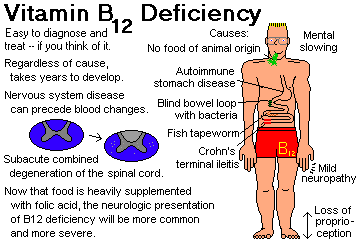
SUBACUTE COMBINED DEGENERATION OF THE CORD is a curious term for a curious lesion: destruction of the myelin and eventually axons of the posterior columns of the spinal cord caused by vitamin B12 deficiency.
Later, the brain and descending pathways are affected. This is a tragic disease to miss, since it's easy to administer the vitamin.
The neurologic damage can be permanent. There's sensory lass; ask also about burning pain in the feet.
Now that food is supplemented with folic acid, there's more of this clinically. (Why?)
Like it or not, a vegetarian (not even necessarily a vegan) who does not know EXACTLY what he/she is doing is likely to end up B12 deficient. By now, the myelopathy in these people is so well known that it's come to be called "vegetarian's myelopathy" (Int. Med. 45: 705, 2006). Moral high-ground or no, these people are endangering their health and the health of their families. The index case was a 14-year-old vegan who paralyzed herself (thankfully, treatment helped her): Clin. Ped. 40: 413, 2001; this is the tip of the iceberg.
Remember that people who don't take good care of themselves and eventually can't walk may have subacute combined degeneration of the cord -- and pay with their lives (AMFJP 30: 47, 2009.)
* Future pathologists: The same histologic and clinical picture may be seen in copper deficiency ("Are you taking a lot of zinc to prevent colds?") and in nitrous oxide abuse.
HASHIMOTO'S ENCEPHALOPATHY, seen in about 1% of patients with Hashimoto's thyroiditis, involves the white matter underneath the cortex. It is now clear that the pathology includes an immune-based lymphocytic vasculitis You treat it with thyroid replacement and glucocorticoids. Reviews: Neurology 49: 623, 1997. Neurology 61: 1124, 2003.
ALCOHOLISM probably isn't good for the brain all by itself. But the most famous sequelae (Wernicke-Korsakoff) are the result of thiamine deficiencies (Wernicke's from a prolonged fast: For. Sci. Int. 47: 17, 1990).
One-night drunkenness and compulsive problem drinking have no known morphologic counterparts.
* You'll learn in your "Psych" unit about brain-waves that are markers for not-learning-from-bad-experiences, etc., etc. Your lecturer, like possibly even some of you, had a few semi-bad experiences with alcohol as a college frosh. Your lecturer then said "To heck with this", and now rarely drinks. By contrast, the future problem drinker doesn't learn.
CEREBELLAR VERMAL DEGENERATION (better than "atrophy"; superior aspect is most heavily involved) is typical of chronic alcoholism ("superior vermal atrophy"), but is not entirely specific.
Does the "moderate drinker" really get more cortical atrophy in old age? Yes! -- Stroke 32: 1939, 2001. No! -- J. Neur. N. Psy. 71: 104, 2001. Definite maybe! -- Alc. Clin. Exp. Res. 22: 998, 1998.
{17659} superior vermal atrophy
|
![]() Superior (anterior) vermal atrophy
Superior (anterior) vermal atrophy
WebPath Photo
* MARCHIAFAVA-BIGNAMI DISEASE is a mysterious ailment, mostly affecting alcoholics and (less often) anorectics and the badly-neglected.
Nobody knows the cause. It's reported mostly from Europe, and used to be linked epidemiologically to Italian red wine. Perhaps an adulterant (arsenic?) was the cause.
Contrary to classic teaching, the disease is often reversible with good nutrition and cessation of drinking. Great photo NEJM 351: e10, 2004.
{31986} Marchiafava-Bignami
In suspected Wernicke-Korsakoff, look in the mammillary bodies and periventricular gray of the diencephalon for edema and/or bleeds (acute) and/or gliosis (old).
{31763} Wernicke's
{31985} Wernicke's
{31985} Wernicke's
|
|
|
Blood alcohol levels (gm/dL)....
0.050-0.10... happy 0.10-0.20... drunk 0.20-0.350... kisses mother-in-law, shoots best friend 0.350 & up... books say "coma & death" unless you're tolerant; police often find these levels in folks who are still driving |  |
METHYL ALCOHOL causes necrosis of the retinal cells (ganglion cells, rods, cones). In acute fatal cases, there is cytotoxic edema and necrosis of the entire brain. The putamen is especially hard-hit.
{31984} methyl alcohol poisoning. Not a pretty sight.
REYE'S SYNDROME brains show only cytotoxic edema and perhaps Alzheimer II glia.
CARBON MONOXIDE ENCEPHALOPATHY is often followed (in severe cases that survive for some months) by necrosis of the globus pallidus (less often, the hippocampus, Purkinje cells, and white matter).
{31751} carbon monoxide after-effects
{18751} carbon monoxide after-effects
{31742} carbon monoxide after-effects
* One of your lecturer's friends in medical school suffered this catastrophe after saving five people from a burning building. After awakening from several days of coma, he returned to medicine despite major difficulty walking and speaking.
KONZO results from poor people eating semi-poisonous cassava root (manihot / manioc) during food shortages (Lancet 339: 208, 1992; chilling reading). Though somtimes compared to ALS, it is actually an acute, epidemic, permanent, non-progressive disease caused by necrosis of the upper motor neurons that move the legs.
METHOTREXATE ENCEPHALOPATHY causes necrosis of the white matter. Look for mineralization of the axons.
ARSENIC POISONING produces petechiae throughout the deep brain substance.
{00206} fatal arsenic poisoning
{00209} fatal arsenic poisoning
ORGANIC MERCURY POISONING
MANGANESE TOXICITY selectively affects the motor system, and produces parkinsonism-plus-dystonia ("strut like a rooster"). However, it does not work on the substantia nigra, but in the caudate and globus pallidus (Neurology 45: 1199, 1998).
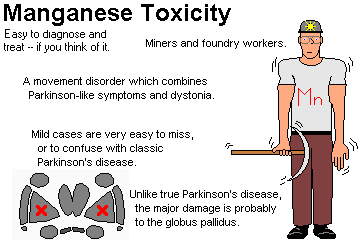
WILSON'S DISEASE features copper deposition, especially in the basal ganglia.
Other genes modify Wilson's. Some patients have primarily neurologic disease while others have primarily hepatic disease.
* PANTOTHENATE KINASE DEFICIENCY (PANK2) causes NEURODEGENERATION WITH BRAIN IRON ACCUMULATION TYPE I (Brain 134: 947, 2011), a hereditary neurodegenerative disease that is easily diagnosed today by the iron accumulation in the basal ganglia.
BAD GAUCHER'S DISEASE, HUNTER'S DISEASE, HURLER'S DISEASE, SANFILIPPO'S DISEASE, TAY-SACH'S DISEASE, and NIEMANN-PICK'S DISEASE feature intra-neuronal storage of their respective products, and eventually loss of mentation.
Also worth remembering are LESCH-NYHAN and PHENYLKETONURIA. Neither is a storage disease, but both are inborn errors of metabolism with serious effects on the nervous system.
LEIGH'S SUBACUTE NECROTIZING ENCEPHALOPATHY (as bad as it sounds) is the result of any of at least 14 different deficiencies in cytochrome C oxidase. Usually a disease of babies, it can strike older children or young adults as well.
FAMILIAL MYOCLONUS EPILEPSY is several genetic illnesses.
* Another form (not the Lafora body kind) is caused by mutant cystatin (cystine protease inhibitor): Nature 381: 26, 1996.
THE LEUKODYSTROPHIES feature bad myelin, rather than demyelinization; typically, the diseases are autosomal recessives and there is problem breaking down myelin. About one child in 7000 is affected; the diseases are often missed until autopsy (Neurology 75: 718, 2010).
METACHROMATIC LEUKODYSTROPHY ("sulfatide lipidosis") is a deficiency in aryl-sulfatase A. The metachromasia is due to sulfatide accumulation.
{31803} metachromatic leukodystrophy patient
{31807} metachromatic leukodystrophy, gross
{31981} metachromatic leukodystrophy, micro. The blue dye stains the metachromatic stuff pink.
* ZELLWEGER'S DISEASE is caused by a lack of functioning peroxisomes in liver, brain, and kidney. Early diagnosis by imaging: Neurology 78: 1304, 2012.
KRABBÉ GLOBOID CELL LEUKODYSTRPHY is a deficiency in galactocerebrosidase. There's bad myelin, with eventual loss of oligodendroglia, plus lipid-laden macrophages clustering around vessels. This is a disease of early childhood with death in a few years.
{32004} Krabbe's globoid histiocytes
* PELIZAEUS-MERZBACHER DISEASE, mutated protolipid protein of myelin, gets discussed a lot because the severe forms are in the "diff" of a profoundly retarded baby. Contrary to "Big Robbins", many adult-onset cases are known. Remember tiger-striping of the white matter.
ADRENOLEUKODYSTROPHY is an X-linked disease in which cholesterol esters accumulate. The business of "Lorenzo's oil" is now history. The 1992 movie was produced despite the fact that the oil does little or nothing to help children who are already symptomatic. However, restricting very-long-chain saturated fatty acids before symptoms appear seems to be helpful, with or without "Lorenzo's oil" (Arch. Neuro. 62: 1073, 2005.)We need to honor the parents of Lorenzo Odone for their efforts (Lancet 373: 888, 2009). It is now being treated with some success using bone marrow transplantation (Lancet 356: 713, 2000).
* CANAVAN'S DISEASE, lack of aspartoacylase, features Alzheimer II glia all over the white matter. (This is in contrast to Alzheimer II glia caused by elevated blood ammonia, where they are most abundant in the gray matter.)
RADIATION NECROSIS of the brain sometimes occurs.
ACUTE RADIATION NECROSIS features widespread necrosis of cells, especially oligodendroglia and the granular cell layer of the cerebellum.
DELAYED RADIONECROSIS may occur in therapeutic-range radiation, after months or years.
In the white matter, all of the glial cells die. Whatever vessels remain exhibit radiation-type changes.
At the edges, look for axonal spheroids. It is likely to be worse if the patient has also taken methotrexate.
{01909} radiation necrosis
|
|
|
|
|
INTRODUCTION
You are familiar with the old expression "malignant by location". This is especially applicable to brain tumors, which may be histologically benign but difficult to remove surgically without damaging important things.
Risk factors for brain tumors are, for the most part, obscure. The classic study that looked at having ever been a professional boxer (double the risk for meningioma) and having had more than five full-mouth dental x-rays before 1945 (when doses were way too high, meningiomas only) is now history (JNCI 70: 863, 1983) and applied only to meningiomas -- the results were probably valid (see below). You know Turcot's anti-oncogene deletion syndrome as a risk factor for gliomas, and of course, previous radiation (i.e., for acute lymphoblastic leukemia or solid cancers of the brain or its coverings) is implicated, too (Cancer 67: 392, 1991).
Just as brain cells may be difficult to distinguish, the histogenesis of most of these tumors is seldom obvious from morphology.
EXTRA-AXIAL tumors inside the skull are outside the brain-and-cord itself. The ones to know are the meningioma and the acoustic neuroma. All the rest are INTRA-AXIAL.
All gliomas are best considered malignant, though some are more malignant than others. No glioma is considered curable by today's medicine, and when they recur, they are likely to be more aggressive (JAMA 303: 967, 2010).
Malignant primary brain tumors are locally invasive, and may spread via the spinal fluid ("neuraxis dissemination", J. Neurosurg. 83: 67, 1995), but very seldom metastasize to the rest of the body.
| "Psychiatric" changes are common as the first signs of a brain tumor. Frontal lobe tumors seem to
produce personality changes and/or depression and/or loss of interest, while temporal lobe tumors
seem to produce hallucinations and/or mania and/or amnesia and/or "panic attacks" (West. J. Med.
163: 19, 1995). Charles Whitman, the University of Texas sniper,
had a glioma involving his frontal and hypothalamic areas. (This likely explains the
severe headaches he's been having; the relationship to his behavior must remain
speculative. Whitman was the
also son of a violent martinet and recorded his struggles to control his
rage in his diaries; he was also on amphetamines.)
Numbers to remember: Around 1% of random autopsies includes a primary brain tumor. In adults, 70% of primary brain tumors are supratentorial. In children, 70% of brain tumors are infratentorial (medulloblastomas by definition arise in the cerebellum, juvenile pilocytic astrocytomas are usually infratentorial, and diffuse pontine astrocytomas are the third common pediatric brain tumor.) |

|
* Update for pathologists on how radiologists use imaging to study brain tumors: Arch. Path. Lab. Med. 131: 252, 2007.
* The treatment protocols for the common brain tumors have been standardized, and a few molecular markers are known for prognostication. It's slow-going. Update Lancet 379: 1984, 2012.
* Junk science! You're heard the pop claim that cellular telephones cause brain tumors. The idea is that "radiation causes cancer"... or perhaps somebody realized that juries in junk lawsuits won't understand the difference between microwave radiation that makes cell phones work and ionizing radiation that damages the genes. In the most recent study, people who use cell phones have only 9/10 of the risk of getting an acoustic neuroma than do non-users, there is no correlation with duration or total use, and the neuroma is somewhat more likely to be on the opposite side. Neurology 58: 1304, 2002. I have already drawn the obvious conclusion. The "Interphone" study found essentially nothing (Int. J. Epid. 39: 675, 2010). The CERENAT French study that supposedly showed a risk actually showed an effect but only in "the heaviest users" -- it was a face-to-face "how much did you talk on your cell phone before you got your brain tumor?" interview study that begs for recall bias, no obvious trend to the tumor being on the same side as your cell phone (Occup. Env. Med. May 9, 2014). The cell-phone / brain tumor lawsuits are becoming an industry.
GLIOMAS
The common tumors arising within the brain itself. As a rule, gliomas stain positive with GFAP.
* The molecular biology was worked out in the 1990's.
* The great white-knuckle call in neuropathology today is "recurrent glioma vs. radiation necrosis" (J. Neurosurg. 82: 436, 1995). Nowadays we are doing molecular typing to solve this toughest of calls: Am. J. Clin. Path. 121: 671, 2004. The radiologists may be able to make the distinction for us, using "molecular" magnetic resonance imaging (Nat. Med. 17: 130, 2011).
* A host of tumors with differentiation as both glia and neurons are now known. Leave these to us (Arch. Path. Lab. Med. 131: 228, 2007).
ASTROCYTOMA / ANAPLASTIC ASTROCYTOMA / GLIOBLASTOMA
These are the most common primary brain tumors in adults (about 80%), and are a continuum of malignancy. There is a slight male predominance.
Astrocytomas tend to become more malignant with time, and ultimately most will probably become glioblastomas. And there is likely to be a mix when you examine the tumor.
ASTROCYTOMAS are poorly circumscribed, whitish brain tumors. Grossly, the most common appearance of astrocytomes is "diffusely infiltrating", with very poorly-defined borders. Microscopically, they may recall protoplasmic, fibrillary, fibrous, or gemistocytic astrocytes, or grow as spindle cells or xanthoma-like cells, or (most often) present a mix.
Protoplasmic astrocytomas are perhaps the most familiar, with the tumor cells each bearing only a few processes, and a background of little holes ("microcystic"); these tumors cells actually look like stars ("astro", Am. J. Clin. Path. 103: 705, 1995).
* In "diffuse astrocytoma" every astrocyte in a region seems to turn neoplastic at once. In "gliomatosis cerebri" (which may be the same thing), the entire brain, especially the white matter, is invaded. I used to wonder about a virus infection; however, it's now quite clear that most of these are aneuploid, like true malignant tumors (Neurology 56: 1224, 2001; Ann. Neuro. 52: 390, 2002). Staining and possible molecular mechanisms: J. Clin. Path. 58: 166, 2005.
* For some reason, the various isocitrate dehydrogenase enzymes tend to mutated in low-grade astrocytimas (IDH1, IDH2).
Daumas-Duport grading system: Count one for each of these criteria:
Grade I: Zero criteria
Grade II: One criterion
Grade III: Two criteria
Grade IV: Three or four criteria
By contrast, the 2007 World Health Organization system arbitrarily assigns a grade to each of over 100 entities. Proteomics as a way of grading astrocytomas: Neurology 66: 733, 2006. For now...
{01497} astrocytoma
{01501} astrocytoma
{01503} astrocytoma
{01518} astrocytoma
{01531} astrocytoma
{15706} astrocytoma
{01504} astrocytoma
{01506} astrocytoma
{01507} astrocytoma
|
|
GLIOBLASTOMA (formerly "glioblastoma multiforme"; Arch. Path. Lab. Med. 131: 397, 2007; JAMA 310: 1842, 2013) is a floridly malignant, variegated (many colors, many kinds of histology) tumor. It is distinguished from the anaplastic astrocytoma by necrosis, very anaplastic cells, and/or the formation of new blood vessels.
It can arise from a pre-existing astrocytoma, or de novo (especially in older patients.)
Also watch methylation of MGMT, which repairs DNA. As you'd expect, if this enzyme is diminished, there's a better response to temozomide.
{01575} glioblastoma
{01576} glioblastoma, butterfly
|
Australian Pathology Museum High-tech gross photos
|
![]() Glioblastoma
Glioblastoma
Coronal section
Wikimedia Commons
Endothelial proliferation ("glomeruli", etc.; you can do a reticulin stain and it will make these areas stand out) and "palisading" of cancer cells around necrotic areas are typical.
Despite massive efforts, median survival rate is about 14 months (up from ten months thanks to the new treatments). However, around 5% survive for three or more years -- this must have something to do with the genetic profile but this remains to be worked out (Brain 130: 2596, 2007).
{01582} glioblastoma
{01584} glioblastoma, dead stuff
{01585} glioblastoma
{01587} glioblastoma, gemistocytes
{01596} glioblastoma, monster cells
{17721} glioblastoma
GLIOSARCOMAS exhibit both glial and mesenchymal differentiation; they often follow radiation (Cancer 75: 2910, 1995; J. Neurosurg. 112: 26 & 990, 2010).
Adult astrocytomas always infiltrate the surrounding tissue, and extend far beyond the obvious tumor mass.
BRAINSTEM GLIOMAS
These are pediatric, malignant astrocytomas, which tend to involve the brainstem and turn into glioblastomas. Many cures are obtainable with radiation.
JUVENILE PILOCYTIC ASTROCYTOMAS (J. Neurosurg. 82: 536, 1995; Cancer 72: 1335, 1993)
These are indolent tumors that typically involve the cerebellums of children. Often they appear as a cyst with a nubbin in the wall. Even if the histology looks nasty, they are likely to grow only very slowly, and they're the only common WHO Grade I glioma other then subependmomas.
"Pilocytic" (hair-like) astrocytes are long and thin, and "Rosenthal fibers" are typical.
* Most of these children grow up as long-term survivors (Cancer 119: 2630, 2013). Although these often do not recur after surgery, or recur late, patients grow up to be substantially less happy then their counterparts. The teenaged years, during which the young person realizes that he/she will never be able to keep up with peers in many different aspects of life, are especially stormy (J. Neurosurg. 96: 229, 2002).
* At least some are driven by mutant BRAF. Watch this as a possibility for targeted therapy: J. Clin. Inv. 121: 1344, 2011.
{01542} juvenile pilocytic astrocytoma
|
|
OLIGODENDROGLIOMAS
These are uncommon gliomas of adults that typically occur in the centrum semiovale.
Grossly, they are gray and soft, often with little calcifications (ask a radiologist). Microscopically, the tumor is sheets of fried-egg cells (* the clearing is caused by the formalin fixation), with round central nuclei and clear cytoplasm. Often there is a admixture of astrocytoma.
Some of these are well-differentiated, others less so, and the WHO leaves the decision as to whether it's a "grade II" or "grade III" to the pathologist's experience. Today, it is usual to test a suspected oligodendroglioma for combined loss of 1p and 19q, which confirms that it is an oligodendrogliioma and (for the more anaplastic lesions) is a marker for favorable prognosis and good response to chemotherapy (Arch. Path. Lab. Med. 131: 242, 2007). We now report "genetically favorable oligodendroglioma".
{01618} oligodendroglioma
{01620} oligodendroglioma
{01624} oligodendroglioma with calcifications (shown reddish-purple here)
{01626} oligodendroglioma with calcifications
EPENDYMOMAS (pathology Cancer 106: 388, 2006)
These arise from the single layer of glia that lines the ventricles.
Pediatric ependymomas generally arise in the fourth ventricle. As you'd expect, they can cause hydrocephalus and are tough to excise.
{01642} ependymoma (trust me)
{15699} ependymoma (trust me)
Adult ependymomas are the common spinal cord glioma (astrocytomas less common -- J. Neurosurg. 83: 590, 1995.)
Pathologists talk about true / Flexner rosettes (little attempts to make neural tubes, with a clear ring instead of the of delicate fibrillary material in the middle as in the Homer-Wright rosettes seen in some medulloblastoma-neuroblastomas), pseudo-rosettes (around vessels), and "ependymal rosettes" with blepharoplasts (the basal bodies of cilia, visible by * PTAH stain). (Today, ependymal rosettes with blepharoplasts are separated from other "true" rosettes.)
* Pathologists confirm the diagnosis of ependymoma by finding positive staining for epithelial membrane entigen (Arch. Path. Lab. Med. 131: 234, 2007) -- "because ependyma is a kind of epithelium" -- and glial fibrillary acid protien "because it is glia".
* Histologic grading for prognosis: Cancer 100: 1230, 2004). Another group finds that only mitotic count / MIB-1 labelling index correlates with prognosis: Cancer 106: 388, 2006. This all remains very unsettled.
* Many other brain tumors can express "ependymal features"; no one knows what this means, but hard-core learners who like great photos can see J. Neuropath 67: 177, 2008.
* Although ependymomas are gliomas and thus cures are never certain, even posterior fossa ependmomas that are operated and radiated have a 10 year survival of 85% with pretty good outcomes (J. Neurosurg. 120: 1063, 2014).
{01650} ependymoma
{01654} ependymoma
{01656} ependymoma, blepharoplasts
* Childhood ependymomas and choroid plexus papillomas and SV40 virus (or its
kin): NEJM 326: 988, 1992. This is holding up for other
gliomas as well (Cancer 94:
1037, 2002; J. Neurosurg. 95: 96, 2001; Am. J. Med. 114: 675, 2003), but there's considerable doubt that this is actually a pathogen;
more likely it's reactivation. You already know that SV40 contaminated some of the
early polio![]() vaccines.
vaccines.
* Ependymomas and choroid plexus papillomas expressing genes from the JC virus: J. Neurosurg. 102(S3): 294, 2005.
* MYXOPAPILLARY EPENDYMOMAS arise from the filum terminale, resemble gelatinous sausages, and are histologically distinctive. The tumor cells form collarettes over the surfaces of dense fibrous cords; there's a layer of mucin between.
{01665} * myxopapillary ependymoma
{01666} * myxopapillary ependymoma
![]() Myxopapillary ependymoma
Myxopapillary ependymoma
WebPath Photo
SUB-EPENDYMOMAS are the most indolent of gliomas, arising from the ventricular walls. The classic case is an asymptomatic mass found at autopsy in the fourth ventricle of an older man. These tumors can occasionally be symptomatic (rays: AJR 165: 1245, 1995).
CHOROID PLEXUS PAPILLOMAS may occur at any site in the ventricles, and are most common in children. They are generally benign, but cause problems by overproducing spinal fluid or blocking its flow.
* Future pathologists: Distinguish these from metastatic carcinoma by their being GFAP positive! The rare choroid plexus carcinomas have anaplasia and local invasion.
* You will be bewildered by the ongoing experiments using
herpes simplex virus![]() , its thymidine
kinase, and gancyclovir to infect and then selectively kill glioma cells. Suicide
gene therapy. J. Neurosurg. 79: 729, 1993;
J. Neurosurg. 81: 256, 1994, Proc. Nat. Acad. Sci. 93: 3525, 1996.
There is now talk of occasional cures
(Neurology 58: 1109, 2002) though usually it's not a great success
(J. Neurosurg. 112: 328, 2005).
, its thymidine
kinase, and gancyclovir to infect and then selectively kill glioma cells. Suicide
gene therapy. J. Neurosurg. 79: 729, 1993;
J. Neurosurg. 81: 256, 1994, Proc. Nat. Acad. Sci. 93: 3525, 1996.
There is now talk of occasional cures
(Neurology 58: 1109, 2002) though usually it's not a great success
(J. Neurosurg. 112: 328, 2005).
|
|
NEURONAL TUMORS
Neuroblastomas can arise in the cerebral hemispheres of children, and ganglioneuromas and gangliogliomas (i.e., a mix of neoplastic neurons and glia from a common clone: Am. J. Path. 151: 565, 1997) can be found in the CNS, too.
![]() Ganglioglioma
Ganglioglioma
Pittsburg Illustrated Case
Primitive neuroectodermal tumors ("PNET's") in the CNS itself are generally MEDULLOBLASTOMAS (Arch. Path. Lab. Med. 135: 984, 2011).
These typically arise in the cerebellum of younger people ("the commonest posterior fossa tumor in children"), and tend to spread up and down the neuraxis by way of the spinal fluid.
These tumors strike at random. Turcot's (familial polyposis -- either familial adenomatous polyposis coli / APC or hereditary non-polyposis colon cancer / HNPCC ... plus brain tumors, review South. Med. J. 101: 1273, 2008) and the basal cell nevus syndrome (PTCH antioncogene deletion) are the two known risk factors.
{31933} medulloblastoma, cord
{01677} medulloblastoma
{01686} medulloblastoma
{01687} medulloblastoma (cord and dura)
{18761} medulloblastoma
|
|
The new systems for grading correlate quite well with outcome (Cancer 94: 552, 2002).
Neuropathologists point out that these cells show both neuronal (Homer-Wright rosettes, pseudo-rosettes, synaptophysin stain) and glial (GFAP-positive) differentiation.
* The genetics has recently been worked out (J. Clin. Onc. 10: 1627, 2009).
* Medulloblastomas may excite a desmoplastic, fibrous response ("fibrous medulloblastomas", "desmoplastic mesothelioma", the old "cerebellar sarcoma" -- many carry the "patched" mutation).
The tumor is radiosensitive, or may be found early enough to enable a surgical cure. There is about a 50% 5-year survival.
* Nobody's ever identified a "medulloblast" -- the cells remind me of the fetal external granular layer of the cerebellum.
* Several variants of primitive embryonic-type tumors in the brains of children are now described, including some with true (lumen-in-the-center / Flexner) rosettes (Am. J. Clin. Path. 126: 277, 2006).
The substantial majority of children with medulloblastomas now get cures, even a majority of childern with high-risk features (amplified n-myc, large tumor cells, Lancet Oncol. 7: 813, 2006).
|
|
MENINGIOMAS (Lancet 363: 1535, 2004)
|
|
These are tumors of the arachnoid cap cells, and make up about 25-30% of primary brain tumors and around 25% of spinal canal tumors. Most occur where there are arachnoid granulations (i.e., next to the falx or tentorium or on the lesser wing of the sphenoid bone. However, they can occur on any surface in the head.
Patients are usually middle-aged, and there is a moderate female predominance.
The basic biology of these lesions is obscure. There is a link to head trauma (Science 254: 1131, 1991) and many meningiomas exhibit monosomy 22 (Science 254: 1153, 1991; Cancer 77: 2567, 1996). NF2 (neurofibromatosis type II, autosomal dominant mutated "merlin") is a powerful risk factor, and not surprisingly, sporadic meningiomas often have mutated merlin. Neurofibromatosis type I is not a risk factor.
Meningiomas usually (around 90%) express the progesterone receptor, and RU-486 (mifepristone, "the abortion pill") is now in use for nonresectable meningiomas (the weird politics: JNCI 89: 912, 1997).
The link to head trauma, especially 10-19 years earlier, reaffirmed: Neurology 58: 1849, 2002. The risk to previous radiation, particularly brain tumors and quack ringworm treatment, is well-established, and the link to old-fashioned high-dose dental x-rays has been reaffirmed as a risk factor for meningiomas: Cancer 100: 1026, 2004. NF2 (neurofibromatosis type II, autosomal dominant mutated "merlin") is a powerful risk factor, and not surprisingly, sporadic meningiomas often have mutated merlin.
* Please ignore everything you may hear about smoking and/or breastfeeding as a risk factor or protective factor for meningioma; the survey results are wildly discrepant.
Grossly, the tumors are usually firm, and solid, perhaps with a whorly pattern on cross section.
Future radiologists: Look for thickening of the bone over the meningioma.
Microscopically, there may be primarily whorls and nodules (as in healthy arachnoid; this is the MENINGOTHELIAL MENINGIOMA), or spindle cells (FIBROUS MENINGIOMA), or intermediate forms (TRANSITIONAL MENINGIOMAS; look for psammoma bodies, and if there are a huge number you may call it a PSAMMOMATOUS MENINGIOMA. A slightly more aggressive but still benign variant is the ANGIOBLASTIC MENINGIOMA.)
You can find mixtures of the above, various degenerative changes, or occasionally, evidence of malignancy.
* Future pathologists: Meningiomas stain for epithelial membrane antigen (EMA) unlike most other intracranial masses. On electron microscopy, look for lots of desmosomes.
Mitotic counts are key in prognosticating (Am. J. Clin. Path. 128: 118, 2007.) In both 2000 and 2007, the World Health Organization published new systems for grading meningiomas; most are grade I and the others have high MIB labeling indices and/or distinctive patterns.
* Occasionally, a hemangiopericytoma will look grossly like a meningioma. These tend to be more aggressive.
ANAPLASTIC MENINGIOMAS are rare; they are diagnosed the the cells are wildly anaplastic and/or there are 20 or more mitoses / hpf. Two year survival is around 50%.
Molecular markers for meningiomas are being developed. A majority have mutated NF2 and/or a deletion on chromosome 22 of material near NF2 (some other gene must be involved); loss of 1p is commonly a feature of progression toward malignancy.
Meningiomas can generally be removed for cure by surgery or gamma knife; recurrences may be more and more abnormal morphologically (recently reconfirmed Cancer 117: 1272, 2011). The sudden appearance of a very anaplastic sarcoma where a meningioma used to be suggests a second primary (* consider NF2 - Arch. Path. Lab. Med. 135: 935, 2011).
Multiple meningiomas: Think of neurofibromatosis-2; not surprisingly, the NF2 gene on chromosome 22 is often mutated in its conserved region in any meningiomas (Am. J. Path. 146: 827, 1995).
* Meningiomatosis: Lots of little meningiomas around proliferating blood vessels, forming a mass that needs to be removed, since it causes seizures (Arch. Path. Lab. Med. 119: 1061, 1995; Arch. Path. Lab. Med. 120: 587, 1996).
* Future oncologists: Chemotherapy for high-grade meningiomas has historically not been a great success. Trabectedin, a DNA-binding protein from the sea squirt Ecteinascidia turbinata has been used on a single patient with good results (Cancer 118: 5038, October 2012). It's an orphan drug used experimentally; the mechanism of action is unclear.
{00221} meningioma, gross
{31996} meningioma
{00224} meningioma, micro
{09459} meningioma, with psammoma bodies
{09460} meningioma
{09462} meningioma
OTHER BRAIN TUMORS
PRIMARY NON-HODGKIN'S LYMPHOMAS OF THE BRAIN ("microgliomas" is an archaic misnomer): reviews Cancer 74: 1383, 1994; J. Neurosurg. 82: 558, 1995 (HIV negative cases); Am. J. Clin. Path. 121: 246, 2004 (post-transplant CNS lymphomas); Arch. Path. Lab. Med. 132: 1830, 2008.
Transplantation and AIDS have rendered this an important topic.
Epstein-Barr virus![]() is usually
present (and strongly suspect as a cause) in transplant and AIDS lymphomas, though not in sporadic
brain lymphomas (Neurology 43: 1591, 1993).
is usually
present (and strongly suspect as a cause) in transplant and AIDS lymphomas, though not in sporadic
brain lymphomas (Neurology 43: 1591, 1993).
You already know that EBV![]() and herpes 8
and herpes 8![]() (Kaposi's sarcoma virus), together or separately, are
infamous causes of non-CNS lymphomas in the immune-compromised. Herpes 8 seems to be
exonerated, however, as a cause of CNS lymphomas, being present only in the
bystander cells (J. Clin. Path. 54: 617, 2001).
(Kaposi's sarcoma virus), together or separately, are
infamous causes of non-CNS lymphomas in the immune-compromised. Herpes 8 seems to be
exonerated, however, as a cause of CNS lymphomas, being present only in the
bystander cells (J. Clin. Path. 54: 617, 2001).
* Not surprisingly, the rate of primary CNS lymphoma is way down over the past few years (Cancer 95: 193, 2002), except among very old folks -- HIV is now manageable, and immunosuppression for transplant recipients is less severe.
* The concern that polyomavirus may cause CNS lymphomas has been dismissed by molecular biology: Neurology 63: 1299, 2004.
* miRNA's in the CSF as a sensitive and specific marker for primary CNS lymphoma: Blood 117: 3140, 2011.
A host of different types of lymphoma histologies have been reported, with a tendency nowadays toward bigger, meaner-looking cells (Blood 96: 4084, 2000). Most are large B-cell lymphomas. These tumors tend to follow vessels (check the reticulin pattern; reticulin is likely to be rather dense in these tumors, which helps us tell they are not just inflammation). Death usually results in a few weeks to a year or two.
* We used to think that these tumors mostly stayed local in the CNS, and that systemic lymphomas can't present as apparently-localized CNS lesions. Depending on circumstances, you may still want to stage (Cancer 77: 827, 1996).
|
|
![]() CNS Lymphoma
CNS Lymphoma
Biopsy
Wikimedia Commons
HEMANGIOENDOTHELIOMAS / HEMANGIOBLASTOMAS are distinctive tumors of the cerebellum that mimic very low-grade renal cell carcinoma (!).
Like renal cell carcinomas, these tumors even produce erythropoietin and cause polycythemia. Patients generally have Von Hippel-Lindau anti-oncogene deletion syndrome. Look for impressive blood vessels, and lipid-laden foam cells.
* Future pathologists: These tumors even resemble renal cell carcinoma by their positivity for ezrin, an epithelial cell marker responsible for anchoring actin to the cell membrane (Am. J. Path. 148: 367, 1996). Every once in a great while, a hemangioblastoma occurs outside the cerebellum (Arch. Path. Lab. Med. 127: e382, 2003).
{01878} hemangioblastoma
{01882} hemangioblastoma
{01884} hemangioblastoma
CHORDOMAS are uncommon tumors of the vestigial notochord (ask a comparative anatomist) that occur at the sacrum or clivus. Some are so bland histologically as to be considered "malignant only by location" when within the skull. Historically, even these were deadly, the intracranial lesions taking out the cranial nerves progressively until death ensued.
* Don't worry about the histology, which features "bubble cells". Pathology update Cancer 93: 40, 2001; clinicians Lancet Onc. 13: e69, 2012.
Once uniformly lethal, new radiation techniques are giving apparent cures for some patients: J. Neurosurg. 91: 432, 1999, others. Update J. Neurosurg. 102 S: 165, 2005. Imatinib: Cancer 101: 2086, 2004 (awaiting confirmation). Since the tumor is rare, grows slowly, and recurs unpredictably, the best we can say for sure is that today's techniques have made this lesion far more manageable.
* The tumor genetics are only starting to be examined. There is no known signature mutation. p53 overexpression (not surprisingly) correlates with poor prognosis (Cancer 104: 1255, 2005).
{01897} chordoma (note the resemblance to primitive cartilage)
{01899} chordoma
{01906} chordoma ("bubble cells")
We have already mentioned COLLOID CYST OF THE THIRD VENTRICLE as a cause of hydrocephalus.
CRANIOPHARYNGIOMAS: Rathke's pouch tumors in the pituitary-hypothalamic region. As before, look for machine-oil cysts grossly and the recapitulation of embryonic teeth (ameloblasts, calcium, squames) microscopically.
{01855} craniopharyngioma
{01858} craniopharyngioma
{01860} craniopharyngioma
{01861} craniopharyngioma
{10962} craniopharyngioma
{01857} craniopharyngioma cyst fluid
|
|
TERATOMAS (J. Neurosurg. 109: 126, 2008), DERMOIDS (Arch. Path. Lab. Med. 119: 371, 1995), LIPOMAS, EPIDERMAL CYSTS, and so forth may be seen, especially within congenital (?) defects in the corpus callosum.
GERMINOMAS of the pineal, hypothalamus, and elsewhere ("midline!") usually mimic seminoma (staining for placental alkaline phosphatase is confirmatory), less often embryonal cell carcinoma, choriocarcinoma, and/or other testicular cancers; the more primitive-looking the cancer (i.e., not seminoma), the worse they behave (J. Neurosurg. 86: 446, 1997).
METASTATIC CANCER is by far the most common "brain tumor".
The most common primary sites are lung (by far; seeking the primary ARJ 168: 1339, 1997), breast, melanoma, kidney, and gut.
Around 50% of smokers dying of lung cancer have "brain mets", and these are not uncommonly the actual cause of death.
* Future pathologists: Using your arsenal of special stains can tell the origin for most metastases. TTF-1 is probably lung adenocarcinoma. Cdx2 is probably a GI primary; CK20 suggests GI but is less specific (Arch. Path. Lab. Med. 131: 1686, 2007).
The best place to find them is at the corticomedullary junction (the cancer cells get trapped as the vessels narrow at their entry to the white matter -- once your instructor's pet idea, now confirmed Cancer 77: 1551, 1996). There is generally much edema around a "met", and treatment just to reduce the edema helps.
* The prognosis for these patients is of course very grave, but the new gamma-knife technique is providing some long-term survivals for occasional patients with brain metastases (Cancer 104: 2784, 2005).
{09442} melanoma
{29393} breast cancer metastasis
|
|
Metastatic cancer in the spinal canal often encases the spinal dura and impinges on nerve rootlets. The meninges (cord and brain) may also be packed with a thin layer of cancer ("meningeal carcinomatosis", a diagnosis typically made only at autopsy.)
* Surgical excision of a solitary metastasis with hope for a long-term survival: J. Neurosurg. 83: 605, 1995, Chest 109: 271, 1996; Cancer 78: 711, 1996. Happens, rare; usually colon primary.
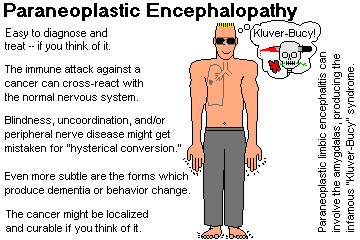
PERIPHERAL NERVE
|
|
|
The anatomic pathology of the peripheral neuropathies is the most arcane area in pathology. Don't worry too much about it.
The pathologist will look for:
CRITICAL ILLNESS POLYNEUROPATHY, seen in the intensive care unit and infamous as a cause of inability to wean a patient from a ventilator, is now known to be damage to axons (motor more than sensory;) caused by "the systemic inflammatory response syndrome", i.e., some cytokine(s) in someone seriously sick (Muscle Nerve 32: 140, 2005; review of the syndrome by the original physician to characterize it). It is quite common and probably underdiagnosed. (Suspect it when there is a facial response to painful stimuli, but the limb does not withdraw. Prove it's a neuropathy when phrenic nerve stimulation fails to cause the diaphragm to move.)
GUILLAIN-BARRÉ syndrome (Lancet 363: 2136, 2004; NEJM 366: 2294, 2012) is a relatively common (1 person in around 70,000 gets it per year), serious, generally non-fatal, autoimmune disorder of the motor roots.
Patients experience ascending paralysis and areflexia. If they can be supported through weeks or months of paralysis ("You see, I DID hear everything you said!"), survival is the rule, though there may be some permanent weakness (~20%). In the ~5% of cases in which death occurs, pathologists note demyelinization of the motor rootlets.
The disease typically follows some viral (notably
CMV![]() )
or other (notably Campylobacter jejuni infection and H. 'flu,
which lead to the axonal variant -- see Brain 123: 2171, 2000;
Arch. Neuro. 68: 445, 2011 for the immunology of campylobacter cases.)
)
or other (notably Campylobacter jejuni infection and H. 'flu,
which lead to the axonal variant -- see Brain 123: 2171, 2000;
Arch. Neuro. 68: 445, 2011 for the immunology of campylobacter cases.)
IV immunoglobulin is the mainstay of treatment, though no one really knows how it works (Neurology 62: 1939, 2004).
Other PERIPHERAL NEUROPATHIES form a bewildering array. Remember:
|
|
* Ascorbic acid helps an animal model: Nat. Med. 10: 396, 2004.
* For painful neuropathies, try topical capsaicin, the stuff in hot peppers (it acts by opening sodium and calcium channels, and somehow depletes substance P).
NERILEMMOMAS ("schwannomas") arise from cells of the fibrous tissue surrounding nerve bundles. The nerve is at the edge of the lesion.
As a result, the nerve runs along the edge of the tumor, and resection is generally possible.
Ask any pathologist to show you "Antoni A" (palisaded spindle cells forming "Verocay bodies" / "zebra stripes", supposedly in imitation of Pacinian corpuscles), and myxoid "Antoni B" areas. They light up famously with S100.
{01846} schwannoma
{01849} schwannoma
{15694} eighth-nerve tumor
|
|
|
|
|
|
|
|
"Acoustic neuromas" are schwannomas of the eighth cranial nerve. This is a common location. Especially if bilateral, ask about neurofibromatosis (especially type II, schwannomin gene: Nat. Genet. 18: 382, 1998).
* There's a multiple schwannoma syndrome that spares the eighth nerves; the gene is SMARCB1.
{11031} eighth-nerve tumor
{15693} eighth-nerve tumor
PLEXIFORM NEUROFIBROMAS arise from the fibrous tissue within nerve bundles. They are traversed by the nerve fibers, and resection will require sacrificing the nerve. They usually mean neurofibromatosis; most neurofibromas that turn malignant begin as plexiform neurofibromas.
Most of the neurofibromas in classic neurofibromatosis are CUTANEOUS NEUROFIBROMAS, subcutaneous bumps. While these look strange, they have very little malignant potential. Anyone can get a lone cutaneous neurofibroma, but in neurofibromatosis, there can be hundreds.
* "Diffuse neurofibroma" looks like thick nerve trunks with chunks of collagen ("Wagner-Meissner bodies"). It's thoroughly benign.
Of course, neurofibromas also light up with S100.
A "triton tumor" is a neurofibroma that makes rhabdomyoblasts. This really happens -- something about the Triton newt regenerating its legs, remember from biology?
{01843} von Recklinghausen's of cauda equina
{01854} neurofibroma, trust me
* Despite conventional wisdom, and the fact that skin over big neurofibromas can get to be elephant-like, the "elephant man" had Proteus syndrome instead.
 Paraganglioma
Paraganglioma
Pittsburgh Pathology Cases
|
How many psychiatrists does it take to screw in a light bulb? {18601} |
[Gilgamesh, the warrior-king, has left his kingdom to find an answer for death. On his journey, he meets a barmaid. She tells him:]
 |
Gilgamesh, where are you hurrying to? You will never find the
answer for which you are looking. When the gods created humankind, they allotted us to death, but
life they retained in their own keeping. As for you, Gilgamesh, fill your belly with good things; day
and night, night and day, dance and be merry, feast and rejoice. Let your clothes be fresh, bathe
yourself in water, cherish the little child that holds your hand, and make your wife happy in your
embrace; for this too is the lot of humankind.
-- 2600 B.C.
|
After sixty years on this planet, I have concluded (for now) that what we call "a person" is fundamentally a spiritual process. After reviewing what evidence I could find, it seems most reasonable to me to think that we inhabit our human bodies and human brains (the products of Darwin's world) only temporarily. This doesn't bother me as a man of science, since I'm impressed by anecdotal accounts of phenomena that do not fit the familiar scientific paradigms but that have resisted systematic study. Relativity and quantum theory have satisfied me that the universe is stranger than we think, or even than we can think, even before we consider the riddle of consciousness. Considering spirit and body to be distinct helps me deal (though not in full) with questions of religious faith in Darwin's world. Why spirit and body have been joined remains the great question, which I will pass along to you. Like Socrates, I've heard it whispered that the answer involves "Love" with a capital "L".
Humankind began performing ceremonial burials at least 50,000 years ago, and we may assume that we've been contemplating our own mortality at least since that time. While discovering the relationship of mind and brain would seem a key to determining the true nature of human beings, there seems to be no easy answer. Philosophers regard this as a key problem, and (to my knowledge) all the great world-faiths allow considerable room for discussion.
The mind and the body (brain) might be related in any of several ways. This is a short survey of the principal positions; my amateur effort made it past a philosophy professor when I first prepared it in 1984.
INTERACTIONISM describes the mind and brain are distinct and equally real; during life, the mind effects changes in the material brain (presumably by telekinesis). Philosopher Karl Popper and neurosurgeon Sir John Eccles currently (1984) maintain this view. Popper says "the mind plays on the brain as the pianist plays on the keyboard". Parapsychology has failed to demonstrate any such force to most people's satisfaction. Neuroscience hasn't found it, either (nor can I imagine how we could, at present). Physical causation is easily demonstrated in our world, but no case of non-physical causation been demonstrated. (But psychologists do continue to study mind as if it obeyed causal laws.) Of course, interactionism probably violates the laws of conservation of energy, momentum, and so forth. Niels Bohr (of the Bohr atom and much more) pointed out that the microprocesses of the brain are of an order of magnitude where quantum indeterminacy should make a difference. Anyway, the laws of physics have never really been tested for neurons. Most recently (late 1990's and after), a significant minority opinion in science is "quantum mind", the best-known of several proponents being major-league quantum physicist Roger Penrose. This is my position at least for now. An interactionist may believe (but does not have to believe) that all mental events are accompanied by physical change in the brain. NOTE: Some people (especially those interested in parapsychology) talk about "a different kind of matter", unknown to conventional science, which forms a second body for spirits, the dead, etc. (Popularized in Ghost.... and there are some interesting anecdotes.... but no convincing demonstrations have been forthcoming from the parapsychologists, despite decades of trying.) Dante (Purg. canto 25) describes how ontogeny recapitulates phylogeny (this will surprise those of you who believe that the medieval mindset was anti-science -- that's simply wrong) and follows this discussion with an account of interactionism (following Aquinas, Dante believed that God creates and infuses the soul when, and only when, the brain is prepared). After death, a new body is created from the matter of the spiritual realms. Philosophically, this is unrelated to interactionism (and not so interesting); the problems of how "mind" can be related to "subtle matter" are as difficult as defining how mind and brain interact.
PARALLELISM regards both mind and matter as closed systems, each with states determined by its own laws. However, they have been set in motion so that, in the course of time, every change in one corresponds to a change in the other. Leibnitz (co-discoverer of calculus) compared mind and brain to two clocks set in motion simultaneously. Though they always show the same hour, neither influences the other. I don't know anybody who believes this nowadays, or why anybody would.
EPIPHENOMENALISM sees mind as real and different from brain, but as dependent on brain and exerting no causality it. I suspect this is the practical view of most medical doctors.
MATERIALISM sees matter as possessing an ontological priority to mind. (Brain is ultimately "more real than" mind.) The assumption is that as neuroscience advances, it will become possible to explain all behavior without postulating mental causes. Interactionists assume the opposite, of course. RADICAL BEHAVIORISM, as explained by B.F. Skinner, defines behavior as the set of observable responses of an organism to stimuli. Skinner was unconcerned with non-observable mental states, denied that mental states are causes, are real, etc. Most of us, however, find being conscious interesting. For specialists: REDUCTIVE MATERIALISM describes the mental as no different from the physical. EMERGENTIST MATERIALISM views mental events as a special set, though a distinguished set, of brain states. ELIMINATIVE MATERIALISM denies the reality of mental states at all. LOGICAL BEHAVIORISM ddefined mental states in terms of dispositions to certain behaviors (although it might be hard to define these behaviors completely). It is hard for logical behaviorists to explain how one mental state causes another, or how a mental state can result in no behavior. CENTRAL-STATE IDENTITY THEORY views mental events as real and as causes, but they are identical with microstates of the brain. Some theorists claim (and I have no idea why) that all the mental events that could possibly exist must correspond to neuronal states. Others claim only that all known mental events correspond to neuronal states. The former theorists deny that a machine or a disembodied spirit or a Martian could think; the latter theorists consider this possible.
FUNCTIONALISM, based on information theory and work in artificial intelligence, seeks to avoid the difficulties of both interactionism and materialism. This view compares mind to computer software, brain to computer hardware. The "personal self" is the self-organizing portion of the program within the computer of the brain. Thus, it is meaningful to talk about mind affecting brain, whether or not we believe in the ultimate physical determinacy of the brain. The mind obeys its own set of laws. Exactly what "consciousness" has to do with all of this is unclear. Most of us do not think "consciousness" is the same as a computer program's ability to edit itself. Functionalists do not care whether all mental events are related to changes in neurons, or whether the same organization might be operative in other systems (machines, disembodied spirits, etc.) A personal after-life requires only that the same software be run on a different machine. David MacKay thinks this is quite possible; Roger Sperry is pessimistic....
Further reading for physicians on mind and body:
Churchland, P.S., "Mind-Brain Reduction: New Light from the Philosophy of Science", Neuroscience 7: 1041-7, 1982
Fodor, J.A., "The Mind-Body Problem", Scientific American 24: 114-123, Jan., 1981.
Friedman, D.X. "The Search: Body, Mind, & Human Purpose", Am. J. Psych. 149: 858, 1992. Not hard metaphysics like some of the others, but thoughts on what psychiatry is all about. Good quotation from Claude Bernard.
Greyson, B., "Distressing near-death experiences", Psychiatry 55: 95, 1992. The title is understated. Echoes of "Revelation" or Dante.
Greyson, B., "Varieties of Near-Death Experience", Psychiatry 56: 390, 1993. Prevalence and impact. The impact on a person's behavior is generally salutary. Dutch 13-year prospective study of near-death experiences: Lancet 358: 2039, 2001. The authors discussed whether it could be paranormal, and noted if it were just physiology, there should be some identifiable correlates with duration, medication, attitudes, and so forth -- but there was not.
Hebb, D.O., "Consider Mind as a Biological Problem", Neuroscience 6: 2419-2422, 1981. I couldn't follow this one.
Lukoff, D., et. al., "Toward a more culturally sensitive DSM-IV", J. Nerv. Ment. Dis. 180: 673, 1992. Despite the trendoid title, this is a past-due call for psychiatrists to deal more intelligently with religious issues, whether "cultural" or the spontaneous religious experiences that happen to lots of people.
MacKay, D.M., "The Interdependence of Mind and Brain", Neuroscience 5: 1389-91, 1980
-, "Ourselves and Our Brains: Duality Without Dualism", Psychoneuroendocrinology 7: 285-94, 1982.
Owens, J.E., et. al., "Features of the near-death experience in relation to whether or not patients were near death", Lancet 336: 1175, 1990. (It's much more likely to happen if you're really near death than if you just think you are. The author thinks this favors "the transcendent hypothesis".)
Sabom, M., Recollections of Death, now out of print. Formerly the chief cardiologist at the Atlanta VA Hospital, Dr. Sabom told me in 1980 that, in his series of dozens of patients who reported having watched their resuscitations, they were uniformly accurate, without a single major error. He played a great tape for me ("The blood went in that doctor's shoe" and indeed it had, etc.; upon seeing his own heart, the guy made the two classic observations a medical student makes at an autopsy.) This strikes me as more impressive evidence for "the transcendent hypothesis" (instead of "hallucinations from lack of oxygen to the brain" or whatever) than do the stories about "light, love, and meaning", though Dr. Sabom records these, too. Dr. Sabom was subsequently fired, supposedly for his interest in parapsychology, but today's skeptics (understandably) consider him the most respectable near-death experience researcher.
Sperry, R.W., "Mind-Brain Interaction: Mentalism, Yes; Dualism, No", Neuroscience 5: 195-206, 1980.
Stevenson, I., Journal of Nervous and Mental Diseases 165: 152-70, 1977. The guy who investigates reincarnation claims around the world, and is also a psychiatry professor at Virginia, writes about the empirical evidence for and against survival after death. Still interesting, though you won't find a definitive answer here.
"Can science explain consciousness?" Sci. Am. 271(1): 88, July 1994. I didn't understand this one, either.
Kendler, KS. "A Psychiatric Dialogue on the Mind-Body Problem". Am. J. Psych. 158: 989, 2001. Following Plato's dialogues, an attending talks with three residents. Highly recommended.
Kendler, KS, "Toward a Philosophical Structure for Psychiatry", Am. J. Psych. 162: 433, 2005. "Cartesian substance dualism is false. Epiphenomenalism is false."
The grave is the first stage of the journey into eternity. -- Muhammad
NOTE: Studying for the licensure examination in basic sciences? Around this time, students often ask "What's the best way to review for 'National Boards' in Pathology"? The answer is, "Whatever book or set of notes you can read with comfort, comprehension, and interest." This might be anything from re-reading "Big Robbins" (generally favored by students who feel stronger), the "ERF handouts" or a review book, to various quiz books and quiz banks (generally favored by students who feel too weak to remain focused on a text; but be sure you look up why answers are right or wrong!). Only you can tell what feels right for you.
* ADVANCE DIRECTIVES
Mine has been essentially the same since 1973. Now that I've
hit fifty years of age, make that percentage odds business equal to my chronolocial
age.
In
case of serious disease or serious injury leaving me with less than a 50%
chance of a return to
meaningful life, institute no therapy except for hygiene
and
relief of pain and respiratory distress. If intravenous, endotracheal,
or stomach
lines are already in
place, you must remove them.
"Meaningful existence" means able to say, write, sign, or fingerspell
the Lord's Prayer at the right time in a church service. This is
a carefully considered definition that since the 1970s still meets
every contingency of which I can think.
Specifically, in case of an
acute subarachnoid hemorrhage with coma, do not initiate any life-maintaining
intervention. Administer analgesics and other comfort measures only.
When there is less than a 50% chance of a return
to meaningful life,
allow me to die of dehydration if active euthanasia or death by organ donation
is not feasible.
I have experienced prerenal azotemia with BUN
near 100 and it is not really so unpleasant. [I added this in 1977.]
If I have less than a 50% chance of returning to work, or if I am fully
retired, do not administer
antibiotics. In an unwitnessed cardiac arrest or if I am fully
retired, do not begin CPR or continue it if begun. In all circumstances,
let the above serve as a guide to my thinking.
On Annunciation Day 2010, after reading the American Heart Association
statistics in Crit. Care Med. 38: 101, 2010, I had "No CPR"
tattooed on my chest. This is something I had been wanting to do since
medical school. The only exception would be open-chest surgery,
as I am told is customary in "DNR" patients.
I'm on record -- commenting on the very expensive chemotherapeutic agents that buy a few months --
that I'd decline any intervention at a cost more than $5k/month gained.
I have previously remarked
that as an invalid or inactive person not able to contribute further to those around me,
it would be unconscionable for me to allow other living things to be killed to feed me.
I have given myself out to be a mainstream Christian throughout my entire
adult life. All spiritual values proceed from relationships among people --
in fact, I believe that even the Good Lord is a community of three Persons though this is a
doctrine that I do not pretend to understand fully. Without
the ability to act in relationships, my natural life has no value.
My body goes for anatomic dissection and/or my organs are to go for
transplantation as appropriate for my manner of death.
You may consider me
legally dead when I have no reflexes off medication.
Although I am a
gentle soul and have actually helped anti-death penalty activists,
I have never opposed the death penalty itself. Let this be remembered
in the unlikely event that I am murdered. My last will (2004) is in the possession
of my house buddy, executor, and principal heir Lewis Burton.
Memorial services follow the rite of the Episcopal Church,
with white vestments please, as was the custom among the ancient
Christians. Keep
the tone light and humorous as I would have done, and remember that
"All Creatures of our God and King" was my favorite hymn.
There's a video of my reading Plato's "Phaedo" somewhere that people
would enjoy on this occasion.
After dissection (anatomy class, autopsy, or organ donation
plus autopsy),
my body is to be cremated and my
ashes are to be scattered by other skydivers as per our custom.
I expressly forbid burial under any circumstances, though keeping any
interesting pathology specimens around for teaching is strongly encouraged.
The atoms
of which my body was composed never belonged to me and do not belong
to my heirs, but to
the Good Lord, and He deserves them returned to His creation.
Have
a nice day.
|  |
*SLICE OF LIFE REVIEW
{01152} brain, immature but normal
{01215} oligodendrocyte, normal
{01221} microglia, resting in normal cortex
{01222} dorsal root ganglion, normal
{01228} eye, normal
{01230} frontal lobe, normal cerebral cortex
{01231} occipital lobe, normal cerebral cortex
{01239} pineal gland, normal
{01273} neuron, normal
{01351} neuron, normal with glia
{01356} astrocytes, foot processes on capillaries
{01408} oligodendrocyte, normal nerve tracts
{01409} oligodendrocyte, normal
{01410} oligodendrocyte, normal
{01435} myelin, normal
{03695} transverse sinus ligament of marshall, normal
{04442} leptomeninges, normal over cortex
{04727} cerebellopontine angle, normal
{07194} trauma chemical injury, brain normal and carbon monoxide 7-4-112
{11369} pons, normal
{11402} vertebral basilar artery, normal
{11405} vertebral basilar artery, normal
{11408} vertebral basilar artery, normal
{12833} internal carotid artery, normal anatomy
{12836} internal carotid artery, normal anatomy
{12839} internal carotid artery, normal anatomy
{01209} neurons
{01224}
{01226}
{01228}
cerebellum
{14597} microglia, normal
{10598} microglia, normal
{14599} microglia, normal
{14600} microglia, normal
{14601} peripheral nerve, normal
{14602} peripheral nerve, normal
{14603} peripheral nerve, normal
{14604} peripheral nerve, normal
{14605} schwann cells, normal
{14606} schwann cells, normal
{14608} nerve, normal
{15061} pineal gland, brain sand
{15062} pineal gland, brain sand
{15063} pineal gland, brain sand
{15064} pineal gland, brain sand
{15146} neuron, nissl substance (rer)
{15153} pyramidal cell, cerebral cortex
{15156} cerebellum, immature
{15157} neuron in a brain stem nucleus, #31 arrow on neuron cell body
{15158} choroid plexus, fetal brain of animal #31
{15159} dorsal root ganglion, #32
{15161} dorsal root ganglion, #32 arrow on bipolar cell
{15165} nerve, normal
{15314} pacinian corpuscle, finger tip
{17663} wernicke's encephalopathy, comparison with normal *mammillary bodies
{17859} brain, normal
{17860} brain, normal
{17861} brain, normal
{17862} brain, normal
{17863} brain, normal
{17864} brain, normal
{17865} brain, normal
{17866} brain, normal
{17872} infarct, brain frontal lobe looks normal
{19970} brain 32 weeks, normal
{19971} brain 32 weeks, normal
{19990} pineal gland with cyst, normal
{20155} brain, normal
{20713} pineal gland, brain sand
{20714} cochlea, normal
{20715} ciliary process, normal eye
{20716} optic nerve head and retina, normal
{20767} cerebral cortex of newborn, arrows in large cells layer v; note columnar arrangement
{20768} pyramidal cell in developing cortex, pial surface is toward bottom
{20769} choroid plexus, newborn
{20770} dorsal root ganglion, reduced silver
{20771} dorsal root ganglion, reduced silver
{20774} perineurium, transverse
{20775} nerve, longitudinal section
{25686} white matter, normal brain
{25687} cerebral cortex, normal
{30242} cranial nerves, normal
{30243} cranial nerves, normal
{30985} internal capsule and corona radiata, normal 1/10
{31018} cerebral cortex, normal
{31024} cerebral cortex, normal
{31027} skull, norm`l
{31030} skull, normal
{31045} posterior fossa, normal anatomy
{31048} vestibulocochlear nerve in cp angle, normal
{31051} cisterna magna and pons, normal brain
{31111} tentorial notch contents, normal
{31174} thalamus, normal
{31210} brain, normal
{31219} brain, normal
{31243} brain, normal
{31330} sella turcica, normal
{31339} brain, normal
{31354} brain, normal
{31358} skull, normal plain anatomy
{31361} skull, normal plain anatomy
{31364} frontal sinus, normal plain anatomy
{31370} lumbar spine anatomy, normal
{31373} lumbar spine anatomy, normal
{31376} lumbar spine anatomy, normal
{31385} lumbar spine anatomy, normal
{31388} lumbar spine anatomy, normal
{31418} internal carotid artery anatomy, normal
{31421} circle of willis anatomy, normal
{31433} venous drainage, brain normal anatomy
{31445} straight sinus joining torcula or * Conflnormal venous anatomy - with arrows
{31451} middle cerebral artery, normal anatomy
{31454} middle cerebral artery, normal anatomy
{31460} internal carotid artery anatomy, normal
{31463} vertebral basilar circulation, normal
{31466} basilar artery, normal
{31469} posterior cerebral artery, normal
{31475} vertebral basilar circulation, normal
{31490} vertebral basilar circulation, normal
{31511} spinal cord, normal
{31517} spinal cord, normal
{31575} down's syndrome, cerebral atrophy/normal
{31583} substantia nigra midbrain, normal
{31589} substantia nigra, normal confusing because melanin isn't black
{31631} caudate, normal histology
{31640} neuron and astrocytes in putamen, normal
{31642} cerebellum, normal & disrupted
{31760} wernicke's encephalopathy, normal mammillary body for comparison
{32912} cavum septum pellucidum, normal
{34331} dorsal root ganglion, normal
{34334} dorsal root ganglion, normal
{34337} dorsal root ganglion, normal
{35819} pineal, normal
{35822} pineal, normal
{35837} area postrema, normal
{35861} cerebral cortex, normal
{35870} neuron, normal cells in caudate
{35876} locus ceruleus, normal
{35915} purkinje cell, normal
{37284} Alzheimer's disease, normal neuron
{37335} caudate, normal for comparison
{37338} Huntington's disease, normal brain on top for comparison
{37500} germinal matrix, normal
{37513} germinal matrix, normal
{37515} germinal matrix, normal
{37609} brain, normal
{37665} brain, normal for comparison
{37678} aqueduct, normal midbrain
{37679} aqueduct, normal
{37680} aqueduct, normal
{40144} brain, normal
{49534} * Cerebellum, normal
{53716} EEG, normal
| New visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if people like me who call ourselves Christians didn't try to act as good as other good people ." Prayer Request

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |
Teaching Pathology
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |
 |
Click here to
see the author prove you can have fun skydiving without being world-class. Click here to see the author's friend, Dr. Ken Savage, do it right. |
